Open Access Article
Open Access ArticleCreative Commons Attribution 3.0 Unported Licence
Discovery of SARS-CoV-2 main protease inhibitors using a synthesis-directed de novo design model†
Aaron
Morris‡
a,
William
McCorkindale‡
b,
The COVID Moonshot
Consortium
c,
Nir
Drayman
d,
John D.
Chodera
e,
Savaş
Tay
d,
Nir
London
 f and
Alpha A.
Lee
f and
Alpha A.
Lee
 *a
*a
aPostEra Inc, 2 Embarcadero Centre, San Franciso, CA 94111, USA. E-mail: alpha.lee@postera.ai
bDepartment of Physics, University of Cambridge, CB3 0HE, UK
cThe COVID Moonshot Consortium, Web: http://www.postera.ai/covid
dThe Pritzker School for Molecular Engineering, The University of Chicago, Chicago, IL, USA
eComputational and Systems Biology Program Sloan Kettering Institute, Memorial Sloan Kettering Cancer Center, New York, NY 10065, USA
fDepartment of Organic Chemistry, The Weizmann Institute of Science, Rehovot, 76100, Israel
First published on 6th May 2021
Abstract
The SARS-CoV-2 main viral protease (Mpro) is an attractive target for antivirals given its distinctiveness from host proteases, essentiality in the viral life cycle and conservation across coronaviridae. We launched the COVID Moonshot initiative to rapidly develop patent-free antivirals with open science and open data. Here we report the use of machine learning for de novo design, coupled with synthesis route prediction, in our campaign. We discover novel chemical scaffolds active in biochemical and live virus assays, synthesized with model generated routes.
Coronaviruses are a family of pathogens that is frequently associated with serious and highly infectious human diseases, from the common cold to the SARS-CoV pandemic (2003, 774 deaths, 11% fatality rate), MERS-CoV pandemic (2012, 858 deaths, 34% fatality rate) and most recently the COVID-19 pandemic (ongoing pandemic, 1.7 million deaths up to Dec 2020). The main protease (Mpro) is one of the best characterized drug targets for direct-acting antivirals.1,2 Mpro is essential for viral replication and its binding site is distinct from known human proteases, thus inhibitors are unlikely to be toxic.3,4 Moreover, the high degree of conservation across different coronaviruses renders Mpro targeting a fruitful avenue towards pan-cornavirus antivirals.5 To date, most reported Mpro inhibitors are peptidomimetics, covalent, or both.2 Peptidomimetics are challenging to develop into oral therapeutics, and covalent inhibitors incur additional idiosyncratic toxicity risks. We launched the COVID Moonshot consortium in March 2020, aiming to find oral antivirals against COVID-19 in an open-science, patent-free manner.6
Here we report the prospective use of a simple model to rapidly expand hits. Starting from 42 compounds with IC50 within assay dynamic range (<100 μM) and 515 inactives, our model designed 5 new compounds predicted to have higher activity, together with predicted synthetic routes. All designs were were chemically synthesized and experimentally tested, and 3 have measurable activity against Mpro. The top compound has comparable Mpro inhibition to the best in the training set, but with a different scaffold, and is active against the OC43 coronavirus in a live virus assay.
Algorithmic de novo design aims to automatically generate compounds that are chemically diverse, synthetically accessible and biologically active.7 Classic approaches apply heuristics to fragment and modify known active compounds, with the region of chemical space explored and synthetic accessibility constrained by those rules.8,9,10 Recent machine learning approaches explore chemical space in more abstract molecular representation space,11,12 but this often comes at the expense of synthetic accessibility.13 Our approach builds on rule-based fragmentation and molecule generation, but employs a method that combines regression and classification amid noisy data, and use of machine learning to predict synthesis routes. Our model comprises two parts: compound prioritisation and chemical space exploration.
Our compound prioritisation model aims to predict whether a designed compound is likely to be an improvement in activity over the incumbent. However, as is typical in the hit-expansion stage, bioactivity modelling is hindered by insufficient data where the majority of compounds are inactive, and noisy data as measurement variability increases for lower affinity compounds. Thresholding the data and framing the problem as classification of active/inactive would not allow us to rank compounds based on predicted improvement over the incumbent, yet the amount of measured bioactivity data and the measurement noise makes a regression approach challenging.
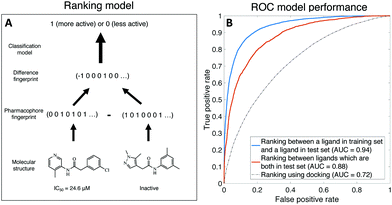
To overcome both challenges, we develop a learning-to-rank framework.14,15 Rather than training a regression model to predict the IC50 of a compound, we instead train a classifier to predict whether a compound is more or less active than another compound, with the input to the model being the difference in molecular descriptors between the molecules (see Fig. 1 for a schematic). This model accounts for both compounds with IC50 measurements and compounds that are simply inactive–active compounds are ranked by their IC50, all inactives with no measurable IC50 are considered less active than active compounds, and inactive–inactive pairs are ignored. Further, we account for noise by only considering IC50 differences amongst actives above 5 μM. We use the FastAI Tabular model,16 with input features generated from concatenated Morgan, Atom Pair, and Topological Torsion fingerprints implemented in RDkit,17 and dataset was randomly split into training (80%) and testing (20%); details about model implementation can be found in ESI† and source code.
Fig. 1 shows that our binary ranking model achieves an AUC of 0.88 (95% CI: [0.83,0.96]) in ranking ligands within the test set, and AUC for 0.94 (95% CI: [0.91,0.98]) where we compare a ligand in the training set against another ligand in the test set; the latter is more relevant as our goal is finding ligands more active than the best incumbent. The 95% confidence interval is computed using bootstrapping. We also compare our model against OpenEye’s FRED hybrid docking mode as implemented in the “Classic OEDocking” floe, a physics-based docking algorithm, on the Orion online platform, which achieves AUC of 0.72; 95% CI: [0.722,0.723] (see ESI† for implementation details). Note that docking does not require ligand bioactivity as training data, thus is not a directly comparison to machine learning. In the ESI† Material, we discuss that our model ranks ligands better than a model that directly learns IC50 (AUC = 0.86; 95% CI: [0.71,0.95]).
Beyond train-test split, model performance can be evaluated from a time-split. Five months have elapsed from the time we deployed our model to select compounds to writing up the manuscript. During that time, the COVID Moonshot Consortium (a team of expert medicinal chemists) has independently designed, synthesised and tested 356 compounds,18 out of which 15% were better than the top 2 compounds (having IC50 comparable within error) in our dataset. Table 1 shows that our model has an enrichment factor of ∼2, i.e. if we rescore the 356 compounds synthesized by the medicinal chemistry team using our model, and pick the top 1%–10% percentile, the proportion of molecules that would be better than the top 2 compounds would be ∼2x higher than human selection.
| Percentile | 1% | 2.5% | 10% |
|---|---|---|---|
| Enrichment factor | 1.7 | 2.3 | 1.7 |
Having demonstrated the accuracy of our ranking model, we now turn to chemical space exploration. We first consider a set of chemically reasonable perturbations (e.g. amide to retroamide, amide to urea), which is applied to the whole set of active molecules. We then fragment along synthetically accessible bonds (e.g. amides and aromatic C–C and C–N), and reconnect the synthons to generate an exhaustive library. The resulting library of 8.8 million generated molecules is scored using our ranking model by the probability of having a higher potency compared to the most potent molecule in the dataset.
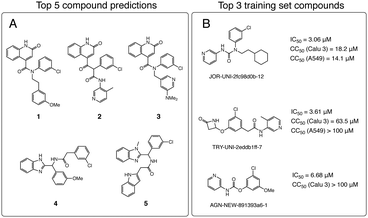
Although virtual “reactions” were used to generate new molecules, the synthons are not necessarily off-the-shelf nor the reactions optimal. As such, we use a retrosynthesis predictor to triage based on synthetic accessibility. We fed top hits into Manifold, our platform for synthesis route prediction (https://postera.ai/manifold). Manifold searches for synthetic routes starting from purchasable molecules. The underlying technology is based on Molecular Transformer, a machine learning model for reaction prediction using sequence-to-sequence translation.19,20 The top 5 molecules with predicted routes <4 steps were synthesised and tested (Fig. 2A). For comparison, the most potent molecules from the training set are shown in Fig. 2B; 1–5 have Tanimoto similarity <0.48 (1024 bit ECFP6) to every molecule in the training set.
Fig. 3 shows that for Compounds 1, 2, 4 and 5 our retrosynthesis algorithm generates successful routes, thus provides a reasonable estimate of synthetic complexity. The syntheses were carried out at the Wuxi AppTec and compounds were assayed as received. Minor variations in building blocks were employed depending on what was readily available. We note that our algorithm failed to estimate the synthetic complexity of Compound 3. The final amide formation step was unexpectedly challenging, and no desired product was seen despite significant efforts in condition screening. Compound 3 was furnished via an alternative strategy, employing an Ullmann coupling to arylate the amide, which was not predicted by our approach.
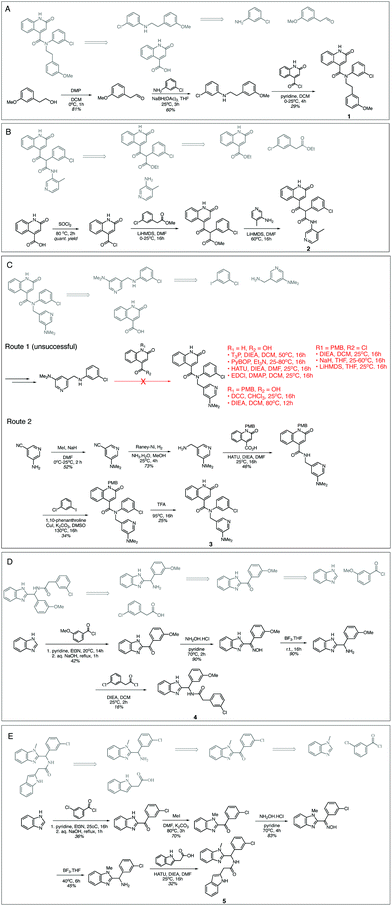 | ||
| Fig. 3 Model generated synthetic schemes that are experimentally validated. Schemes (A–E) show the synthesis schemes generated by our model (grey) and experimental schemes for Compounds 1–5. The ESI† contains experimental procedures provided by our contract research organisation. | ||
Compounds 1–5 were tested for Mpro activity using a fluorescence assay. Fig. 4 shows that Compounds 1–3 have IC50 within assay dynamic range (<100 μM), and Compound 1 has IC50 = 4.1 μM. Compound 1 is further assayed in live virus assays, with the less pathogenic OC43 coronavirus, showing EC50 = 13 μM and is not cytotoxic (CC50 > 100 μM against A549 cell line; CC50 is the concentration required to cause 50% cell death). We employ OC43 as a rapid surrogate assay for SARS-CoV-2 as the former can be done in a BSL-2 rather than BSL-3 lab. Interestingly, the top non-cytotoxic hit of the training set (TRY-UNI-2eddb1ff-7) does not show OC43 activity, showcasing the utility of using generative models to suggest new scaffolds with complementary physicochemical properties.
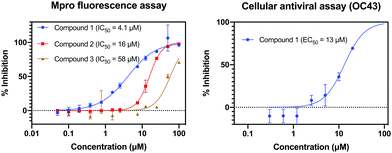 | ||
| Fig. 4 Three compounds generated using our synthesis-directed model exhibit Mpro activity. Our most active compound has measurable antiviral activity against the OC43 coronavirus and no measurable cytotoxic effect (CC50(A549) > 100 μM). 95% CI: IC50 (Mpro)–Compound 1 [3.42,4.86] μM, Compound 2 [15.1,16.5] μM, Compound 3 [48.8,69.4] μM; EC50 (OC43)–Compound 1 [10.1, 18.4] μM. See ESI† for assay details. | ||
In summary, we demonstrated the utility of a de novo design model, guided by estimation of synthetic complexity, for generating ideas in hit expansion. At the time of writing, the quinolone series is undergoing optimisation by the COVID Moonshot initiative (https://postera.ai/covid). Data for Compound 1–5 is registered as the ALP-POS-ddb41b15 series on the Moonshot platform.
J. D. C. acknowledges support from NIH grants P30 CA008748 and GM124270. W. M. acknowledges the support of the Gates Cambridge Trust.
Conflicts of interest
A. M. and A. A. L. are co-founders and shareholders of PostEra (https://postera.ai). J. D. C is a current member of the Scientific Advisory Board of OpenEye Scientific Software, Interline Therapeutics, and Redesign Science. The Chodera laboratory receives or has received funding from multiple sources,including the National Institutes of Health, the National Science Foundation, the Parker Institute for Cancer Immunotherapy, Relay Therapeutics, Entasis Therapeutics, Silicon Therapeutics, Interline Therapeutics, EMD Serono (Merck KGaA), AstraZeneca, Vir Biotechnology, Bayer, XtalPi, the Molecular Sciences Software Institute, the Starr Cancer Consortium, the Open Force Field Consortium, Cycle for Survival, a Louis V. Gerstner Young Investigator Award, and the Sloan Kettering Institute. A complete funding history for the Chodera lab can be found at http://choderalab.org/funding.Notes and references
- T. Pillaiyar, M. Manickam, V. Namasivayam, Y. Hayashi and S.-H. Jung, J. Med. Chem., 2016, 59, 6595–6628 CrossRef CAS PubMed.
- R. Cannalire, C. Cerchia, A. R. Beccari, F. S. Di Leva and V. Summa, J. Med. Chem., 2020 DOI:10.1021/acs.jmedchem.0c01140.
- Z. Jin, X. Du, Y. Xu, Y. Deng, M. Liu, Y. Zhao, B. Zhang, X. Li, L. Zhang and C. Peng, et al. , Nature, 2020, 582, 289–293 CrossRef CAS PubMed.
- Y. Liu, C. Liang, L. Xin, X. Ren, L. Tian, X. Ju, H. Li, Y. Wang, Q. Zhao and H. Liu, et al. , Eur. J. Med. Chem., 2020, 112711 CrossRef CAS PubMed.
- S. Ullrich and C. Nitsche, Bioorg. Med. Chem. Lett., 2020, 127377 CrossRef CAS PubMed.
- J. Chodera, A. A. Lee, N. London and F. von Delft, Nat. Chem., 2020, 12, 581 CrossRef CAS PubMed.
- P. Schneider and G. Schneider, J. Med. Chem., 2016, 59, 4077–4086 CrossRef CAS PubMed.
- N. Brown, B. McKay, F. Gilardoni and J. Gasteiger, J. Chem. Inf. Comput. Sci., 2004, 44, 1079–1087 CrossRef CAS PubMed.
- H. Patel, M. J. Bodkin, B. Chen and V. J. Gillet, J. Chem. Inf. Model., 2009, 49, 1163–1184 CrossRef CAS PubMed.
- M. Hartenfeller, H. Zettl, M. Walter, M. Rupp, F. Reisen, E. Proschak, S. Weggen, H. Stark and G. Schneider, PLoS Comput. Biol., 2012, 8, e1002380 CrossRef CAS PubMed.
- R. Gómez-Bombarelli, J. N. Wei, D. Duvenaud, J. M. Hernández-Lobato, B. Sánchez-Lengeling, D. Sheberla, J. Aguilera-Iparraguirre, T. D. Hirzel, R. P. Adams and A. Aspuru-Guzik, ACS Cent. Sci., 2018, 4, 268–276 CrossRef PubMed.
- M. H. Segler, T. Kogej, C. Tyrchan and M. P. Waller, ACS Cent. Sci., 2018, 4, 120–131 CrossRef CAS PubMed.
- W. Gao and C. W. Coley, J. Chem. Inf. Model., 2020, 60(12), 5714–5723 CrossRef CAS PubMed.
- N. P. Duffy, Molecular property modeling using ranking, US Pat., 7702467, 2010 Search PubMed.
- S. Agarwal, D. Dugar and S. Sengupta, J. Chem. Inf. Model., 2010, 50, 716–731 CrossRef CAS PubMed.
- J. Howard et al. , http://fastai,https://github.com/fastai/fastai, 2018.
- RDKit: Open-Source Cheminformatics Software, https://www.rdkit.org Search PubMed.
- The COVID Moonshot Consortium, bioRxiv, DOI:10.1101/2020.10.29.339317, 2020.
- A. A. Lee, Q. Yang, V. Sresht, P. Bolgar, X. Hou, J. L. Klug-McLeod and C. R. Butler, et al. , Chem. Commun., 2019, 55, 12152–12155 RSC.
- P. Schwaller, T. Laino, T. Gaudin, P. Bolgar, C. A. Hunter, C. Bekas and A. A. Lee, ACS Cent. Sci., 2019, 5, 1572–1583 CrossRef CAS PubMed.
Footnotes |
| † Electronic supplementary information (ESI) available: Experimental and assay details, and the full list of contributors in the COVID Moonshot Consortium. Our training set, de novo design method and generated molecules are available on https://github.com/wjm41/mpro-rank-gen. See DOI: 10.1039/d1cc00050k |
| ‡ These authors contributed equally to this work. |
| This journal is © The Royal Society of Chemistry 2021 |