Effect of diselenide administration in thioacetamide-induced acute neurological and hepatic failure in mice
Abstract
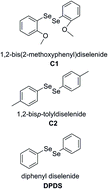
Hepatic encephalopathy is a common complication of severe acute hepatic failure and has been associated with high short-term mortality rates. Therefore, the aim of this study was to investigate the effect of diphenyl diselenide (DPDS) and its analogues in protecting against thioacetamide (TAA)-induced acute neurological and hepatic failure in mice. The animals received a TAA dose of 200 mg kg−1 intraperitoneally, and then, 1 hour later, they received 15.6 mg kg−1 of diselenides intraperitoneally. Twenty three hours after diselenide administration, the animals were sacrificed, and blood, brain and liver samples were collected for analysis. The results showed that mice exposed to TAA presented oxidative stress characteristics, such as an increase in lipid peroxidation (LPO), enhanced glutathione peroxidase activity and a decrease in the GSH/GSSH ratio in the brain and liver. In addition, the TAA group showed a decrease in cellular viability in both tissues. TAA treatments also generate reactive oxygen species and cause inhibition of glutathione-S-transferase in liver, which were associated with TAA exacerbated half-life in this tissue. In the histopathological analyses, we observed that TAA induced a large inflammation process that was confirmed according to the elevation of liver myeloperoxidase activity. Moreover, the treatment with diselenides reduced the oxidative stress significantly. Additionally, after the establishment of acute hepatic failure (AHF), DPDS was able to inhibit the inflammatory processes with a more significant decrease in major hepatic damage effects than was presented after treatment with its analogues. Thus, our results showed that DPDS is a promising therapeutic option for the treatment of AHF and hepatic encephalopathy as mice returned to normal conditions after the damage.
- This article is part of the themed collection: New Talents

 Please wait while we load your content...
Please wait while we load your content...