Changes in breath carbon isotope composition as a potential biomarker of inflammatory acute phase response in mechanically ventilated pediatric patients†‡
Abstract
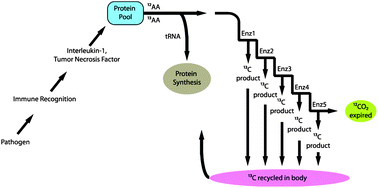
Sepsis is a leading cause of mortality in intensive care units. Animal studies have shown exhaled breath carbon isotope delta values (BDVs, i.e., 13CO2/12CO2 delta value) to be a marker for the inflammatory acute phase response (APR). The purpose of this study was to determine the baseline variability of BDVs in mechanically ventilated pediatric patients with and without systemic inflammatory response syndrome (SIRS) and to correlate the BDV with clinical course over time. The study was an observational pilot study in a pediatric intensive care unit at an urban, tertiary care children's hospital. Seventeen mechanically ventilated pediatric patients underwent measurement of exhaled BDVs every 8 hours for 72 hours. The BDV was not statistically different between SIRS, No-SIRS and SIRS with shock. The mean BDV was significantly lower in subjects with active sepsis or trauma/post-op status compared to subjects with No-Infection/Trauma/Surgery (No-ITS) or septic shock. Trend analysis over time revealed that the No-ITS and ITS in recovery groups had positive slopes. Subjects who developed infections during the study and subjects who underwent shock had a negative trend over time. These results indicate that the BDV does not correlate well with the SIRS status. However, when patients are classified based on their inflammatory APR the BDV correlates with the severity of systemic inflammation. When monitored over time, changes in the BDV may correlate with changes in physiology related to fractionation during the APR to infection, trauma or due to altered macronutrient oxidation during episodes of septic shock.
- This article is part of the themed collection: Novel stable isotopes in health sciences
 Please wait while we load your content...
Please wait while we load your content...