New insights into an innovative Auricularia auricular polysaccharide pH-sensitive hydrogel for controlled protein drug delivery†
Abstract
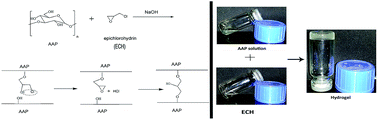
A novel hydrogel based on Auricularia auricular polysaccharide (AAP), was prepared and characterized. AAP hydrogel exhibited a pH-sensitive release of model protein drug (bovine serum albumin, BSA) under simulated gastrointestinal conditions. The results indicate AAP hydrogel has promising potential as an effective vehicle for oral delivery of protein.

 Please wait while we load your content...
Please wait while we load your content...