Gut : liver : brain axis: the microbial challenge in the hepatic encephalopathy
Abstract
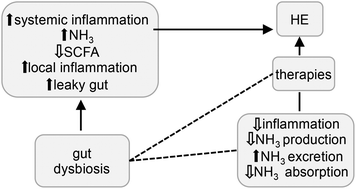
Hepatic encephalopathy (HE) is a debilitating neuropsychiatric condition often associated with acute liver failure or cirrhosis. Advanced liver diseases are characterized by a leaky gut and systemic inflammation. There is strong evidence that the pathogenesis of HE is linked to a dysbiotic gut microbiota and to harmful microbial by-products, such as ammonia, indoles, oxindoles and endotoxins. Increased concentrations of these toxic metabolites together with the inability of the diseased liver to clear such products is thought to play an important patho-ethiological role. Current first line clinical treatments target microbiota dysbiosis by decreasing the counts of pathogenic bacteria, blood endotoxemia and ammonia levels. This review will focus on the role of the gut microbiota and its metabolism in HE and advanced cirrhosis. It will critically assess data from different clinical trials measuring the efficacy of the prebiotic lactulose, the probiotic VSL#3 and the antibiotic rifaximin in treating HE and advanced cirrhosis, through gut microbiota modulation. Additionally data from Randomised Controlled Trials using pre-, pro- and synbiotic will be also considered by reporting meta-analysis studies. The large amount of existing data showed that HE is a clear example of how an altered gut microbiota homeostasis can influence and impact on physiological functions outside the intestine, with implication for host health at the systems level. Nevertheless, a strong effort should be made to increase the information on gut microbiota ecology and its metabolic function in liver diseases and HE.

 Please wait while we load your content...
Please wait while we load your content...