Mesenchymal stem cell-derived microvesicles mediate BMP2 gene delivery and enhance bone regeneration†
Abstract
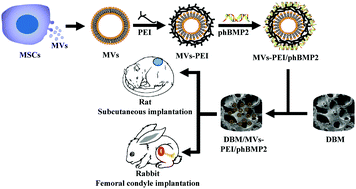
A demineralized bone matrix (DBM) scaffold has good biocompatibility, low antigenicity, a natural porous structure and no cytotoxicity, and so it is an appropriate material for bone regeneration. However, osteoinductive growth factors are often removed during preparation, which destroys the osteoinductive capacity of the DBM scaffold. Biomaterials combined with gene therapy is a promising approach to effectively avoid this adverse side effect. This study develops a human bone morphogenetic protein 2 (hBMP2) gene-activated DBM scaffold to enhance the osteoinductive capacity of DBM and improve bone repair. Bone marrow mesenchymal stem cell (MSC)-derived microvesicles (MVs) were obtained, and polyethyleneimine (PEI) and human bone morphogenetic protein 2 (hBMP2) plasmids (phBMP2) were sequentially coated on the MVs by layer-by-layer (LBL) self-assembly to form an MVs–PEI/phBMP2 non-viral gene vector. Finally, the gene-activated scaffold (DBM/MVs–PEI/phBMP2) was prepared by loading MVs–PEI/phBMP2 onto a DBM scaffold. The experimental results show that the MVs–PEI/phBMP2 exhibits higher transfection efficiency and lower cytotoxicity to MSCs when the MVs/PEI weight ratio = 5, and could enhance the osteogenic differentiation of MSCs in vitro. Subcutaneous implantation into rats showed that the DBM/MVs–PEI/phBMP2 scaffold could efficiently enhance the deposition of: collagen fibers, osteocalcin, osteopontin and CD34 endogenous proteins. Rabbit femoral condyle defect experiments proved that the DBM/MVs–PEI/phBMP2 scaffold could significantly promote bone repair. This study presents a novel, highly efficient and low cytotoxicity gene delivery vector based on MVs. The gene-activated DBM scaffold based on MVs not only could promote bone formation but also angiogenesis, implying that this kind of gene-activated scaffold is a promising bone substitute material.


 Please wait while we load your content...
Please wait while we load your content...