Sun exposure of indoor workers in the UK – survey on the time spent outdoors
K. A.
Baczynska
 *,
M.
Khazova
and
J. B.
O'Hagan
*,
M.
Khazova
and
J. B.
O'Hagan
Centre for Radiation, Chemical and Environmental Hazards, Public Health England, Chilton, Didcot, Oxfordshire, UK. E-mail: Katarzyna.baczynska@phe.gov.uk
First published on 24th October 2018
Abstract
Assessment of ultraviolet (UV) exposure is essential for evaluation of the risks and benefits to optimise public health outcomes. The exposure depends on available environmental UV radiation and individual behaviour, and it can be obtained from dosimetry studies; however, the use of dosimeters is often not feasible for large population groups or over long periods of time. In this study, a lifestyle questionnaire has been used to obtain information on the time spent outdoors by indoor workers that could be used in combination with dosimetry studies in smaller targeted groups to quantify UV exposure for health risk/benefit analysis. 894 office and laboratory workers at the Public Health England, UK, responded to the survey. Questions addressed the time of day and the duration of time; staff were outdoors on weekdays, at weekends and during holidays. The majority of the responders spent negligible time outdoors on weekdays. Outdoor activities before and after work were constrained by the work pattern and commuting. The average time for those who go outdoors before and after commuting was 22.5 ± 16.2 min and 30.4 ± 21.4 min, respectively. Only 7% of participants regularly spent their lunch break outdoors for 21.5 ± 12.2 min and weekday exposure may contribute less than 13% of the daily available erythema dose. At the weekend, on average responders spend 5.0 ± 2.6 h outdoors over the two days: if taken around midday, it accounts for approximately 50% of available UV exposure. In winter months in the UK, November to March, the combination of very low environmental UV and low ambient temperatures results in negligible UV exposure. Holidays contributed to the majority of the annual UV exposure. In summer, 45% of responders went to destinations where the UV levels may be up to 2 times higher than in the UK; durations of overseas holidays are also longer than UK breaks. The UV dose from two weeks of holiday in extreme UV index level destinations could be comparable to a 1.5–2 summer months holiday in the UK. The survey data were validated with 6 months of dosimetry within the same cohort; very strong and strong correlation was found between the survey and measurements. This shows that a lifestyle survey can be used in combination with targeted dosimetry studies in small groups to obtain information about the time spent outdoors.
Introduction
There is consensus in the international community that UV radiation can cause considerable damage to the skin and the eye, increase the risk of skin cancers and suppress adaptive immunity.1 Established and emerging health benefits from sun exposure include cutaneous vitamin D synthesis, as well as its role in blood pressure modulation, cardiovascular health, and melatonin and serotonin regulation for mood and cognition.2 This suggests that inadequate sun exposure carries its own risks, affecting life expectancy and the quality of life and may present a significant burden to health services; it calls for a balanced approach to UV exposure for optimum human health. Adults spend up to 30–45 years working and inadequate UV exposure could have long lasting health implication while working and in retirement.Understanding personal UV exposure is essential for evaluation of the risks and benefits to optimise public health outcomes. Personal UV exposure depends on available ambient levels that change with latitude and altitude, the time of year, the time of day, meteorological conditions and an individual's behaviour.3 This information can be obtained by UV dosimetry, but direct measurements often are not feasible for large population groups or over long periods of time. There are a number of publications that reported UV exposure during recreational activities in Oceania, the tropics and the south of Europe,4–13 in countries with extreme and very high UV levels. These data could act as a proxy for the exposure of British holiday makers in those locations undertaking the same range of activities. Weekday and weekend exposures in the UK are very different; the daily schedule is governed by work patterns and lifestyle. Furthermore, as the erythema doses depend on ambient UV radiation, these results cannot be directly used in the UK; such an analysis is complicated further by the variability of British weather and lower temperatures, both affecting the exposed body area.
Very few studies described sun exposure during weekdays and weekends in the UK14,15 and they are limited to specific small groups; crucially, timing of exposure is not reported. The extensive studies of personal UV dosimetry in Denmark16 for weekdays and weekends cannot be extrapolated for the UK either; although the anticipated UV Index (UVI) in Scandinavia is similar to the UK, cultural differences, working practices and more variability of British weather may affect accumulated exposures. National health and wellbeing publications provide some insight into the time spent outdoors. However, these lifestyle surveys often focus on a particular activity like cycling to work17–21 and don't give detailed information on the overall daily time outdoors.
The aim of this study was to test the feasibility of using a lifestyle questionnaire to quantify the time spent outdoors that, in combination with dosimetry in smaller targeted groups, would provide information on UV exposure. A similar approach was successfully implemented in the large population study DGUV FB-181 of German outdoor workers22–24 for the assessment of long-term occupational UV exposure.
Methods and materials
In this study, office and laboratory workers at Public Health England (PHE), UK, were asked to complete a questionnaire about the time spent outdoors. The research study approval was granted by the PHE Research Ethics and Governance Group.PHE is a government organisation that employs 5409 scientists, researchers, public health professionals and administrative staff (number valid for summer 2017). All PHE employees fall into these categories and could be considered as office or laboratory staff. PHE has a number of centres across the UK including Wales, England, Northern Ireland and Scotland; the majority of employees are located in the south of England and London.
The full-time working week at PHE is 37.5 h, with core working hours 10:00–12:00 and 14:00–16:00. This allows a flexible start and end of the day, with a lunch break of minimum 30 min to maximum 2 h taken between 12:00 and 14:00.
A pre-tested on-line based survey was available on an intranet for PHE employees. The invitation for participation was included in the PHE Weekly Newsletter on the launch on 15 June 2017, followed by a reminder one week before closure. The survey was live on the intranet for 4 weeks. Due to organisational restrictions it was not possible to approach employees personally and/or send the survey link via E-mail.
The questionnaire consisted of 12 questions (Q1 to Q12) about the time spent outdoors on weekdays, weekends and holidays:
• Q1 and Q6. Do you spend any time outdoors before or after commuting to/from work, i.e. none, up to 30 min, 30–60 min, 60–90 min and more than 90 min?
• Q2. How do you commute, i.e. driving, cycling, walking, public transport and other? What time do you leave home/work, i.e. before 8:00, 8:00–9:00, 9:00–10:00 and after 10:00/before 16:00, 16:00–17:00, 17:00–18:00 and after 18:00 and how long do you commute each way (open question)?
• Q3. How often do you spend lunch break outdoors, i.e. never, occasionally, once, twice, three or four times a week?
• Q4. How long do you spend outdoors at lunch break, i.e. less than 15 min, 15–30 min, 30–45 min, 45–60 min, more than 60 min?
• Q5. What do you do, i.e. walking/jogging, cycling and playing sports?
• Q7. On a typical two-day weekend, how much time in total do you spend outdoors, i.e. less than 2 h, 2–4 h, 4–6 h, 6–8 h, 8–10 h, more than 10 h?
• Q8. What are your main outdoor activities during weekends, i.e. camping, cycling, jogging, walking, dog walking, gardening, playing sports, watching sports, spending time with children, outdoor festivals/visiting theme parks, rock climbing, flying aircraft or gliders, BBQ/picnic and others?
• Q9. In the past year, how many days did you spend on holiday and where did you go in June–August, September and October, November–March and April and May? For example, June–August: Italy 7 days, UK 3 days
• 10. What is your gender?
• Q11. What is your age group, i.e. under 25, 25–45, 46–60 and 60+ years old?
• Q12. In which region do you work, i.e. England, Wales, Scotland and Northern Ireland?
To calculate the average time, the middle value of each range was used and only data for participants who stated that they spent time outdoors were included in calculations.
The chi-square test of independence25 was used to test null hypothesis for gender and age.
Holiday seasons were defined as UK summer (June–August), autumn (September–October), winter (November–March) and spring (April–May), based on a combination of environmental UVI and ambient temperature governing people's exposure.
The holiday destinations were grouped according to the maximum UVI levels: extreme (11+), very high (8–10), high (6–7), moderate (3–5), low (<3) and snow sport destinations for each given season.26–29
Sixteen participants from the same cohort wore dosimeters (Scienterra Ltd, Oamaru, New Zealand) from April to September 2017 to record erythema effective irradiance in 30 s intervals. The participants also were asked to complete the questionnaire.
Dosimetry data were used to calculate the time outdoors before/after commuting to work, at lunch break and during good-weather weekends. The non-parametric Spearman rank correlation analysis was used to analyse the rank association between survey and dosimetry data. The degree of correlation was rated as very weak (rs = 0–0.19), weak (rs = 0.2–0.39), moderate (rs = 0.40–0.79), strong (rs = 0.8–0.79) and very strong (rs = 0.8–1.0).25
Results and discussion
Survey
A total of 894 staff members responded to the survey which resulted in a response rate of 16%. It was recognised that a 16% response rate may not be representative as it was not possible to ascertain how many employees were actually aware of the survey (i.e. read the announcement in PHE news). Information on employees’ attendance at the time of the survey also was not available. The total number of employees included those on long-term leave (maternity, sickness, holidays, sabbaticals), away from the office on business, field trips or secondment during this period. A low response rate is of great concern especially since this study was conducted in a public health organisation where workers were likely to be better informed and more engaged. Approaching participants through employers is a useful route. However, the format of the intranet-based survey needs further investigation to improve uptake. Wider publicity, a dedicated survey launch with presentations and a personal approach by E-mail may improve the response rate. Furthermore, the number of responses to a particular question varied and this could indicate the complexity or ambiguity of this question. The question about commuting was particularly affected and the number of responses dropped to 494.The responders were from the following age groups. The PHE staff age-profile data are given in brackets:
• 39% – 25–45 years old (PHE 50%),
• 49% – 46–60 years old (PHE 39%),
• 5% – younger than 25 years old (PHE 4%),
• 5% – older than 60 years old (PHE 7%).
74% of responders were women (PHE 68%), mostly from England, and
• 68% of responders were full time workers,
• 17% worked 4 days a week and
• 10% worked 3 days a week.
The type of part time arrangements has not been confirmed and could be either reduced or compressed hours, or homeworking arrangements.
The erythema effective radiant doses (given in a standard erythema dose, SED) on a clear sky day were calculated over different times of the day for four seasons at Chilton (51.57°N; −1.32°W), using the PHE solar monitoring network data,30 and are listed in Table 1. In addition, the total daily doses were calculated for summer at Chilton, Glasgow (55.86°N; 4.34°E) and Cyprus (34.59°N; 32.99°E) for a very good weather and more representative summer weeks. These data will be used for the discussion of the results.
| Duration | Timing | April | May | July | September |
|---|---|---|---|---|---|
| 30 min | 7:30–8:00 | 0.19 (1%) | 0.3 (1%) | 0.3 (1%) | 0.0 (0%) |
| 30 min | 17:00–17:30 | 0.2 (1%) | 0.5 (2%) | 0.7 (2%) | 0.1 (0%) |
| 30 min | 12:00–12:30 | 1.5 (8%) | 2.3 (8%) | 2.9 (8%) | 1.3 (9%) |
| 2 h | 12:00–14:00 | 6.1 (33%) | 9.3 (31%) | 11.9 (31%) | 9.3 (66%) |
| 4 h | 11:00–15:00 | 11.3 (62%) | 17.6 (58%) | 22.5 (58%) | 9.3 (66%) |
| 6 h | 10:00–16:00 | 15.1 (82%) | 23.9 (79%) | 30.6 (79%) | 12.1 (87%) |
| 8 h | 9:00–17:00 | 17.4 (95%) | 28.2 (93%) | 35.9 (93%) | 13.5 (97%) |
| 10 h | 8:00–18:00 | 18.4 (100%) | 30.4 (100%) | 38.8 (100%) | 14.0 (100%) |
Vertically orientated receiving surfaces with randomly changing azimuth (human body) may receive around 30% of the radiation measured on a horizontal plane,31 which reduces the UV dose listed in Table 1. Small exposed body areas, as generally happens when there are low ambient temperatures, further decrease the erythema exposure doses.
Weekdays
Morning and afternoon weekday time outdoors was linked to the work pattern and commuting constraints: see Table 2.| Morning commute | % of responders (n = 422) | Evening commute | % of responders (n = 443) |
|---|---|---|---|
| Before 08:00 | 62.6 | Before 16:00 | 8.0 |
| 08:00–09:00 | 37.0 | 16:00–17:00 | 35.4 |
| 09:00–10:00 | 0.0 | 17:00–18:00 | 45.3 |
| After 10:00 | 0.4 | After 18:00 | 11.3 |
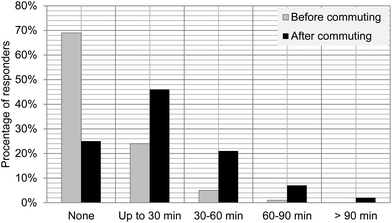
Only 30% of respondents reported going outdoors before commuting, as shown in Fig. 1. The average time spent outdoors before commuting to work was 22.5 ± 16.2 min (n = 273; middle values of the categories “<7.5 min” and “>60 min” were 15 and 60 min, respectively).
More than 60% (n = 264) of participants commute before 8 am. The time spent outdoors before commuting for this group of people cannot result in more than 0.3% of the available daily exposure.
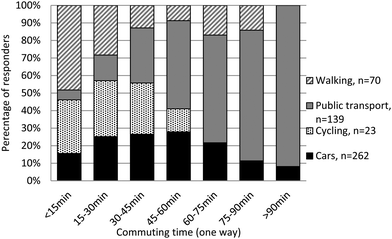
75% of responders (n = 650) spent 30.4 ± 21.4 min outdoors after work. However, 56.6% of responders leave the office after 17:00, see Table 2, and this time doesn't noticeably contribute to daily exposure. Eight percent commute before 16:00, only half of them arrive home in 30 min (see Fig. 2) or less, and nearly ¾ of them would spend some time outdoors after that. Therefore, for only 3.0% of all responders the after-work time outdoors may have a perceptible contribution to accumulative weekly dose. No correlations were found between gender or age and time outdoors before (p = 0.26 and p = 0.41, respectively) and after commuting (p = 0.52 and p = 0.95, respectively). The time spent outdoors was independent of the commuting duration but it was significantly dependent on the timing of the commute in the morning. Responders who commute before 8:00 spent less time outdoors (p = 0.025). Cars and public transport were used by 81% (n = 401) of responders to commute, and for this group commuting does not contribute to the daily erythema UV exposure since the vehicle's window glass blocks short wavelength UV. As illustrated in Fig. 2, more people were commuting longer by public transport.
Walking or cycling provides less than 1% of daily exposure when commuting before 8:00. Only 4 responders cycled or walked to/from work after 10:00 or before 16:00. Walking or cycling is also generally of shorter duration than other modes of transport. The small exposed body area while commuting and lower ambient temperatures in the morning further reduce the possible erythema exposure. The morning and evening contribution of the outdoor time to total daily UV exposure did not exceed 3.5% of the daily erythema dose.
It should be noted that commuting before 8:00 in winter also reduces morning light exposure for circadian entrainment for those with no access to daylight in the workplace.
The majority of sun exposure on a weekday comes from the lunch break. However, only 11% of responders always go outdoors during the lunch break, as shown in Fig. 3. 72% and 34% are walking/jogging and sitting, respectively, with 2% and 1% playing group sports and cycling. Spending time outdoors during the lunch break was independent of gender and age (p = 0.23 and p = 0.19, respectively); the average time was 21.5 ± 12.2 min (n = 710; middle values of the categories “<7.5 min” and “>60 min” were 15 min and 60 min). As illustrated in Table 1, a 30 min lunch break could contribute up to 10% of the total daily available erythema dose in a sunny day. Only 21% of responders who reported spending lunch time outdoors did so for more than 30 min.
 | ||
| Fig. 3 Frequency per week (n = 893) (a) and duration per day (b) of lunch time spent outdoors (n = 710, participants who do not spent time outdoors do not answer this question). | ||
53% of responders never or rarely go outdoors and some people commented that they do not really have a lunch break, just having lunch in front of the computer. One of the free-text comments to the survey stated: “Very little opportunity to spend time outside at lunch times during past year; since when time was available, it was usually cold and cloudy, or raining”. Another wrote: “I spend significantly more time outdoors at lunchtime in the summer (around 1 h) than I do in the winter (around 15 min typically). I do not go outside after work in the darker months – October–March, I spend all winter inside”.
Combined lunch time and morning/evening outdoor time with a mean of 71.4 min from this survey suggests that an individual could receive 10–13% of the available daily erythema dose. In comparison, indoor workers in Denmark received a median of 12–22% of their total UVR dose on workdays.16 Current survey data are on a lower end of the Danish distribution, and this would only be for the 11% minority who always spent lunch time outdoors. Such a difference may be explained by the observation that the typical duration of lunch break of PHE employees may be shorter than that in the Danish study.
The high variability of the British weather results in a significantly lower accumulated erythema dose than may be expected from Table 1. Furthermore, the body area exposed at the lunch break in a workplace is likely to be limited to the arms and face only. Facial skin care products with UV blockers further reduce face exposure.
In winter months in the UK, November to March, the combination of very low environmental erythema irradiance and the low ambient temperatures results in negligible exposure on weekdays.
Weekends
At the weekends, the majority of the responders spent 2 h or more outdoors over the two days as shown in Table 3. Therefore, erythema exposure is higher in the weekend than in weekdays in the same season. The time spent outdoors is longer and is likely to happen between 10:00–16:00 with more body area exposed when walking, gardening, BBQ/picnic and spending time with children as the reported main activities. On high UVI level days, sun protection may be required to avoid sunburn.| Time spent outdoors | <2 h | 2–4 h | 4–6 h | 6–8 h | 8–10 h | >10 h |
|---|---|---|---|---|---|---|
| Percentage of responders | 13% | 26% | 29% | 18% | 10% | 6% |
At the weekend, 13 and 29% of responders spent up to 2 h and up to 4 h outdoors per weekend, respectively, and 51% more than 4 h. Mean times spent outdoors over the two weekend days were calculated taking the middle value of each range to be 5.0 ± 2.6 h (n = 878) (middle values of the categories “<2 h” and “>10 h” were 1 h and 10 h, respectively). The time spent outdoors was independent of gender and age (p = 0.50 and p = 0.85, respectively).
If the time outdoors is taken around midday, it accounts for approximately 50% of the available daily erythema exposure. These results are consistent with the previous studies of weekend exposure in the UK;32 reported mean 2 ± 0.3 h per day for summer weekend exposure and the questionnaire of15 returned 5.2 ± 2.2 h weekend exposures of the healthy group of study participants.
Similar to weekdays, in winter months in the UK the combination of very low environmental UV and low ambient temperatures results in negligible erythema exposure at weekends.
It should also be noted that the results reported here describe the time spent outdoors on weekdays and weekends from April to October on rain-free days. The average time spent outdoors greatly depends on the weather and it changes with seasons. This has been captured by the comments of responders that their time outdoors is significantly reduced or they do not go outdoors at all in winter months.
Holidays
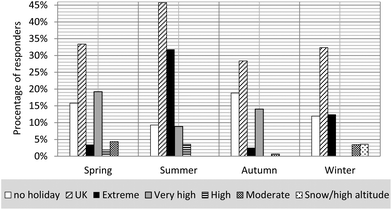
The number of days spent on holiday and the destinations vary depending on the season. The majority of responders take their holiday in summer as shown in Fig. 4. 9.3% of responders (n = 70) declared that that they did not take holidays in summer. 45.8% of responders (n = 345) spent summer holidays in the UK and 40.7% (n = 302) went to extreme and very high UVI level destinations. The most often chosen overseas destinations were Southern Europe and the Mediterranean. One responder spent 16 days in Tibet and Nepal at high altitude, 5 responders went to Australia (9–29 days) and South Africa (14–21 days), but these happened in the UK summer when the UVIs are relatively low in the southern hemisphere.Summer
Although the maximum UVI levels in the UK in summer (UVI = 8) would classify it as very high, a day with such high UV levels is a rare event and it doesn't happen every year.30 The maximum UVI in Southern Europe and the Mediterranean in summer may be up to 50% higher. Combined with the much higher probability of prolonged periods of good weather in this region, as opposed to the variability of British summers, the holiday exposure overseas is likely to be significantly higher than the direct comparison of the maximum UVI may suggest. Using PHE's solar monitoring data, it was estimated that the exposure dose over 7 days of holidays in good weather in the south of England is ∼60% lower than that in Cyprus. However, it may be less than 50% in a more representative week. Further north in the UK, this difference in erythema dose may be as high as a factor of 3, whereas the maximum difference of UVI is ∼ 1.6.31.84% of responders (n = 240) spent their holidays in countries where the UV Index was 11+. The duration of the holidays in the extreme UVI level destinations peaks at 14 days, with 5% of responders (n = 12) spending 21 days and one responder spending 70 days, whereas UK holiday breaks are generally shorter, generally peaking at either 7 or 14 days. Taking these facts together with 1.4–2 times higher maximum UVI, likely prolonged periods of good weather and an outdoor lifestyle, holiday exposure of this group may be 3–5 times higher than over a similar period in the UK. In other words, the UV exposure dose from two weeks of overseas summer holidays in extreme UVI levels may be comparable to 1.5–2 months of summer holidays in the UK.
It is estimated that for Northern European populations, up to one quarter of the annual UVR exposure can occur during two weeks of sun holidays in Southern Europe. The mean accumulated UV dose of the Danish sun seekers in Tenerife was 56.5 SED measured on the wrist,33 and 6 days of such holidays constituted 40% of the annual erythema dose received on average by a Danish indoor worker. In ref. 4, the UV dose of tourists at the Great Barrier Reef snorkelling excursion in spring and summer months was 1.5 SED/10 min on the neck and 0.6 SED/10 min on the back.
Autumn
During September–October, 28.4% of the responders (n = 142) did not have holidays and 29.2% (n = 214) spent holidays in the UK, with durations that peaked between 5 and 7 days. In the autumn, UVI levels in the UK are in decline from the beginning of August.34 They decrease to 50% in the middle of September and to 10–20% in October compared with summer time. Decreasing ambient temperature also affect the exposed body area and erythema exposure during a week-long UK break at this time of the year is lower than in a single day of a summer weekend.2.5% of responders (n = 19) went to extreme (for 10, 14, 21 and 27 days) and high (for 7 and 14 days) UVI destinations in the autumn. Overseas holidays in the autumn are generally longer than UK breaks. Ambient temperatures there are also high enough to enable a range of outdoor activities to be undertaken with substantial body area exposed. The autumn holidays to these destinations extend summer sun exposure, similarly to those described above for a summer, 2 weeks in the autumn may be equivalent to up to 1.5–2 months outdoors in the UK in summer.
Winter
In the UK winter, November to March, 11.9% of responders (n = 90) reported no holidays or staying in the UK, where the combination of negligible UV and very low ambient temperatures rules out any contribution to annual erythema exposure. In contrast, 12.5% of responders (n = 94) spent 5–30 days overseas with extreme UV levels that provided a significant contribution to the sun exposure similar to the summer breaks. 3.6% of responders (n = 27) went for a week for snow sports. Danish skiers received an accumulated 44.5 SED during 6 days of skiing in the Alps in March.33 Although skiers expose only a small skin area, it is important to include skiers into this analysis because the face is a very common site for skin cancer.17Spring
In spring, April and May, 15.8% (n = 119) had no holidays and 33.4% of responders (n = 252) spent time off in the UK for 5–7 days. At this time of the year UVI levels in the UK are relatively low, with the exception of the transient low ozone events that have been previously observed in the UK and resulted in an UVI being comparable to summer clear days.35 26% of responders went to very high (for 5 to 7 days) and extreme (for 7, 10 and 14 days) UVI destinations. For the majority, this is likely to be the first UV exposure they received on unconditioned skin after a long winter.Validation of the survey
16 participants from the same cohort wore dosimeters from April to September 2017. The dosimetry data showed that none of the participants (n = 16) spent any time outdoors before work and this was in agreement with questionnaires, with the exception of one participant who answered up to 30 min outdoors in the survey.The majority of participants answered the Q3 question as never, occasionally and always. The recordings from dosimeters were rated accordingly: no exposure = never, one or more exposure episode during the study but less than once or more every week = occasionally, and one or more exposure days every week excluding holidays = always.
Table 4 lists the sample size, n, Spearman rank correlation coefficient, 95% confidence intervals (CI) and average time outdoors for questions Q3, Q4, Q6 and Q7. The questionnaire answers given by the participants very strongly and strongly correlated with the measured time for questions about the frequency of lunch break Q3 (rs = 0.85, 95% Cl: 0.61, 0.94, n = 15) and the time outdoors during the lunch break Q4 (rs = 0.74 95% Cl: 0.26, 0.93, n = 11), respectively. The mean time spent outdoors during the lunch break was 23.6 ± 11.3 min.
| Questions | n | r s strength of correlation | (95% CI) | Average time, min | Survey average time, min |
|---|---|---|---|---|---|
| a Participants who do not spend time outdoors were not included in the calculations of the average. | |||||
| Q3: How often do you spend lunch break outdoors? | 16 | 0.86, very strong | (0.61, 0.94) | n/a | n/a |
| Q4: How long do you spend outdoors at lunch break? | 11 | 0.74, strong | (0.26, 0.93) | 23.6 ± 11.3a (n = 11) | 21.5 ± 12.2 (n = 711) |
| Q6: Do you spend any time outdoors after commuting from work? | 16 | 0.80, strong | (0.50, 0.93) | 29.2 ± 7.8a (n = 9) | 30.4 ± 21.4 (n = 650) |
| Q7: On a typical two-day weekend, how much time in total, do you spend outdoors? | 16 | 0.77, strong | (0.44, 0.91) | 273.6 ± 69.8 (n = 16) | 300 ± 153 (n = 876) |
A very strong correlation between the time spent outdoors after commuting was found (question Q6), rs = 0.80 (95%Cl: 0.50, 0.93, n = 16), with the average time of 29.2 ± 7.8 min measured by dosimeters.
A strong correlation (rs = 0.77, 95%CI: 0.44, 0.91) was found for the time spent outdoors at weekends (question Q7), with the mean time of 273.6 ± 69.8 min. 4 participants overestimated their outdoor time: 3 participants stated 8 h in Q7 but spent around 5 h on average, one participant stated more than 10 h but went outdoors for only 3 h on average.
These results show that the lifestyle survey can be used to obtain information about the time spent outdoors and to design direct dosimetry studies in small representative groups.
Conclusions
In this study, the feasibility of using a lifestyle survey to obtain information on outdoor behaviour of indoor workers was examined. The study was conducted on office and laboratory workers of Public Health England, UK. Questions addressed the time of day spent outdoors and its duration for weekdays, weekends, and holidays.Outdoor activities before and after work are constrained by work pattern and commuting. 30% of responders reported going outdoors before commuting for an average of 22.5 ± 16.2 min and 75% spent 30.4 ± 21.4 min outdoors after work. The morning and evening contribution of the outdoor time to total daily UV exposure did not exceed 3.5% of the available daily erythema dose. A long commuting time may reduce this value further as outdoor activities happen before 8 am and/or after 6 pm.
Only 11% of responders always go outdoors during the lunch break for 21.5 ± 12.2 min. In total, weekday exposure may contribute less than 13% of the daily available erythema dose. At the weekend, responders spent 5.0 ± 2.6 h outdoors over the two days. If taken around midday, it accounts for approximately 50% of the daily available UV exposure. The high variability of the British weather results in a significantly lower accumulative dose than may be expected from the maximum seasonal UVI. In the UK winter months, November to March, the combination of very low environmental UV and low ambient temperatures results in negligible UV exposure on weekdays and at weekends.
The majority of UV exposure came from holidays. In summer, 40.7% of responders went to destinations where the UVI may be up to 2 times higher than in the UK; durations of overseas holidays are also longer than UK breaks. The erythema dose from two weeks of holidays in extreme UVI destinations could be comparable to 1.5–2 summer months in the UK.
Weekend and holiday exposure is likely to happen in the middle of the day when UV levels are the highest and often more time is spent outdoors. Sun protection is essential in late spring and summer; extra care is needed to avoid over-exposure at extreme, high and very high UV level destinations.
The questionnaire was validated by direct measurements of erythema effective irradiance for 16 participants from the same cohort in April–September 2017 resulting in very strong and strong correlation with survey results.
The current pilot study was limited to a similar socio–economic group, mostly from affluent areas in the south of England. It is essential to expand this survey for a much broader cross-section of society. When used in large population studies, such a questionnaire in combination with dosimetry on small representative groups could provide quantitative data on UV exposure essential for the assessment of health impacts of sun exposure.
Using the employers’ route may be a good way to approach participants. However, in this study, the use of the organisation's intranet has been proven inefficient and further consideration is needed to avoid poor response rates.
Balancing risks and benefits of sun exposure is very important. The morning light (low UV exposure) can boost circadian rhythm entrainment, especially in winter, whereas lunch breaks outdoors could benefit cardiovascular, bone and mental health. These benefits have to be balanced against adverse effects, such as erythema and ocular pathologies, increased risk of skin cancers, premature skin aging, and weakening of the immune system. The public health message has to provide a balanced approach to sun exposure.
Conflicts of interest
There are no conflicts to declare.References
- R. M. T. Lucas, W. Smith and B. Armstrong, Solar ultraviolet radiation: global burden of disease from solar ultraviolet radiation. Environmental Burden of Disease Series. 13. N, World Health Organization, Geneva, 2006 Search PubMed.
- H. Van der Rhee, E. de Vries, C. Coomans, P. van de Velde and J. W. Coebergh, Sunlight: For better or for worse? A review of positive and negative effects of sun exposure Cancer Res. Front., 2016, 2, 156–183 Search PubMed.
- B. Diffey, Sun Protection. A risk managment approach, IOP Publishing, London, 2017 Search PubMed.
- N. Downs, A. Parisi and P. Schouten, Solar ultraviolet radiation incident upon reef snorkelers determined by consideration of the partial immersion of dosimeters in the natural ocean environment, Meas. Sci. Technol., 2010, 22(1), 015801 CrossRef.
- F. Xiang, S. Harrison, M. Nowak, M. Kimlin, I. Van der Mei and R. E. Neale, et al., Weekend personal ultraviolet radiation exposure in four cities in Australia: influence of temperature, humidity and ambient ultraviolet radiation, J. Photochem. Photobiol., B, 2015, 143, 74–81 CrossRef CAS PubMed.
- N. J. Downs, P. W. Schouten, A. V. Parisi and J. Turner, Measurements of the upper body ultraviolet exposure to golfers: non-melanoma skin cancer risk, and the potential benefits of exposure to sunlight, Photodermatol., Photoimmunol. Photomed., 2009, 25(6), 317–324 CrossRef PubMed.
- M. G. Kimlin, N. Martinez, A. C. Green and D. C. Whiteman, Anatomical distribution of solar ultraviolet exposures among cyclists, J. Photochem. Photobiol., B, 2006, 85(1), 23–27 CrossRef CAS PubMed.
- M. G. Kimlin, A. V. Parisi and J. Wong, Quantification of personal solar UV exposure of outdoor workers, indoor workers and adolescents at two locations in Southeast Queensland, Photodermatol., Photoimmunol. Photomed., 1998, 14(1), 7–11 CrossRef CAS.
- E. Herlihy, P. H. Gies, C. R. Roy and M. Jones, Personal dosimetry of solar UV radiation for different outdoor activities, Photochem. Photobiol., 1994, 60(3), 288–294 CrossRef CAS PubMed.
- M. A. Serrano, J. Canada, J. C. Moreno and G. Gurrea, Personal UV exposure for different outdoor sports, Photochem. Photobiol. Sci., 2014, 13(4), 671–679 RSC.
- K. L. Glanz, P. Gies, D. L. O'Riordan, T. Elliott, E. J. Nehl and F. A. McCarty, et al., Validity of self-reported solar UVR exposure compared to objectively measured UVR exposure, Cancer Epidemiol., Biomarkers Prev., 2010, 19(12), 3005–3012 CrossRef PubMed.
- M. A. Serrano, J. Cañada and J. C. Moreno, Erythemal ultraviolet exposure of cyclists in Valencia, Spain, Photochem. Photobiol., 2010, 86(3), 716–721 CrossRef CAS PubMed.
- M. A. Serrano, J. Cañada and J. C. Moreno, Ultraviolet exposure for different outdoor sports in Valencia, Spain, Photodermatol., Photoimmunol. Photomed., 2011, 27(6), 311–317 CrossRef PubMed.
- B. Diffey, C. Gibson, R. Haylock and A. McKinlay, Outdoor ultraviolet exposure of children and adolescents, Br. J. Dermatol., 1996, 134(6), 1030–1034 CrossRef CAS PubMed.
- R. Stafford, M. Farrar, R. Kift, M. Durkin, J. Berry and A. Webb, et al., The impact of photosensitivity disorders on aspects of lifestyle, Br. J. Dermatol., 2010, 163(4), 817–822 CrossRef CAS PubMed.
- E. Thieden, Sun exposure behaviour among subgroups of the Danish population. Based on personal electronic UVR dosimetry and corresponding exposure diaries, Dan. Med. Bull., 2008, 55(1), 47–68 Search PubMed.
- Active lives adult survey [Available from: https://www.sportengland.org/media/12458/active-lives-adult-may-16-17-report.pdf.
- Measuring national well-being: Life in the UK: 2016 [Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/wellbeing/articles/measuringnationalwellbeing/2016#how-do-we-spend-our-time-and-are-we-satisfied-with-its-use.
- Natural England, Department for Environment, Food & Rural Affairs, and Forestry Commission, Survey shows that more people are heading for the outdoors in England [Available from: https://www.gov.uk/government/news/survey-shows-more-people-are-heading-for-the-outdoors-in-england.
- Physical Activity Statistics 2015 British Heart Foundation Centre on Population Approaches for Non Communicable Disease Prevention. Nuffield Department of Population Health, University of Oxford [Available from: https://www.bhf.org.uk/-/media/files/.../bhf_physical-activity-statistics-2015feb.pdf.
- Travel Trends: A report on the 2016 International Passenger Survey (2016) Office for National Statistics, London [Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/leisureandtourism/articles/traveltrends/2016.
- J. Schmitt, E. Haufe, F. Trautmann, H.-J. Schulze, P. Elsner and H. Drexler, et al., Occupational UV-Exposure is a Major Risk Factor for Basal Cell Carcinoma: Results of the Population-Based Case-Control Study FB-181, J. Occup. Environ. Med., 2018, 60(1), 36–43 CrossRef PubMed.
- S. Schneider, K. Diehl, L. Schilling, M. Spengler, R. Greinert and T. Görig, Occupational UV Exposure And Sun-Protective Behaviour In German Outdoor Workers: Results of a Nationwide Study, J. Occup. Environ. Med., 2018 DOI:10.1097/JOM.0000000000001397.
- M. Wittlich, S. Westerhausen, P. Kleinespel, G. Rifer and W. Stöppelmann, An approximation of occupational lifetime UVR exposure: algorithm for retrospective assessment and current measurements, J. Eur. Acad. Dermatol. Venereol., 2016, 30, 27–33 CrossRef PubMed.
- T. D. V. Swinscow and M. J. Campbell, Statistics at square one, Medical Journal British, London, 11th edn, 2009 Search PubMed.
- New Zealand's Environmental Reporting Series: Environmental indicators Te taiao Aotearoa. UV Index for New Zealand [Available from: http://archive.stats.govt.nz/browse_for_stats/environment/environmental-reporting-series/environmental-indicators/Home/Atmosphere-and-climate/uv-intensity.aspx.
- United States Environmental Protection Agency. UV Index for USA [Available from: https://www.epa.gov/sunsafety/sun-safety-monthly-average-uv-index#tab-3.
- National Network for the measurements of ultraviolet radiation in Greece [Available from: http://www.uvnet.gr.
- Liley JBaRLM, Where on Earth has the highest UV?, in UV Radiation and its Effects: An Update, ed. R. L. McKenzie and E. Davis for NIWA and RSNZ, Royal Society of New Zealand, Wellington, New Zealand, pp. 36–37. [Available from: https://www.niwa.co.nz/sites/default/files/import/attachments/Liley_2.pdf Search PubMed.
- Public Health England Solar Monitoring Network [updated 26 January 2018. Available from: https://uk-air.defra.gov.uk/research/ozone-uv/uv-uk-monitoring.
- G. Schauberger, Model for the global irradiance of the solar biologically-effective ultraviolet-radiation on inclined surfaces, Photochem. Photobiol., 1990, 52(5), 1029–1032 CrossRef CAS PubMed.
- B. Diffey, A behavioral model for estimating population exposure to solar ultraviolet radiation, Photochem. Photobiol., 2008, 84(2), 371–375 CrossRef CAS PubMed.
- B. Petersen, M. Triguero-Mas, B. Maier, E. Thieden, P. A. Philipsen and J. Heydenreich, et al., Sun behaviour and personal UVR exposure among Europeans on short term holidays, J. Photochem. Photobiol., B, 2015, 151, 264–269 CrossRef CAS PubMed.
- K. A. Baczynska, L. L. Price, M. P. Higlett and J. B. O'Hagan, Estimating Sun Exposure of Children in Day Care Nurseries in South Oxfordshire, UK, Photochem. Photobiol., 2016, 92(1), 193–200 CrossRef CAS PubMed.
- B. H. Petkov, V. Vitale, C. Tomasi, A. M. Siani, G. Seckmeyer and A. R. Webb, et al., Response of the ozone column over Europe to the 2011 Arctic ozone depletion event according to ground-based observations and assessment of the consequent variations in surface UV irradiance, Atmos. Environ., 2014, 85, 169–178 CrossRef CAS.
| This journal is © The Royal Society of Chemistry and Owner Societies 2019 |