Bismuth drugs tackle Porphyromonas gingivalis and attune cytokine response in human cells†
Abstract
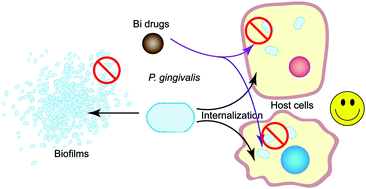
Periodontitis is the leading cause of severe tooth loss and edentulism in adults worldwide and is closely linked to systemic conditions such as diabetes and cardiovascular disease. Porphyromonas gingivalis is the key pathogen in periodontitis. Herein, we provided the first evidence that bismuth drugs suppress P. gingivalis in its planktonic, biofilm, and intracellular states. In total, 42 bismuth-associated proteins were identified including its major virulent factors (e.g., gingipains, hemagglutinin HagA, and fimbriae). Bismuth perturbed its iron acquisition, disturbed the energy metabolism and virulence, and deactivated multiple key enzymes (e.g., superoxide dismutase and thioredoxins). Moreover, bismuth inhibited its biofilm formation and disrupted the 3-day matured biofilms. Notably, the internalized P. gingivalis in various human cells (e.g., human gingival epithelium progenitors, HGEPs) was oppressed by bismuth but not the commonly used antibiotic metronidazole. Importantly, bismuth drugs enabled the counteraction of immuno-inflammatory responses in different host cells perturbed by P. gingivalis. The production of IL-6 and IL-8 attenuated by P. gingivalis in both of native and IL-1β-stimulated HGEPs was restored, while the bacterium-enhanced expression of IL-6, IL-1β, and TNFα in THP-1 macrophages was alleviated. This proof-of-concept study brings prospects for the potential reposition of the routinely used anti-Helicobacter pylori bismuth drugs to better manage inflammatory diseases such as periodontitis and P. gingivalis-related complex systemic disorders.


 Please wait while we load your content...
Please wait while we load your content...