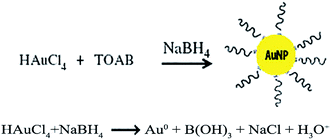Engineered gold nanoparticles for photothermal cancer therapy and bacteria killing
Alireza Gharatape
ae,
Soodabeh Davaran
b,
Roya Salehi
*c and
Hamed Hamishehkar
*d
aDepartment of Medical Nanotechnology, School of Advanced Medical Science, Tabriz University of Medical Science, Tabriz, Iran
bDrug Applied Research Center and Department of Medicinal Chemistry, Faculty of Pharmacy, Tabriz University of Medical Science, Tabriz, Iran
cResearch Center for Pharmaceutical Nanotechnology and Department of Medical Nanotechnology, School of Advanced Medical Science, Tabriz University of Medical Science, Tabriz, Iran. E-mail: salehiro@tbzmed.ac.ir; Fax: +98 4133363132; Tel: +98 4133363161
dDrug Applied Research Center, Tabriz University of Medical Science, Tabriz, Iran. E-mail: hamishehkarh@tbzmed.ac.ir
eStudent Research Committee, Tabriz University of Medical Science, Tabriz, Iran
First published on 1st November 2016
Abstract
Over recent decades, one of the most important and complex problems facing our society is the multi-drug resistance of human cancer cells and pathogens to most clinically approved therapeutics. Recent advances in nanoscience and nanotechnology have expanded our ability to design and construct nanomaterials with targeting, therapeutic, and diagnostic functions. These multifunctional materials have gained attention as promising tools for selective cancer/bacteria therapy in the absence of current drugs. Photothermal therapy (PTT) is a minimally invasive therapy in which photon energy is converted into heat in order to kill cancer cells. Gold nanoparticles (GNPs) with a high light-to-heat conversion capability are among the most important candidates for PTT. GNP-assisted PTT has shown great success in recent years, suggesting promise for future applications. In this review, we will discuss the current status of GNPs in the photothermal treatment of cancer and bacterial conditions. The review starts with an outline of recent developments in the various methods used for the size- and shape-controlled synthesis of GNPs, followed by a discussion of the modification of GNPs using suitable protecting and functionalizing agents. We will then consider therapeutic outcomes of different types of GNP-assisted PTT in cancer therapy and bactericide through a comprehensive review of the most important results obtained both in vivo and in vitro. The advantages and disadvantages of methods for developing different-shaped GNPs, variations in irradiation conditions, the use of PTT in combination with other therapeutic methods, and a comparison between the PTT efficacies of different-shaped GNPs will also be discussed in detail.
1. Introduction
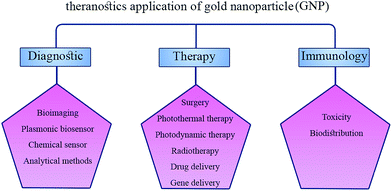
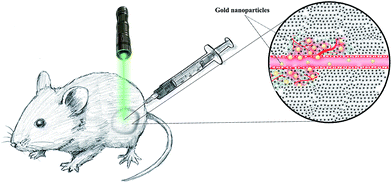
The struggle between man and disease, and man's considerable efforts to overcome disease has led to the emergence of novel methods, treatments, and modern medical systems. Just a few decades ago, before the advent of the concept of nanotechnology, few predicted that one day most development, research, and costs in the field of healthcare would be allocated to nanotechnology.1 Nanotechnology, and more accurately nanomedicine, could progress rapidly and replace traditional therapeutic methods with new and more effective systems to win in the fight against disease. At the same time, the biggest challenge for the treatment of diseases such as cancer and infections is the resistance of cancer cells and bacteria and viruses to current drugs and antibiotics.2–6 Thus, further studies and greater investment are required to introduce new antibiotics and anticancer drugs for more effective therapy. Nanomedicine could address many issues in cancer therapy by maximizing drug targeting and minimizing drug side effects.7–13 In addition to these advantages, the real miracle of nanotechnology is to change the overall war strategy. The resistance of bacteria and cancer cells after a period of treatment with existing drugs forced us to improve the generation and potency of medicines. Perhaps, on the opposite side, microbes and cancer cells are also fighting with humans for their survival. Thus, the field of nanotechnology could change the balance in our favor by providing new and advanced treatments.Photothermal therapy, defined as photothermal ablation or optical hyperthermia, has been vigorously researched as a minimally invasive approach to cancer therapy.14 The key component of this technique is a photothermal transducer that can absorb near infrared (NIR) light effectively and convert it into heat through a non-radiative method.15,16 Gold nanoparticles (GNPs) can be designed to have strong surface plasmon resonance in the NIR region, providing the best optical window for biomedical imaging and therapy owing to the low optical attenuation coefficients of water and other tissue chromophores in this spectral range (700–900 nm).17 Therefore, GNPs can be used for photothermal therapy (PTT) and photodynamic therapy (PDT) for therapeutic applications and surface-enhanced Raman spectroscopy (SERS), multiphoton microscopy, X-ray computed tomography (CT), magnetic resonance imaging (MRI), positron emission tomography (PET), and single-photon emission computed tomography (SPECT) for imaging purposes18–22 (Fig. 1). PTT uses GNPs as a transducer to convert NIR light to heat and make a localized temperature increase within tissues that have GNP accumulation. Nanoparticles have high uptake in tumors due to the enhanced permeability and retention effect.23,24 This means that substantial temperature increases can be obtained in tumoral tissues with NIR-light exposure, while the surrounding tissues, which have negligible nanoparticle accumulation, undergo little to no change in temperature with NIR exposure. Thus, the GNP-enhanced PTT method can specifically target tumors more effectively than traditional chemotherapy.
PTT has been investigated with certain types of gold nanostructure in early clinical trials. As an example, pilot clinical studies with AuroShell (150 nm PEGylated polyethylene glycol 5000) gold nanoshells have been approved by the Food and Drug Administration, wherein the nanoshells are given intravenously to patients with primary and/or metastatic lung tumors or for the treatment of head and neck cancer.25,26
2. GNPs
2.1. Methods of synthesis
Several methods for the synthesis of GNPs have been reported, each of which have unique characteristics.27Usually, in the synthesis of GNPs using a chemical reduction method, reduction of a gold salt solution is achieved using appropriate reducing agents such as citrate or borohydrides to generate Au(0). This is followed by stabilization of the achieved GNPs by use of appropriate stabilizing/capping agents such as citrate or alkane thiols, which avoids agglomeration of NPs by forming a metallic precipitate.
The synthesis of GNPs was achieved by use of chemical or natural reducing agents.28–33 Size, shape, and morphology are the more dominant characteristics that should be considered when designing a suitable method for the synthesis of GNPs; e.g. rod-shaped NPs are synthesized through a series of special procedures and reducing agents.34–36 This process might be modified when spherical core/shell NPs are required. A desired size (sub 100 nm) is one of the main indices of GNPs to be considered for access to various areas of treatment such as PTT, PDT, sensing, imaging, hyperthermia, and drug delivery.37–41 Several methods of GNP synthesis, chemical synthesis, and green synthesis are discussed below.
2.1.1.1. Synthesis of GNPs using sodium citrate reducing agent (Na3C6H5O7·2H2O). The synthesis of GNPs by citrate, also known as the Turkevich method, is carried out via a reducing reaction between HAuCl4 and trisodium citrate (Na3C6H5O7·2H2O). During this reaction, Au3+ is reduced to Au0 (Fig. 2). The amount of reducing agent and the concentration of the gold salt, as well as the temperature and stirring intensity of the reaction solution, determines the size, morphology, and concentration of the produced GNPs. In addition, the size of the GNPs is affected according to whether the reducing agent is added suddenly or in a dropwise manner due to the impact on the speed of the reduction process.43–52 In a study conducted by Sahoo et al., the size of the GNPs was controlled by changing the concentration of the citrate salts. An increase in the concentration of the citrate salt from 0.09 to 1.5 wt% resulted in a decrease in the size of the GNPs from 230 to 25 nm, respectively.53
| 2HAuCl4 + 3C6H8O7 → 2Au0 + 3C5H6O5 + 8HCl + 3CO2 |
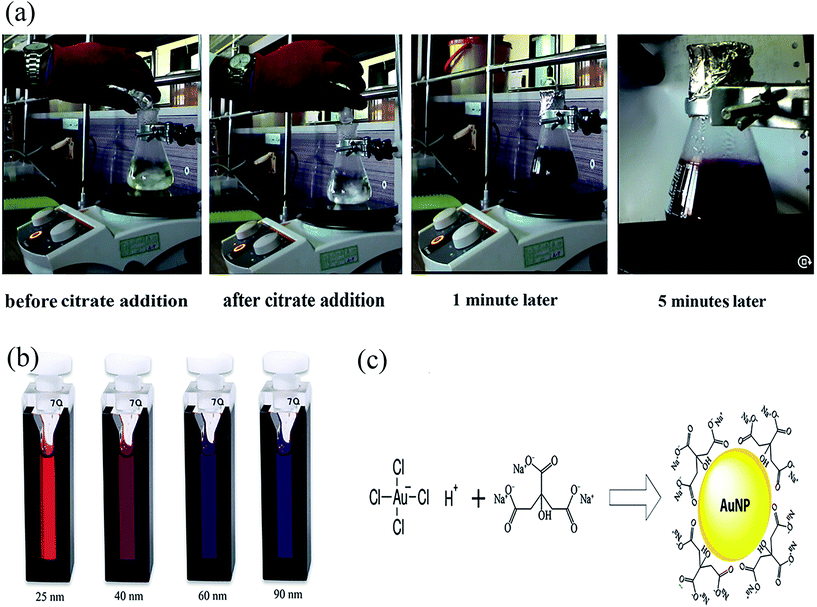 | ||
| Fig. 2 (a) Synthesis of gold nanoparticles using sodium citrate; (b) preparation of different-sized gold nanoparticles by the citrate method; (c) preparation of citrate-stabilized gold nanoparticles. | ||
2.1.1.2. Synthesis of GNPs using sodium borohydride and potassium hydroxide reducing agent (NaBH4, KOH). In general, this method produces much smaller GNPs than the previously described method.54 In an interesting study, Prado and coworkers compared two reducing agents, sodium citrate and sodium borohydride, in the synthesis of GNPs. NaBH4 produced more nuclei initiators and small GNPs, while the GNPs synthesized using sodium citrate as the reducing agent produced more stable nanoparticles.54 The mechanism of GNP synthesis in this method is different to the method described in Section 2.1.1.1. Hexadecyltrimethylammonium bromide solution is mixed with the gold salt solution. Then toluene, ethanol, and castor oil are added and stirred for a few min to produce a two-phase mixture. Next, NaBH4 solution is added dropwise to the two-phase mixture in order to reduce the salt to GNPs. Simultaneously, GNPs are derivatized with hexadecyltrimethylammonium bromide and transferred into the oil phase of the reaction mixture.55,56 Sodium borohydride has also been used by different groups to prepare very small spherical GNPs (3 nm).57,58 In addition to spherical GNPs, Samal and coworkers investigated the role of NaBH4 in methods for the synthesis of gold nanorods (GNRs).59 Jana and colleagues synthesized high aspect ratio (the proportional relationship between width and height) GNRs via a seeding growth method using NaBH4 solution. In this method, HAuCl4 was reduced with borohydride, and 3.5 nm seed particles were prepared. The nanoparticle growth is induced by means of the resultant seeds. Transmission electron microscope (TEM) images showed three different aspect ratios (4.6, 13, and 18) which could be obtained by varying the ratio of seed to gold salt.60 As a result, NaBH4 is a versatile reducing agent which can be used as reducing agent in the synthesis of different-shaped GNPs including spherical,57,58 rod,59,60 cubic61 and star62 shapes (Fig. 3).
In another method, KOH solution is added to the mixture of castor oil and ethanol. The GNPs are prepared by continuous stirring of the mixture at 80 °C.63
2.1.1.3. Synthesis of GNPs using ultraviolet (UV) and X-ray radiation methods. To prepare GNPs via a UV irradiation method, predetermined amounts of chloroauric acid and Triton X-100 solutions were exposed to photo-irradiation for a specific time and distance from the UV source. The photo-activation produced very small GNPs (pink-colored solution) as cores. The addition of extra chloroauric acid and ascorbic acid under irradiation caused the growth of GNPs in a controlled way from 5 to 80 nm.64,65
In the preparation of GNPs via the X-ray method, Triton X-100 was added to a solution of gold salt and then irradiated with X-rays. X-rays reduce the gold salt to GNPs. The intensity and exposure time of the X-ray radiation are the key parameters in determining the size of the GNPs.64,66
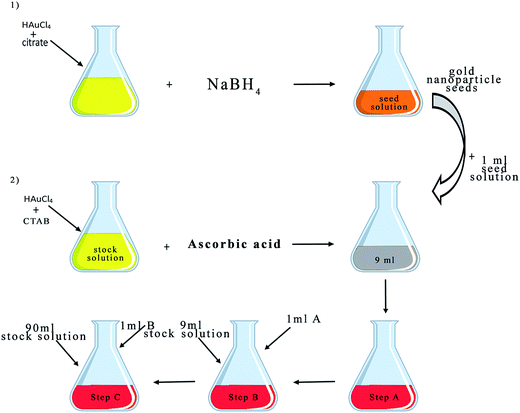
2.1.1.4. Synthesis of GNPs using a seed-mediated growth method. In the seed-mediated growth method, the gold salt solution is mixed with a solution containing NaBH4 (reducing agent) and cetyltrimethylammonium bromide (CTAB) (a quaternary ammonium surfactant) with vigorous stirring.46,67 In the seed-mediated growth method, the first step is the synthesis of seeds which is usually induced by direct reduction. Afterward, the nanoparticles are grown around the seeds. GNRs are the anisotropic particles which are synthesized by this method. The suitable surface area and surface chemistry of GNRs means that these particles are appropriate candidates for biological applications.68 Burrows and coworkers specifically focused on the surface chemistry of gold,68 while Gole and colleagues investigated the role of the size and nature of the seed on the synthesis of GNRs. They found that the aspect ratio of the GNR increased when the size of the seed decreased.69 Brown and coworkers synthesized colloidal GNPs by seeding NH2OH/Au3+ solutions. They demonstrated that the suggested method provided a more monodispersed nanoparticle than the citrate method of synthesis. Furthermore, smaller particles may be grown by this method. The size of the particles was between 30 and 100 nm, as measured by atomic force microscopy analysis.70 In another method, a CTAB solution was added to an HAuCl4 solution, and then a solution of silver acetate (AgC2H3O2) was added to the mixture. Next, a small amount of ascorbic acid (a mild reducing agent) was added under continuous stirring before the solution was allowed to reach a steady state, leading to NP formation. In this method, by changing the amount of silver acetate, the aspect ratio (the proportional relationship between the width and the height)71,72 of the synthesized gold nanorods (GNRs) will be changed73–75 (Fig. 4). In addition to the rod-shape of the GNPs, the seed-mediated growth method is used for the synthesis of gold nanostars,62,76 branched gold nanocrystals77 and gold (nanocages,78 nanocubes79 and core/shell NPs80–82).
2.1.1.5. Synthesis of different-shaped GNPs with the aid of biopolymers. In two separate projects, GNSps were synthesized at the size of 25 nm and 14 nm by luminol; one of the most commonly used chemi-luminescent reagents, to be used as electro-chemi-luminescence sensors for the determination of H2O2.83,84 In another study, gold nanoflowers (GNFs) were synthesized from a mixture of luminol and chitosan (a well-known biopolymer) as reducing agents for the reduction of HAuCl4. By reducing HAuCl4 with luminal83 or chitosan85,86 only, red-colored GNPs were obtained. However, when HAuCl4 was reduced by a mixture of luminol and chitosan, blue colloidal GNFs (90 nm) were obtained and a significant red shift of λmax, from 522 to 663 nm, was detected. By changing the amount of luminol or chitosan, the morphology and size of the GNFs could be tailored.87 The effect of DNA sequences on the morphology of GNPs throughout crystal expansion has previously been investigated by Wang and colleagues. Three types of 30-mer DNAs, including of poly A, poly C, and poly T (designated as A30, C30, and T30), were decorated on GNSps (20 nm) as the seeds for nanoparticle growth. Then, by further addition of HAuCl4 and using NH4OH as the reducing agent, GNFs were synthesized on A30- or C30-coated GNSps, while T30 resulted in GNSp.88 Li and coworkers worked on an enzymatic method and directly synthesized GNFs from HAuCl4 using enzymes.89 These researchers synthesized monodispersed GNFs (70–90 nm) via a solution process at room temperature simply by using HAuCl4, trypsin, and ascorbic acid, which is stable for 1 year in contrast to previously reported GNFs with a large size and poor stability90,91 (Fig. 5).
2.1.2.1. Green synthesis of GNPs from plants. Green synthesis of GNPs is more economical than chemical methods of synthesis due to the ready availability of raw materials (phytochemicals and herbs) such as black tea, Aloe Barbadensis, Rosa Berberifolia, soy, and chamomile. A freshly prepared herbal extract is filtered several times, added to the HAuCl4 solution, and heated to form GNPs. The shape and size of the GNPs is controlled by the plant extracts used or the reaction time.92,97,98 Mukherjee and coworkers synthesized highly stable and biocompatible GNPs by using Peltophorum pterocarpum leaves extract.99 Morinda citrifolia root extract was used by Suman and colleagues as a reducing agent in order to synthesize GNPs in the range of 8–17 nm.100 Fierascu and coworkers developed the synthesis of GNPs using Salvia officinalis101 extract, while Basavegowda and colleagues used Punica granatum extract as a reducing agent in a green synthesis method.102
2.1.2.2. Green synthesis based on the use of bacteria and viruses. Various bacteria such as Streptomyces clavuligerus,103 Klebsiella pneumonia,104 Streptomyces sp.,105 E. coli,106 and thermophilic Geo Bacillus sp.107,108 are used for this purpose by reducing Au3+ to Au0. The NPs synthesized by this method have a size of about 20–30 nm. Furthermore, other studies have reported use of Bacillus subtilis bacteria for the reduction of Au3+ to Au0.109 Graf and colleges developed a procedure based on mixing of HAuCl4 and K2CO3 and using bacteria as reducing agent.110 Liu and coworker showed Bacillus megatherium could bind to Au3+ to reduce Au3+ to Au0.111 In another study, Radloff et al. synthesized gold nanoshells via Chilo iridescent virus. These researchers assembled a gold shell around the viral core and achieved 2–5 nm viral/GNPs.112
2.2. Application of GNPs in future medicine
Gold has recently been introduced in many therapeutic and diagnostic procedures, mainly due to its unique molecular and optical characteristics. A few examples of the applications of GNPs are sensing and diagnosis at nanobiosensors, binding to DNA, and molecular studies based on hybridization imaging, drug delivery, PTT and PDT113–123 (Fig. 6). Due to the immense progress of photonic science and new findings on the unique features of gold in the optic and plasmonic field, it is expected that photonics will have a special contribution in future medicine, and GNPs will play a unique role in the field of diagnosis and therapy.115,124–1283. Photothermal therapy
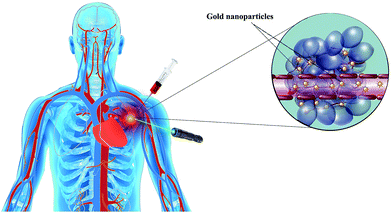
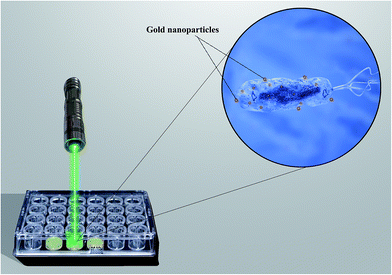
PTT can be considered as a non-invasive method of treatment by conversion of photons into heat energy to destroy cancer cells as well as pathogenic agents14,129–137 (Fig. 7). PTT is based on NIR-light irradiation to the NPs with special composition such as gold, quantum dots, carbon nanotubes, and graphene oxide.138–147 This irradiation leads to nanoparticle excitation and the dissipation of the heat in the surrounding area.138–147 NIR photon radiation is applied in the range between 700 and 1400 nm in a continuous or pulsed mode. Use of pulsed NIR-light irradiation causes nanoscale vapor bubbles to expand and collapse around the NP in the first nanosecond after excitation and the temperature of the surrounding water shell to increase. This causes the temperature of the cells eventually to increase to at least 45–55 °C, causing an increase in blood flow leading to impaired cellular homeostasis and irreversible cell damage (Fig. 7).148–151 The emitted photon wavelength is affected by the NP size and concentration.150,152–154 Not all the energy obtained from the photon radiation is converted into heat; however, by regulating the intensity of the radiation and exposure time it is possible to optimize the process.131,149,155,156 Surface functionalization of NPs by a particular ligand or a special polymer allows targeted cells to be identified without the removal of NPs by the immune system, as well as an increase in the circulation time of NPs.157–163 Medical science is currently facing the serious challenge of drug resistance of cancer cells and microbial pathogens (MDR and XDR), which may be overcome by the application of NPs such as GNPs.164–167 The PTT effect of GNPs on pathogenic agents and cancer in vitro and in vivo models has been reported.168–174 The importance of PTT in the treatment of drug-resistant health challenges is due to the fact that this technique is a drug-free method allowing enormous savings in terms of costs and research time to find and synthesize new antibiotics and chemotherapeutic agents.175–184 | ||
| Fig. 7 Schematic illustration of gold nanoparticle photothermal therapy in cancer cell models.209 | ||
3.1. Photothermal therapy in cancer treatment (as a complementary or separate treatment)
In PTT cancer treatment, there are two important moot points. First, cancer cells can be targeted and in the next step cell uptake or cell internalization may take place. Second, the use of parameters such as wavelength, intensity of radiation, discontinuous or continuous flow, and direct or indirect radiation are also important depending on the size, shape, concentration, and nanoparticle's surface.185–201 In general, PTT depends on the photosensitizer (PS) taken up by the cancer cells to transfer light to heat, leading to photoablation of the cells and subsequent cell death. Consequently, photosensitizing agents are a key factor in PTT. Among the numerous PSs, GNPs are a special PS which exhibit strong localized surface plasmon resonance. Many types of GNPs, such as nanorods, nanocages, and nanocore/shells, have been reported as PSs in PTT.202–2083.1.1.1. Cancer PTT with undecorated GNRs. Pattani and coworkers (2014) investigated the effect of PTT on human colorectal tumor cells (HCT-116) by using GNRs with an average size of 47 × 15 nm to optimize the ‘clean’ destruction of cells by inducing maximum apoptosis. The cell penetration and localization of GNRs to organelles in the perinuclear space was monitored for 1.5, 6, and 24 h. A continuous laser was applied in the intensity range of 20–50 W cm−2 for 5 min at a wavelength of 808 nm. The highest apoptotic percentage was found after 24 h of cell exposure with GNRs, and in the beam intensity of 37.5 W cm−2. The researchers found that cell-death rate was related to GNR penetration and localization209 (Fig. 8).
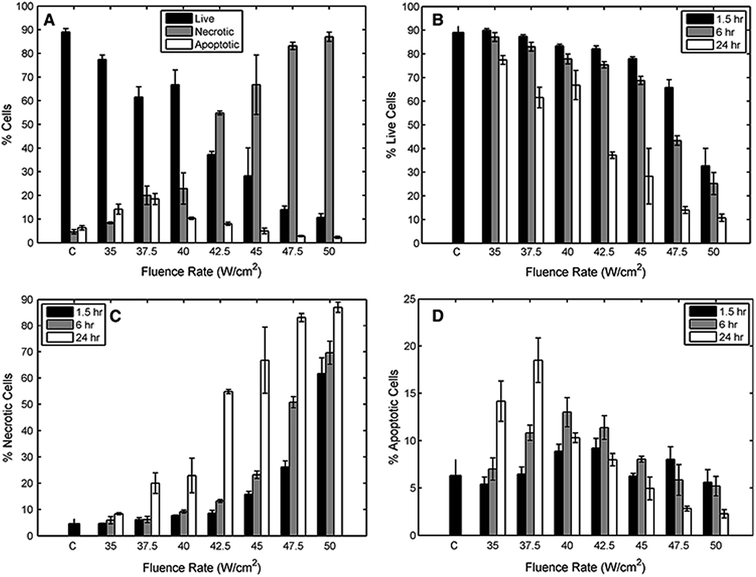 | ||
| Fig. 8 Quantitative analysis of human colorectal tumor cells (HCT-116) death in response to nPTT. In (a) we see the 24 h-incubated GNRs live, necrotic and apoptotic percentages for several fluence rates and see the trends. In (b–d) we see the live, necrotic, and apoptotic cell percentages, respectively, with all three GNR incubation times compared together at several fluence rates. Reprinted with permission from ref. 209. Copyright 2015 Springer. | ||
Okuno and colleagues investigated the effect of PTT of GNR internalized to the lymph nodes. GNRs with a particle size of 67 × 10 nm were irradiated using a continuous laser. The intensity of the radiated photons was 1.5 W cm−2, with a wavelength of 598 nm, and was applied for 3 min until the temperature of the tumor area of the mice reached 51 °C. The systemic administration of GNRs resulted in almost the same degree of temperature elevation of the tumor tissue as when GNRs are locally injected. This observation indicated the successful localization of GNRs in the tumor tissue. However, despite the increased temperature and consequently irreversible tissue destruction, the tumor was not wholly destroyed since viable tumor cells were able to regrow.210
3.1.1.2. Cancer PTT with polymer-coated GNRs. Mackey and coworkers (2014), synthesized PEGylated GNRs with different sizes (38 × 11, 28 × 8, and 17 × 5 nm) and studied their photothermal contrast ability for PPTT application on human oral squamous cell carcinoma (HSC-3 cells) by irradiation of continuous laser with a wavelength of 808 nm, laser radiation severity of 5.8 W cm−2 and exposure time of 2 min. The results indicated that GNRs with a particle size of 28 × 8 nm are able to generate the most effective contrast agent. Furthermore, 28 × 8 nm GNRs showed the best compromise between the total amount of light absorbed and the fraction of which was converted to heat; leading to effective heating in the solution.211 Although this study provided valuable information regarding the effect of size in achieving the optimized result, its limitation was a lack of non-PEG-GNRs as a control to compare the effect of PEGylation on the performance of GNRs.
In 2008, Dickerson and colleagues investigated the possibility of PPTT by an in vivo study in the deep tissues of mammalians. GNRs were derivatized with PEG-5000 to be hidden from the immune system. This functionalization also reduced the surface charge of GNRs to minimize the possible ionic interaction with different organs of the body and consequently to increase the biocompatibility of the delivery system. The final size of the nanorods was in the range of 12–50 nm. PEGylated GNRs were injected directly into the tumor or intravenously into cancer-induced female mice. After a 13 day period, an average tumor growth inhibition for both delivery methods was observed, with resorption of >57% of the directly-injected tumors and 25% of the intravenously-treated tumors. In the previous work of this group, the surfaces of the GNRs were decorated with epithelial growth factor receptor antibodies (anti-EGFR; EGFR receptors are overexpressed on the cancer cell surface) for enhanced targeted delivery to the cancer cells during the in vitro cell culture study. The anti-EGFR-decorated GNRs significantly controlled the tumor growth to a greater extent than the pristine GNRs.212
In 2013, Yang and colleagues synthesized a magnetic polymer coated GNRs to achieve both aims, imaging and therapy, simultaneously. Surface decoration of magnetic NPs by polymer (poly-n-isopropylacrylamide) enhanced the localization of the particles in the cancer cells because of the ability of these types of polymers to respond to temperature. After accurate detection of the cancer cells by NPs, PTT was applied using a laser with a power of 2 W cm−2 and wavelength of 808 nm for 3 min to increase the temperature of the tumor area up to 90 °C. Treatment progress were done after about 10 days, and very good results were obtained in this way that when magnetic polymer is attached to GNPs the tumor volume fell to 0.25% compared to control group while the GNPs group attached to the non-magnetic polymeric NPs lead to decrease in tumor volume to 0.75% in comparison with control group.213
The full-thickness necrosis of the skin observed in 33.3% of animals systematically treated with the laser + GNRs demonstrated that GNRs may have leaked into the tissue near the skin. This may be considered as a main disadvantage of GNRs in generating serious side effects, and may be attributed to the small size of GNRs or high beam energy. The PTT efficacy of PEGylated GNRs were investigated in a difficult and fast growing murine melanoma (cancer-induced female C57BL/6 mice) model using an NIR light-emitting diode (LED) light source. Better biodistribution, greater half-life, and enhanced physical stability have been reported for PEGylated GNRs within in vivo models.214–216 In vivo results demonstrated that the cancer-induced mice in the control groups (treated with saline and GNRs without irradiation) were expired after 9 days. In the group receiving the NIR irradiation alone, mice survived only until 13 days, but the administration of GNRs in combination with NIR resulted in 29 days of cancer-induced mouse survival. Radiated laser intensity was almost 3.5 W cm−2 and an exposure time of 2 min led to a tumor area temperature of about 50 °C. Since the previous study reported the greater safety of LED light compared with laser irradiation,202 the results of this study present a practical way to apply PTT to GNR.169
3.1.1.3. Cancer PTT with antibody-conjugated GNRs. The positively charged GNRs (due to the presence of a bilayer of CTAB during the GNR synthesis) were changed to negative by conjugation of GNRs with poly(styrene sulfonate) to allow interaction with the positively charged anti-EGFR antibodies. The synthesized anti-EGFR-conjugated GNRs were targeted in vitro to one nonmalignant epithelial cell line, HaCat (human keratinocytes) and two malignant epithelial cell lines, HOC 313 clone 8 and HSC 3 (human oral squamous cell carcinoma), for both imaging and therapy purposes. The cell lines were irradiated under continuous NIR with different laser powers (160, 120, 80, and 40 mW). The photo-destruction results detected by the trypan blue cell viability test revealed that all HaCat normal cells were injured at 160 mW, while malignant HSC and HOC cells were destroyed at a lower laser power (80 mW). The increased uptake of anti-EGFR-conjugated PSS–GNRs by the two malignant cells (due to the presence of EGFR on the malignant cell surface) reduced the energy needed to cause destruction of these cells to about half of that required to cause death of the nonmalignant cells. These results showed that the side effects of PTT were minimized by the administration of anti-EGFR-conjugated GNRs.202
Gromley and colleagues tried to develop an effective polymeric drug delivery system for cancer tissue targeting with the aid of GNRs (60 × 15 nm). The results indicated that an enhanced accumulation of polymeric NPs into the tumor tissue (GNRs were already delivered to the tumor tissue) occurred by laser radiation due to the positive effect of heat on the endothelial permeability of the polymeric NPs.217–219 The experiment was repeated by conjugation of heat shock targeting the ligand to polymeric NPs, and it was found that the tumor accumulation of NPs was increased around twice the level of non-conjugated NPs. This study is an interesting example of the supportive and cooperative role of GNRs in successful drug targeting via polymeric NPs.220
Choi and colleagues developed novel NPs including GNRs decorated with chitosan-conjugated Pluronic F68 (CS-NC-PF68-GNRs), and used them as imaging agents for tumor detection and, concurrently, as a highly effective hyperthermia agent for cancer treatment with the PTT technique. In vitro results indicated that the cellular uptake of GNRs became easier by its conjugation with the polymer. An in vivo experiment demonstrated that after 12 days of treatment, complete tumor disappearance was observed in the tumor-induced mice treated with CS-NC-PF68-GNRs under NIR irradiation (Fig. 9).221
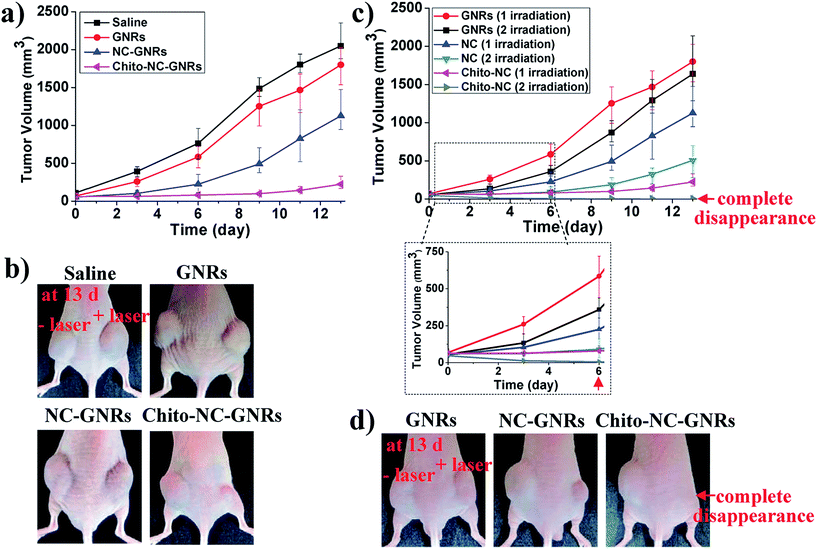 | ||
| Fig. 9 (a and c) Changes in tumor volumes; (b) tumor images 24 h after the intravenous injection of the nanoparticles and one-time NIR-laser irradiation (808 nm; 4 W cm−2 for 4 min); (d) tumor images after NIR-laser irradiation at 24 and 48 h after a single intravenous injection of the nanomaterials. Complete disappearance of tumor by group received Chito-NC-GNRs + laser irradiation. Reprinted with permission from ref. 221. Copyright 2011 American Chemical Society. | ||
Chuang and colleagues conjugated manganese magnetism-iron oxide (MnMEIO) to GNR clusters with an average size of 6 nm to allow the benefit of combined imaging (MRI) and therapy (PTT) abilities in one carrier for cancer therapy in tumor-induced mice by SKBR-3 (a human breast cancer) and Colo-205 (colon cancer) cell lines. They synthesized NPs with appropriate long-term physical stability, low toxicity, and good dispersity. Laser radiation with a wavelength of 808 nm and an intensity of (0 to 5) W cm−2 was applied for 10 min. After 20 to 30 days of treatment with GNPs under irradiation, all subjects remained alive compared with the control groups (mice treated with PBS, only laser, and only carrier) in which all subjects were dead. However, in groups that did not receive laser treatment, the tumor volume was close to that of the negative control group. The GNRs/MnMEIOs nanoclusters demonstrated transverse relaxivity about two-times more than commercial contrast agents and could destroy cancer cells efficiently by creating heat with exposure to an NIR laser. These results showed that the developed dual functional GNRs/MnMEIOs nanoclusters could be promising candidates for in vitro and in vivo magnetic resonance (MR) imaging diagnosis and PTT222 (Fig. 10). A schematic illustration of the GNP PTT in human tumor tissue is shown in Fig. 11.
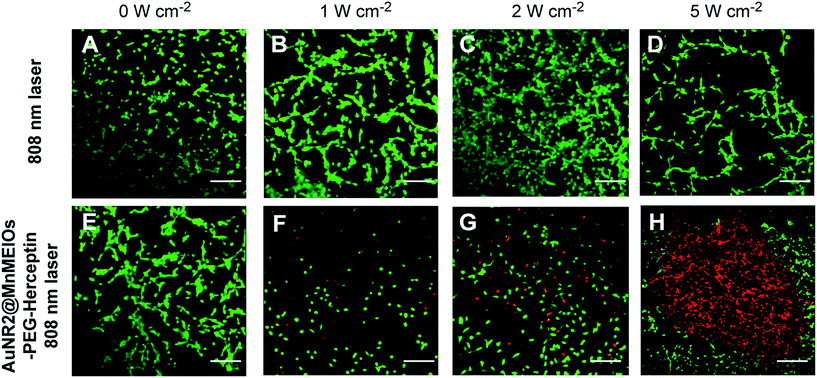 | ||
| Fig. 10 SKBR-3 cells incubated with GNRs/MnMEIOs-PEG-Herceptin at different power densities of 808 nm laser for 10 min. The first row demonstrates the laser alone and the second row shows the combination effect of GNRs/MnMEIOs-PEG-Herceptin and laser treatment. Each column shows cells treated at different laser power intensities (0 to 5 W cm−2). The green ones are viable cells (calcein AM staining) while the red ones are destroyed cells that (PI fluorescence). Reprinted with permission from ref. 222. Copyright 2014 Elsevier. | ||
3.1.1.4. Cancer PTT with GNRs and anticancer agents. Shen and coworkers tried to use combination therapy (PTT and chemotherapy drug) to kill A549 cell lines. In this study, gold nanorods encapsulated into doxorubicin (DOX)-conjugated mesoporous silica NPs with a size of 51 × 13 nm were irradiated with a laser beam power of 23 W cm−2 and wavelength of 808 nm. After radiation for 30 seconds, the temperature reached 66 °C. The authors stated that the simultaneous application of PTT and DOX (chemotherapy drug) caused a synergistic effect of two- to four-times, decreasing the tumor weight compared with the use of each single method223 (Fig. 12).
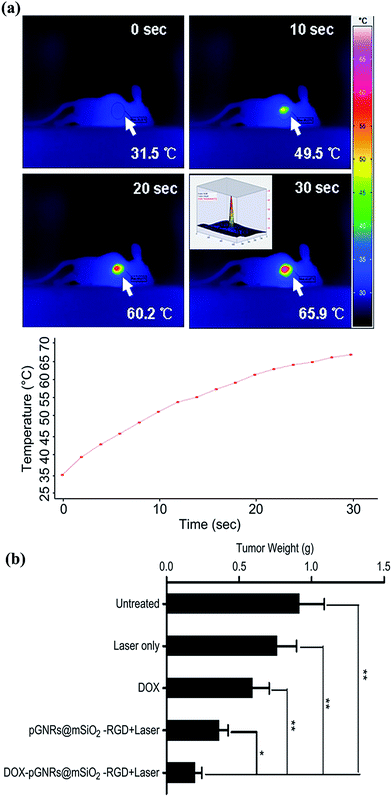 | ||
| Fig. 12 (a) Infrared thermal image of tumor-bearing mouse (808 nm with 3 W cm−2 power densities for 30 s) 2 h after intravenous injection. The color bar shows the relative temperature; (b) temperature changing curve in tumor during 30 s after NIR-laser irradiation. Reprinted with permission from ref. 223. Copyright 2013 Elsevier. | ||
In 2014, Tao and coworkers developed a novel DOX-loaded GNR (GNR-CpG-DOX) for a combination of chemotherapy and PTT in H22 cell lines (in vitro) and cancer-induced BALB/c mice (in vivo). The carrier size, radiated laser intensity, wavelength, and laser duration were approximately 25 nm, 1.5 W cm−2, 808 nm, and 10 min, respectively. After laser beam radiation to H22 cell lines treated with GNR-CpG-DOX, the temperature of the tumor cells increased above 55 °C and cells were photothermally destroyed, with a cell viability of below 20% compared with DOX alone and GNRs alone, with a cell viability of around 40% and 50%, respectively. In vivo results demonstrated that the tumor volume was dramatically increased up to 5-, 3-, 2.8- and 2-fold after administration of NIR, DOX, GNR + NIR, and GNR-CpG-DOX without NIR, respectively. On the other hand, GNR-CpG-DOX exposed to NIR kept the tumor volume constant, and even decreased it after 12 days of daily administration. In contrast with the in vitro results, GNR + NIR showed better performance than DOX in in vivo experiments. Both in vitro and in vivo assays revealed that this engineered vehicle exhibits significant antitumor efficacy.224
3.1.1.5. Combination of PTT and PDT in cancer treatment with GNRs. The clinically ideal phototherapeutic window for tumors is between 700 and 1100 nm, in which the debilitation of light by blood and soft tissues is small, allowing treatment of the deepest tumors. For PDT, light-activated PSs can produce reactive oxygen species (ROS), like singlet oxygen (1O2), free radicals, and peroxides, which can irreversibly harm tumor tissues. Unfortunately, most available PSs, such as hemoporphyrin and phthalocyanine, absorb light energy only over wavelengths smaller than 600 nm, which is a serious disadvantage for PDT. Therefore, substantial attempts have been made to produce novel PSs or the chemical modification of existing ones that have great absorption cross-sections in the NIR area.
At the beginning of 2012, Kuo and coworkers used polymer-coated GNPs with a positive charge surface and GNRs with a negative charge surface, and a size of 13 nm and 35 × 9.3 nm for PTT and PDT, to destroy malignant A549 cell lines. GNRs and GNPs were conjugated with Indocyanin Green (ICG) in order to create high photo stability and produce a promising diagnostic probe (ICG was destroyed at higher temperatures). Then, GNRs and GNPs decorated with ICG were conjugated to anti-EGFR antibodies to assist targeting therapy. The continuous beam was radiated with the wavelength, power, and duration of 808 nm, 222.5 W cm−1, and 3.5–8 min, respectively. The temperature in the cancer cell line was increased to 77 °C in the optimized conditions. The cell-death rate in the cancer cells treated with GNPs was greater than that in the GNRs, and the photochemical destruction capability on GNPs apparently increased depending on the size enlargement (up to 100 nm) of the GNPs. Interestingly, GNRs did not show significant cancer cell death. The interaction between GNPs, and ICG provided much greater photostability in ICG to highly enhance the imaging efficacy.225
Chen and colleagues prepared nanospheres from chitosan and ICG-coated GNRs (chitosan-GNR-ICG-NSs) for PTT and PDT in tumor-bearing mice. In their studies, continuous laser radiated to nanocarriers at a 808 nm wavelength and intensity of 2 W cm−2 for 10 min increased local tumor temperature to around 50 °C. In vitro cytotoxicity and in vivo antitumor efficiency examinations demonstrated that chitosan-GNR-ICG-NSs had a significantly superior antitumor effect than chitosan–ICG nanospheres, GNRs, or laser beam irradiation alone. The antitumor activity of chitosan–ICG was attributed to the induction of an immune response action by chitosan.226
Wang and coworkers coated GNRs with a positively charged polymer (poly allylamine hydrochloride) (average size, 47 nm) to attach a negatively charged Rose Bengal (RB) in order to investigate the combined PDT–PTT efficacy on human oral squamous carcinoma cell line (Cal-27) (in vitro) and cancer-induced male Syrian Golden hamsters (in vivo) against oral cancer. RB has specificity to oral cancer cells and is a well-known anionic PS that is able to produce ROS at a yield of 70% under 532 nm light irradiation to selectively damage tumor tissues. However, RB is a hydrophilic molecule and cannot be easily uptaken into solid tumors.227 TEM images indicated that by conjugation of RB on the GNRs, the intracellular accumulation of GNRs was increased almost four times. In vivo experiments indicated that RB–GNRs without light and with both NIR and green lights, without application of RB–GNRs, did not affect tumor growth. The results were the same in the control group. On the other hand, NIR with RB–GNRs resulted in almost twice the tumor growth inhibition compared with RB–GNRs with a green light. The application of RB–GNRs with both lights caused dramatic tumor growth inhibition (more than 100 times) in comparison with the control group. Therefore, it was concluded that the addition of RB not only caused higher localization of GNRs into the tumor cells, but also increased the therapeutic efficiency of GNRs by producing ROS.228 Table 1 presents further studies on plasmonic PTT based on GNRs.
| Particle type | Size | Laser radiation temperature | Significant remarks | Ref. |
|---|---|---|---|---|
| GNR-conjugated anti-EGFR | 11 × 40 nm | 800 nm/10 W cm−2/4 min | In vitro comparison between gold nanostructures declared that GNRs are more feasible for clinical trials | 113 |
| GNR-conjugated DNA and RNA aptamer + DOX | 10 × 40 nm | 808 nm/4 W cm−2/10 min/up to 42 °C | Multi-modular anticancer container which includes a prostate cancer-specific A10 RNA aptamer, a DOX–DNA complex, and light-stimulated heat-generating GNRs. Chemotherapeutic and PTT have synergistic effect on prostate tumor regression both in vitro and in vivo | 229 |
| Au–Ag dendritic + anti-EGFR | 400 nm | 808 nm/4 min 10–35 W | In vitro cell cytotoxicity of A549 cells treated with hallow Au–Ag dendrites compared with Au nanorods revealed that nanostructured dendrites needed lower particle concentration and laser power toward Au nanorods | 230 |
| Au capped magnetic core mesoporous silica shell | 300 nm | 808 nm/2 W/5 min/45 °C | Chemotherapy, photothermal therapy, MR imaging, dark-field optical and infrared thermal imaging combined simultaneously in one multifunctional nanoellipsoid. Enhanced therapeutic efficacy was observed from the DOX-Au capped magnetic core mesoporous silica shell in in vitro and in vivo studies | 231 |
| PEGylated GNR | 13 × 47 nm | 810 nm/2 W/2–5 min/55 °C | In vitro and in vivo PEG-NR, presented integration between computational therapy and nanotherapeutic | 232 |
| PEGylated GNR | 13 × 47 nm | 810 nm/0.75 W/15 min/45–49 °C | In vitro and in vivo studies indicated enhanced therapeutic efficacy of DOX/PEGylated GNR due to combination of photothermal heating and chemotherapy | 233 |
| Folic acid-conjugated silica surfaced modified GNR | 17 × 45 nm | 808 nm/40 W/3 min | In vitro and in vivo developed nanoprobe can offer effective selective targeting, excellent imaging, and targeting ability for X-ray/CT imaging with dual-mode enhanced radiotherapy and PTT ability | 234 |
| GNR–Fe3O4 PEGylated and conjugated Herceptin | 87 nm | 785 nm/4.53 W cm−2 5 min/55–60 °C | In vitro these nanoparticles are applied in MRI, fluorescence imaging and PTT | 235 |
| GNR coated poly caprolactone based micelles + DOX | 15 × 50 nm | 808 nm/0.2 W/10 min/80 °C | In vitro enhanced DOX release upon NIR irradiation in MDR MCF-7 cancer cells due to photothermally induced phase transition of polycaprolactone regime | 236 |
| GNR-conjugated folate | 12.5 × 46.5 nm | 765 nm/0.75–60 mW/20 min | In vitro GNR induced localized photothermal damage in the tumor cell membranes and evaluated necrosis in the cell | 237 |
| GNR-conjugated folate | 11 × 50 nm | 765 nm/147 W/30 s | In vitro GNR–folate selectively uptake on cell membrane and generating extensive blebbing of the cell membrane under irradiation | 238 |
| GNR/SiO2–DOX | 30 nm | 790 nm/24–48 W/8 min | In vitro multifunctional GNR–SiO2 theranostic nanoparticles applied for TPI imaging, drug payload and PTT. By combination of chemotherapy and hyperthermia cell viability decreased more than single treatment | 239 |
| GNRs with an oligonucleotide-capped silica shell + DOX | 11 × 41 nm | 808 nm/1.5 W/10 min | In vivo DOX–AuMS–dsDNA + PTT led to 30 and 50% greater decrease in cell viability in comparison to free DOX and GNR–silica shell | 240 |
| Folic acid-conjugated GNR/silica coated PEG + camptothecin | 11 × 40 nm | 808 nm/2 W/30 min | In vitro and in vivo novel targeted system was developed by integrating chemotherapy and PTT simultaneously; tumor volumes in treatment group with camptothecin–GNR/silica-PEG-FA nanoparticles decrease significantly. In vivo study showed six-times less cell viability toward non-treated group | 241 |
| Arginine-glycine-aspartic acid (RGD) peptide-conjugated polyamidoamine dendrimer-modified GNR nanoprobe | 10 × 42 nm | 808 nm/4–20 W 4 min | In vitro and in vivo effect of PTT on developed nanoprobe revealed tumor volume regression of one-fifth toward untreated group after 28 days of treatment | 242 |
| Au–Ag nanorod | 14 × 53 nm | 808/600 mW/5 min | In vitro they conjugated aptamer to nanostructures. Au–Ag NRs aptamer-labeled induced 93% cell death | 243 |
Hainfeld and colleagues synthesized PEG/lipoic acid-conjugated GNSps (15 nm) to study the synergistic effect of a combination of hyperthermia and radiotherapy on A431 cell lines and radioresistant subcutaneous squamous cell carcinoma (SCCVII) in mice. TCD50 (radiation dose required to control 50% of the tumors) for extremely radioresistant SCCVII tumors is 55.4 Gy.245 PEG and lipoic acid were decorated on the surface of GNSps to provide sufficient biodistribution and tumor tissue accumulation, respectively. It was shown that the TCD50 dose was reduced to less than 15 Gy, yielding an efficient healing dose. These results indicated that combined hyperthermia and radiotherapy led to a significant reduction in the X-ray dose needed to achieve a similar therapeutic outcome attained with X-rays alone, and therefore improved therapeutic results.246
The anti-EGFR-conjugated GNPs (40 nm) were examined for PTT in the same way as reported for GNRs by the same research team.202 The results were the same, indicating that malignant cells needed less than half the energy required to destroy the benign cells incubated with GNPs. Interestingly, the laser intensity did not cause cell death without NPs, and more than four-times the energy was required to kill the cells in the absence of NPs. Unfortunately, the beam characteristics and time of exposure were different in these two studies, therefore a valuable comparison of GNR and GNP efficacies in the PTT procedure is not possible.247
Jin and colleagues synthesized GNP-coated poly(lactic acid) microcapsules with a double-microemulsion water-in-oil-in-water (w/o/w) method as theranostic microcapsules. Graphene oxide was deposed on the microcapsule surface by an electrostatic layer-by-layer self-assembly technique. In this work, GNPs/PLA-(PAH/GO)n play the role of a contrast agent in CT and ultrasound (US) imaging, with graphene oxide as an NIR-light absorbing agent. The researchers conducted an in vivo acoustic test for US contrast behavior and CT imaging after intravenous injection of the microcapsules into white rabbits. The kidney of the rabbit was imaged and clear enhancements of the rabbit kidneys were seen; and the brightness increased with time. An X-ray CT test showed that the microcapsules have excessive potential for CT contrast imaging because elemental Au has a high X-ray attenuation due to its higher atomic number and electron density. Eventually, the photothermal effect of microcapsules in HeLa cell lines was tested. After 6 min exposure to a laser with a wavelength of 808 nm and radiation intensity of 2–6 W cm−2, cell viabilities decreased to below 10%. Next, the authors evaluated the in vivo photothermal effect on nude mice bearing human fibro-sarcoma HT 1080. After 10 min treatment with an NIR laser, the temperature of the microcapsules reached 54.6 °C in the tumor center with exposure to the 808 nm laser with a power density of 2.23 W cm−2. After 9 days' treatment, the tumor was completely ablated, with a tumor growth inhibition rate of 83.8% in the group of mice that had both microcapsules and NIR irradiation.248
The combination of PTT and gene delivery was investigated in a further study.249 Dense and hollow GNSps were synthesized and concurrently administered with LipofectAMIN™ condensed pAcGFP-1-Endo plasmid on HeLa cells. Dense GNSps showed superior cell damage than hollow ones. It was concluded that the combination of fatal PTT with sub-fatal levels of gene delivery caused a synergistic cytotoxic effect in vitro via an apoptotic pathway.249
The destructive effect of locally injected GNShs (Au shell on silica core) was investigated on the cancer cells of the ear, mouth, and skin followed by pulsed semiconductor laser (810 nm) irradiation. This manuscript suffered from lack of data on GNShs synthesis and characterization and application of proper control groups. The reported tumor inhibition activity of GNShs was not quantitative.196
The same type of carriers (silica based GNShs) with a size of 120 nm in core and 10–20 nm shell thickness were synthesized and coated with PEG to increase the circulation time and prevent non-specific adsorption. PEG-GNShs were injected via the tail vein of tumor-induced mice to assess the accumulation of NPs in the tumor and six different organs. PTT was carried out with a laser wavelength of 800 nm and an intensity of 4 W cm−2 for 3 min, and then tumor length and width were measured daily. None of the eight mice in the control group survived after 24 days (mean survival,13.3 days) while, in comparison, four of seven mice in the GNShs therapy group were still alive 90 days post-irradiation (overall survival, 57%) and, importantly, each of these mice was completely tumor free without sign of tumor recurrence250 (Fig. 13). Despite PEG conjugation of GNShs, a high level of NP accumulation was observed in the reticuloendothelial system (spleen and liver). Unfortunately, the PEG-free GNShs were not administered, and it is therefore not possible to compare specific and non-specific organ accumulation.
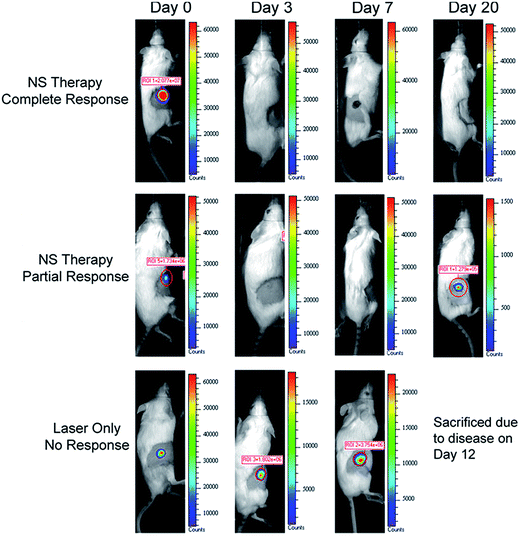 | ||
| Fig. 13 Bioluminescent imaging of tumors following laser irradiation. The mouse in the first row displayed loss of luminescence within 3 days of nanoshell therapy and remained tumor-free for the remainder of the study. The mouse in the second row experienced partial response to nanoshell therapy evidenced by initial loss in signal intensity, but the tumor later recurred. The third row shows a mouse from the control group in which signal intensity and tumor burden increased following laser irradiation. Reprinted with permission from ref. 250. Copyright 2010 Springer. | ||
In another study, PEG and anti-Mucin 7 monoclonal antibodies were conjugated on GNSps (47 nm) to prevent NP aggregation and to target them directly to four types of cancer cell lines. The cells were exposed to laser irradiation with various power densities (10, 20, 25, 30, and 35 W cm−2) and a wavelength of 532 nm (green light), and then cell viability was assessed using 0.4% trypan blue stain. The superiority of the antibody-conjugated GNSps to antibody-blocked NPs and laser alone was demonstrated in this study. The importance of PEG conjugation of GNSps was highlighted in this study because investigation of bare GNSps on cell death was precluded due to the difficulty of handling the experiment because of GNSp aggregation in the cell culture medium.122
Manuchehrabadi and colleagues investigated the PTT effect of GNRs (4 5 × 10 nm) on PC3-cell prostate cancer-induced BALB/c male mice. GNRs were locally injected to the center of the tumor when the tumors reached the desired size. Concurrently, the laser irradiance at the tumor surface was fixed at 1.6 W cm−2 at a wavelength of 800 nm for 15 min. The size of both tumors (treated and control group) was assessed for 25 days thereafter. On Day 0, the average tumors sizes were 691 ± 62 mm3 compared with approximately 44.7 mm3 on the 25th day after treatment. A comparison of the control group and treated groups (laser radiation + GNRs) indicated that a significant decrease in tumor size was observed in the treated group after the sixth day. On the other hand, the tumor size of the untreated group continued to grow and reached 2.5-times the initial size after 25 days. Limitations of this study were the short study time of 25 days after the heating experiments. Ideally, the tumor evaluation period should be extended to confirm that the tumor does not start to regrow.251 Unfortunately, both treated and control groups were evaluated on one mouse. The growth of the control group made the rest of the experiment impossible. Table 2 summarizes further studies on PTT based on gold nanoshells and nanospheres.
| Particle type | Size | Laser radiation temperature | Significant remarks | Ref. |
|---|---|---|---|---|
| GNSh coated with carboxylate polystyrene (GNCPSs) | 200 nm | 808 nm/4 W 10 min/55 °C | In vivo the tumor volumes in mice that received GNCPSs were significantly lower than the nontreatment group and laser-only treatment groups, with an average inhibition rate over 55% (p < 0.005) | 205 |
| SiO2/Au core–shell | 170 nm | 808 nm/2 W 2 min/60 °C | 252 | |
| Liposome/SiO2/Au core–shell–shell | 238 nm | 808 nm/15 min 100 mW | In vitro investigation of the effect of DOX-loaded in liposome/SiO2/GNSh synergistic effect with photothermal therapy. Cell growth inhibition rate was about 13% in DOX free treated group and 57% for liposome/SiO2/Au without laser. It was 81% for liposome/SiO2/Au via laser irradiation | 253 |
| GNSh microcapsules PHA | 2000 nm | 808 nm/8 W 10 min/55 °C | In vitro multifunctional theranostic nanoparticles for ultrasound imaging and photohyperthermia were constructed with a decrease in cancer cell viability below 10% | 254 |
| SiO2/Au core–shell conjugated anti-HER2 | 120 nm | 820 nm/0.008 W/7 min | In vitro developed dual imaging/therapy immune-targeted nanoshells could provide scattering contrast for imaging while also exhibiting sufficient absorption to enable effective PTT | 255 |
| SiO2/Au core–shell conjugated cyclo-(RGDfK), integrin αvβ3 targeting peptide | 140 nm | 808 nm/1.2 W/5 min/47 °C | In vitro and in vivo integrin αvβ3 targeting using RGDfK improved NS accumulation in tumors which offers a class solution to the challenge posed by heterogeneity of tumor-specific antigens across diverse tumor types | 256 |
| Hallow GNSps conjugated anti-EGFR monoclonal antibody C225 | 40 nm | 808 nm/4 W 3 min/65 °C | In vivo in areas where temperature reaches >54 °C, irreversible cellular damage would occur, whereas in areas where the temperature is lower than the thermal death threshold, enhanced tumor uptake of polymeric drugs would ensure sufficient cell killing. Furthermore, tumor necrosis percent reach to 70% when in PTT induced mice treated with C225–HAuNS | 257 |
| PEGylated hallow GNSps attached with [Nle4,D-Phe7]α-melanocyte-stimulating hormone MSH (NDP-MSH) | 47 nm | 808 nm/0.5 W/1 min and 32 W cm−2, 3 min | In vitro and In vivo receptor-mediated active targeting of melanoma and efficient PTA with photothermal coupling agents was achieved in vivo. In vitro tests showed most cells that were treated with NDP-MSH-PEG-GNS plus NIR laser were dead with necrosis | 258 |
| Anti-HER2 immuno gold–silica nanoshells | 111 nm | 820 nm/4 W 2 min | In vitro NIR-laser treatment results showed that cell viability reach to 20% in HER2-positive (KB) cells while HER2-negative (HeLaS3) cell viability did not change in anti-HER2 immuno gold–silica nanoshell treated groups | 259 |
| PEGylated GNShs conjugated with cyclic RGD peptides | 40 nm | 808 nm/16 W 3 min/57 °C | In vivo brain tumor of mice treated with RGD–PEG–AuNS + laser group could survive 25 days and when tumor began regrowth they died up to 31 days, while mice in the control groups died between 17 and 21 days | 260 |
| PEGylated (Au shelled UCNP–Fe3O4) | 180 nm | 808 nm/1 W 5 min | In vivo multifunctional nanoparticles were developed for in vivo dual modal for up-conversion luminescence (UCL)/MR multimodal imaging as well as PTT targeted by the magnetic field which led to an excellent PTT efficacy with 100% tumor elimination in a murine breast cancer model | 261 |
| Fe3O4 core/hybrid/Au shell | 120 nm | 808 nm/2 W 5 min/60 °C | In vivo | 262 |
| Bacteria/Au core/shell | 10–12 nm | 808 nm/6 min 60 mW | In vitro E. coli DH5a was used for fabrication of bacteria/Au core/shell for cancer therapy. Results showed cell viability in the DH5a/Au treated group dropped to 80% while the DH5a-treated group dropped to zero after 8 days | 263 |
Han and coworkers synthesized hollow GNFs in the size range 115–153 nm. GNF was constructed using vesicles with a multi-amine head surfactant. The PTT effect of these novel GNFs was studied on HeLa cells (in vitro) and HeLa-tumor-bearing female BALB/c mice (in vivo). GNFs exhibited a very strong photothermal effect even at small doses, and the increases in the size of the GNFs effected an improvement of biosafety under visible light and cytotoxicity under NIR irradiation due to the difficulty of larger GNFs entering the cell without NIR irradiation, but ease of cell penetration at the elevated temperatures caused by NIR irradiation. The researchers used a red light laser at 808 nm for 5 min with a power density of 9 W cm−2. The temperature reached 70 °C. The cell viability of the control group (GNFs) was 100% while the treated group (NIR laser + GNFs) decreased with increasing NP size and concentration, and reached almost 0% with GNFs in the size range 145–153 nm. An in vivo study of the tumors in mice was monitored for 20 days, and interestingly the tumor disappeared in the treated group (NIR + GNFs) at the end of treatment but, on the other hand, tumor volume increased in the control groups (NIR only).271
Branched GNPs are potential PTT agents due to their large absorption cross-section in the NIR window. Therefore, branched GNPs can generate sufficient heat to eliminate tumor cells. Broek and colleagues synthesized branched GNPs (60.4 nm) conjugated with anti-HER2 (an antigen which is highly expressed in breast and ovarian cancer cells) and anti-PSA antibody (as a negative control) and investigated the PTT performance of these NPs in vitro on two HER2-positive and negative cell lines (human ovarian epithelial carcinoma cell line [SKOV3] and a Chinese hamster ovary cell line [CHO], respectively). A continuous laser of 690 nm wavelength and 38 W cm−2 power density was radiated for 5 min using live/dead staining to evaluate viability. Branched GNRs showed specific photothermal destruction of the SKOV3 cell line (HER2 positive), whereas the control groups (NPs alone, laser alone and anti-PSA antibody-conjugated NPs with laser) did not show any cell death. This high specificity in targeting GNPs is interesting in in vitro experiments, while anti-PSA antibody-conjugated NPs, if not endocyted into cells, were close to the cells and probably could damage the cells by heat generation upon laser irradiation on the cell line.159
Huang and coworkers developed a novel green chemistry synthesis method to fabricate GNFs by the reaction of HAuCl4 solution with the chiral nucleotide, guanosine 5′-monophosphate (5′-GMP) and the chiral reducing agent, L-ascorbic acid (L-AA). This green method resulted in the production of GNFs with excellent biocompatibility (greater than 90% cell viability even until the application of GNFs in the concentration of 200 μmol L−1). The PTT efficacy of GMP-capped GNFs was successfully tested in vitro on MGC803 cells with exposure to He–Ne laser with a wavelength of 632.8 nm, and power density was about 30 mW cm−2. Gold nanomaterials are also Raman active substrates due to strong SERS enhancement and therefore can be used for imaging. The as-synthesized GNFs with excellent biocompatibility can be applied to SERS enhancement, cellular dark-field imaging, and PTT. The synthesized GNFs showed a noticeable SERS enhancement due to their coarse surface and dense tips, both of which enhance the surface area and form a large number of “hot spots”.272
In an interesting study, the simultaneous PDT/PPTT treatment was reported by proposing a new therapeutic strategy using Chlorin e6 (Ce6, a commonly used PS)-functionalized gold nanostars (GNSt-PEG-Ce6). PEG provides outstanding dispersivity and stability in a range of solutions. In order to investigate the synergistic PDT/PPTT effect of GNSt-PEG-Ce6, in vitro and in vivo studies were conducted on A541, MDA-MB-435 cell lines, and MDA-MB-435-tumor-bearing mice models, respectively. Laser radiation with an intensity of 7 W cm−2 and a wavelength of 671 nm for 6 min was applied, and a local temperature increase of more than 25 °C was observed. GNSt-PEG-Ce6 showed almost 50% cell death in an in vitro experiment, while no notable result was observed for GNSt-PEG, indicating the synergistic effect of PDT and PTT. The application of GNSt-PEG-Ce6 + NaN3 confirmed the role of PDT in the therapeutic performance of NPs because of the ROS scavenging action of NaN3. These results are supported by the fluorescence image of MDA-MB-435 cells incubated with various test and control groups. The enhanced in vivo therapeutic efficiency was confirmed by comparing tumor size, histologic examination, and ultrasound and photoacoustic imaging of the tumor in the GNSts-PEG-Ce6-treated group compared with those in PBS, free Ce6, and GNSts-PEG treated groups. This result was in good agreement with in vitro studies.273
Gold nanocages (GNCs) have been claimed to show more tunable powerful scattering and absorption in the NIR region than other gold nanostructures such as nanoshells or nanorods.274 Gao and colleagues developed GNCs coated with PS (hypocrellin B)-loaded liposomes for PTT/PDT cancer therapy. GNCs (edge length, 45 nm; wall thicknesses, 5 nm) were synthesized by galvanic replacement reaction between Ag nanocubes serving as the sacrificial templates and HAuCl4. Liposomes were synthesized with hydrogenated soybean phosphatidylcholine (HSPC), distearyl phosphatidylethanolamine (mPEG2000-DSPE), cholesterol, and Hypocrellin B (HB). To investigate the combined PTT/PDT synergist effect, the developed lipid-HB-GNCs were treated with HeLa cells and exposed to NIR irradiation (790 nm, 85.5 pJ per pulse for 300 s). PDT with HB-loaded nanoliposomes and PTT with blank nanoliposome-coated GNCs led to cell viabilities of 54.5% and 64.6%, respectively. A remarkable reduced cell viability (17.4%) was observed when the combination of the two treatments was administered with a single irradiation.203
Aptamers are single-stranded DNA or RNA (ssDNA or ssRNA) molecules that can bind to pre-selected targets including proteins and peptides with high affinity and specificity. Carbon nanotubes (CNTs) are allotropes of carbon with a cylindrical nanostructure. Single-walled CNTs (SWNTs) have a diameter close to 1 nm, and can be many millions of times longer. CNTs are known for their improved PTT effect when exposed to photons under NIR radiation.275,276
Afrin Khan and coworkers used GNC–SWCNT hybrids for targeting and PTT of cancer cells. SWCNTs were attached to GNCs using the –SH linkage through para-aminothiophenol, then modified with A9 RNA aptamer. The PTT effect of the developed A9 RNA aptamer-attached GNCs–SWCNT was then evaluated on prostate cancer cells under NIR (Nd:YAG laser 1064 nm NIR with power density of 1–2 W cm−2) for 10 min. Their results showed greater than 95% cell death for cells treated with developed antibody-conjugated GNCs-SWNTs, while aptamer-attached antibody-conjugated GNCs exhibited only 2% cell death.277 The observed results challenge the efficacy of GNCs on PTT, despite claims of the superiority of cage-shaped nanogolds in comparison with other shapes.
The application of GNCs for in vivo PTT therapy is restricted due to their short blood circulation lifetime that affects their tumor uptake. Piao and coworkers used red blood cell (RBC) membranes and poly(vinylpyrrolidone) (PVP, MW ∼50![[thin space (1/6-em)]](https://www.rsc.org/images/entities/char_2009.gif) 000) for the surface coating of GNCs to overcome the short lifetime in blood circulation. An in vitro cell-uptake study showed tumor uptake with a 1.7–1.9-fold increase for RBC-GNCs versus PVP-GNCs. Furthermore, in vivo studies on tumor-induced mice after 45 days showed a 100, 80, and 20% survival rate for mice groups that received RBC-GNCs, PVP-GNCs, and PBS, respectively. It is important to note that, in addition to better tumor uptake, the RBC-GNCs revealed considerably reduced accumulations within certain non-target major organs (liver, lung, and kidney) compared with the PVP-GNCs 48 h after injection (p < 0.05).278
000) for the surface coating of GNCs to overcome the short lifetime in blood circulation. An in vitro cell-uptake study showed tumor uptake with a 1.7–1.9-fold increase for RBC-GNCs versus PVP-GNCs. Furthermore, in vivo studies on tumor-induced mice after 45 days showed a 100, 80, and 20% survival rate for mice groups that received RBC-GNCs, PVP-GNCs, and PBS, respectively. It is important to note that, in addition to better tumor uptake, the RBC-GNCs revealed considerably reduced accumulations within certain non-target major organs (liver, lung, and kidney) compared with the PVP-GNCs 48 h after injection (p < 0.05).278
The several sharp spikes in GNSt noticeably increase the local electromagnetic field, mainly due to stronger SERS enhancement, better two-photon action cross-section, and superior photothermal conversion effectiveness than other shapes of GNP.114,279 This unique structure has made GNSt a useful multimodality theranostic nanoprobe.
Liang and coworkers conjugated CD44v6 monoclonal antibody (a molecular marker for identification of human gastric cancer) on PEGylated GNSts and evaluated PTT and the photoacoustic imaging effect on gastric cancer stem cells. GNSt-PEG and GNSt-PEG-CD44v6 NPs with an average particle size of 90 nm were injected into gastric cancer tumor-bearing mice then exposed to NIR irradiation with a diode laser at 790 nm for 5 min with 1.5 W cm−2 power intensities.280 Both GNSt-PEG and GNSt-PEG-CD44v6 revealed little cytotoxicity at doses up to 200 μg mL−1. In vitro cellular uptake indicated more than 83% of GNSt-PEG-CD44v6 internalization to the gastric cancer stem cells, while no evident intracellular uptake was observed in the control group (GNSt-PEG). In vivo studies indicated that the tumor accumulation of GNSts-PEG-CD44v6 was more than two-fold higher than the control group, indicating effective targeting capability of the functionalized GNSt toward the gastric tumor. Additionally, to confirm the effectiveness of targeting, biodistribution of NPs in different organs was investigated and found that the antibody conjugation decreased the non-specific accumulation in the spleen, liver, brain, kidney, heart, and lung.
Photoacoustic imaging study on targeted distribution of GNSt-PEG-CD44v6 indicated that GNSts are excellent contrast agents for in vivo photoacoustic tomography, with a detection limit of 1 ppm (∼1 μg mL−1).281
Wang and colleagues synthesized GNSts (particle size, ∼124 nm) as a dual-sensitive PS for PTT/PDT in cancer treatment and a contrast agent for X-ray imaging. Interestingly, in this study, GNSts treated with 808 nm NIR laser for 15 min per well (300 mW cm−2) was able to generate ROS in addition to its photothermal efficiency. The cell death of GNSt-treated breast cancer cells (MCF7) related to PTT and PDT was 27% and 30%, respectively, which indicated that both PTT and PDT were carried out under the same NIR-light source. Furthermore, the impact of PDT on cell death was stronger than that of PTT. This report is inconsistent with previously published articles regarding the stronger performance of PTT compared with PDT.282,283 The TGI and X-ray imaging showed the great potential of GNSts for simultaneous cancer diagnosis and therapy. Histological analysis of the tumor tissue indicated no damage in the tumors treated with normal saline, normal saline + NIR, and GNSts. However, a noticeable reduction in tumor volume was observed in an in vivo study. Moreover, apoptotic and necrotic tumor cells were monitored in the GNST + NIR treatment group.284
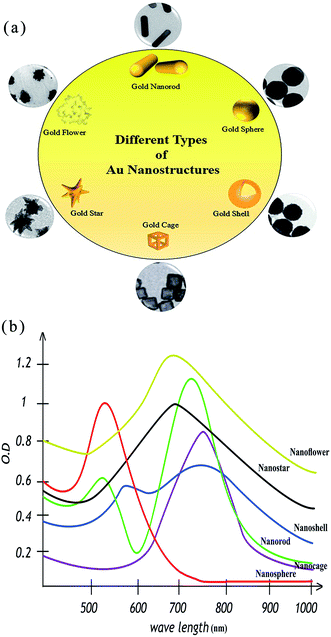
Liu and colleges synthesized a GNSt-probe for multimodality theranostics including SERS detection, X-ray CT, two-photon luminescence (TPL) imaging, and concurrently PTT. GNSts were synthesized with a novel method without the use of the toxic surfactants usually needed for GNS preparation, which enhances the biocompatibility of the produced GNS.285 In a complementary study, this research group synthesized GNSts at sizes of 30 and 60 nm and compared both imaging capability and PTT efficiency of GNSts. Both 30 and 60 nm GNSts showed almost the same imaging performance, which was considerably better than with GNSps (12 nm), but the 30 nm GNSts exhibited 2.4- and 1.2-fold higher tumor uptakes and bio distribution half-lives than the 60 nm GNSts. The in vitro photothermal heating evaluation and PTT efficiency percentages of 30 and 60 nm GNSts and GNShs were 42.3, 41.4 and 34.7 °C and 94%, 90%, and 61%, respectively. This indicates (a) the superiority of GNSts to GNShs and (b) the dominance of 30 nm GNSts compared with 60 mm GNSts. Furthermore, TPL imaging indicated that 30 nm GNSts penetrated more deeply than the 60 nm particles into the cancer tissue. The 30 nm GNSt-treated group exposed to an NIR laser with a 980 nm wavelength and 0.7 W cm−2 laser power for 10 min demonstrated no tumor recurrence in tumor-induced mice after 7 days.286 A schematic illustration of the different types of GNP, with different surface functionalization, used in PTT is shown in Fig. 14. Further studies on PTT based on other shapes of GNP are summarized in Table 3.
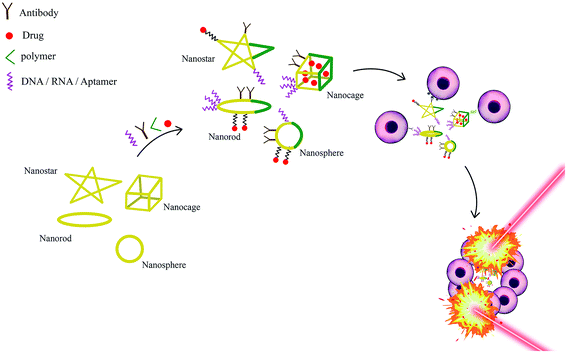 | ||
| Fig. 14 Schematic illustration of different types of gold nanoparticles with different surface modification using in photothermal therapy. | ||
| Particle type | Size | Laser radiation temperature | Significant remarks | Ref. |
|---|---|---|---|---|
| GNPs conjugated with DOX and Herceptin | 186 nm | 810 nm/5 W 10 min/+16 °C | In vitro multitargeted GNPs conjugated with DOX and Herceptin couples three modalities: targeting, stimuli responsive release, and thermal ablation which cause significant decrease in cell viability in comparison to control groups | 287 |
| PEGylated GNCs conjugated with anti-Her2 | 65 nm | 805 nm/0–6 W 0–10 min | In vitro immuno GNCs targeting and photothermal therapeutic effects on SKBR-3 breast cancer cells was quantified and the cell death affected strongly by laser power and exposure time | 288 |
| PEGylated GNPs | 16 nm | 808 nm/400 mW 1 min | In vivo and in vitro a developed system with greatly enhanced uptake by cancer cells was prepared from surface modification of PEGylated GNPs with mixed-charge zwitterionic self-assembled monolayers. In vivo study showed the tumor weight of mice treated with this system was half that of the control group | 289 |
| GNPs–IONP PEG coated | 230 nm | 808 nm/1 W 5 min/50 °C | In vivo and in vitro multifunctional nanoparticles which combined optical, PTT and magnetic properties simultaneously that targeted by the magnetic field was developed for in vivo application | 290 |
| PEGylated GNCs | 48 nm | 808 nm/0.7 W 10 min/53 °C | In vivo survival ratio at laser-treated tumor groups were one-fourth-fold of untreated ones with a greater intra-tumoral distribution of nanocages at the outer surface of the tumor than the inner core | 291 |
| Gold nano popcorns conjugate with anti-PSMA Rh6G and A9 RNA aptamer | 43 nm | 785 nm/80–120 mW/30 min | In vitro selective sensing, PTT, and monitoring of therapy progress | 292 |
| HER2-antibody-conjugated PEGylated GNCs | 45 nm | 810 nm/105–407 W/5 min | In vitro at a power density of 1.2 W cm−2 cell viability decreased to 10% in treated group with nanocage | 293 |
| Transferrin-conjugated PEGylated GNPs | 50.5 nm | 530 nm/407 W/5 min | In vitro multifunctional transferrin-conjugated GNPs were developed for targeting, imaging and PTT of cancer cells. The results indicated six-times more cellular uptake, two orders of magnitude lower laser power effective for PTT and excellent targeting ability of transferrin-conjugated GNPs | 294 |
| PEGylated GNSt | 50 nm | 980 nm/15 W 5 min/60–80 °C | In vivo and in vitro in vivo photothermal ablation was observed right at the laser spot on a mouse injected with PEGylated nanostars but not with PEGylated nanospheres | 295 |
| GNPs coated-Arabic Gym | 40 nm | 532 nm/5 min 182.5 mW | In vitro the irradiated cells treated with GNPs coated-Arabic Gym underwent localized mechanical destruction by the formation of explosive microbubbles | 296 |
| Antibody-conjugated magnetic/silica/gold nanocomposite | 120 nm | 820 nm/35 W 5 min | In vitro a novel multifunctional magnetic-nanoparticle core–silica–gold nanocomposite shell gold nanocomposite system as an MR contrast agent and an effective hyperthermal therapeutic agent. The PTT results revealed the superiority of this system for targeted cells in comparison to non-targeted cells | 297 |
| GNPs coated with CCK2 receptor loaded liposome | 100 nm | 760 nm/10 mW 2 min/55 °C | In vitro new diagnostic and therapeutic approach was developed by combination of gold-coated liposomes and laser-mediated receptor release | 298 |
| Smart GNPs | 10 nm | 660 nm/5–13 W/10 min | In vitro these smart GNPs could respond to pH change. Therefore, in an acidic environment or inside cells they can aggregate. The smart GNPs show selective and efficient destruction of cancerous cells with an intensity threshold of 8 W cm−2 to induce the thermal destruction | 299 |
| Photosensitizer (CE6) loaded PEGylated gold vesicles (GV) | 281 nm | 671 nm/2 W 3 min/50 °C | In vivo and in vitro the developed system has high simultaneous tri-modality NIR fluorescence/thermal/photo acoustic imaging and synergistic PTT/PDT combination treatment ability | 300 |
| DOX-conjugated smart GNPs | 100 nm | 660 nm/8–20 W/1–5 min/44 °C | In vivo and in vitro DOX conjugated GNPs used in this study were a smart thermo/chemo combination cancer therapy with higher cellular uptake, pH dependent aggregation in cell nuclei and more cellular damage than control groups by apoptosis | 301 |
| GNPs conjugated with DOX and DNA aptamer | 13 nm | 532 nm/2 W/0–35 min/80 °C | In vitro CCRF-CEM Tcell they synthesized DOX-loaded aptamer/hairpin conjugated GNP and incubated them via CCRF-CEM T cells. Increasing laser power causes a decrease in cell viability in DOX, sgc8c/hp-GNPs treated group while free DOX did not show any noticeable decrease in cell viability | 302 |
| GNPs coated amphiphilic block copolymer | 14, 20, 30, 40 nm | 808 nm/1 W/5 min | In vivo laser irradiation + NPs treated mice group showed complete elimination of tumors after 1 day but only laser and control group had three fold increase in tumor volume | 303 |
| GNCs core/silica shell coated with PNIPAM + DOX | 200 nm | 808 nm/1 W/5 min/50 °C | In vitro developed nanocarrier can attain the synergistic chemophotothermal therapy outcome and notably increased cancer cell killing efficacy. Viability of cells treated with DOX-loaded nanocarrier + laser reduced cell viability to 20% in comparison to 85 and 80% for carrier + DOX and carrier + laser, respectively | 304 |
| Peptide conjugated PEGylated GNSt | 70 nm | 850 nm/0.2 W/3 min | In vitro the results indicated an efficient photothermolysis at an ultralow irradiance (0.2 W cm−2), which is the lowest value ever reported for pulsed laser powers. Also peptide conjugation causes an increase in cellular uptake and a higher cell-death rate after PTT than control groups | 305 |
In a comparison study, Sibille and colleagues investigated the necrosis induced by CW and pulsed lasers with the same energy levels in the rat liver. This study demonstrated no substantial difference in the tissue necrosis stimulated by the two modes of laser in the rat liver. The only difference achieved at a precise power and duration (20 W, 2 s) was the induction of a deeper tissue necrosis by the pulsed mode. This trend was in contrast with the results of Mordon and Rebeiz, but was in agreement with the previous work of the same research group.309,310 Compton and coworkers studied the effect of pulse-laser exposure in bubble formation (with a nanosecond to microsecond life time) that led to cell lysis and cell necrosis. Shorter pulse durations could be effective in cell necrosis, whereas a 540 ps duration pulse was the optimal condition for cell permeabilization.311
Huang and coworkers conducted a comparative study on the efficiency and cell-death pathways of CW and nanosecond-pulsed laser photothermal cancer therapy by GNSps transported both to the cytoplasm and the nucleus of cancer cells. The results of another comparative study on the efficiency and cell-death pathways of CW and nanosecond-pulsed laser on the cytoplasm and nucleus accumulated GNPs indicated that cell death can be encouraged with a single pulse of a nanosecond laser more effectively than with a CW laser. The CW laser was more effective in cell destruction when GNSps were localized in the cytoplasm than in the nucleus. CW laser stimulated cell death via apoptosis, while the nanosecond-pulsed laser led to cell necrosis.312,313 In contrast, Li and colleagues believed pulsed laser irradiation to have both an apoptosis and a necrosis effect.314 Furthermore, pulsed-mode irradiation can generate singlet oxygen more effectively than CW.315 Pulsed laser generally has a high energy which causes rapid and massive heat creation and bubble formation around the nanoparticles.117 To support the findings of Huang et al. in introducing the necrosis pathway proved by a qualitative imaging method, quantitative FACS flow cytometry is required for a more precise judgment about the cell-death pathway.
The formation of gold nanoclusters on cell membranes increases the efficiency of bubble formation, resulting in damage to breast cancer cells at a relatively low laser fluence of 3–5 mJ cm−2.316 In cancer treatment based on laser-irradiated GNPs, there is great uncertainty regarding the killing of healthy cells. To clarify this problem, a nanophotolysis approach for the selective killing of malignant cells is applied. In a study by Ashiq and colleagues, different-sized GNPs (10, 20, 30, 40, and 50 nm) were synthesized and the effect of the pulse duration in the range of 10–30 ns with 5 mJ cm−2 laser fluence, as well as the effect of GNP size, on breast cancer cell damage was investigated. These researchers demonstrated that the formation of a bubble with a radius of 9 μm around the nanoparticle could effectively kill the breast cancer. These bubbles were generated due to short-pulse laser irradiation. According to these results, the tumor penetration of the GNP and the radius of the bubble were increased with GNP size and pulse duration time.317
Zharov and colleagues synthesized F19 antibody-conjugated GNPs (40 nm) to selectively destroy MDA-MB-231 cell by nanophotothermolysis on three different short-pulse laser wavelength (420, 570, 1064 nm) for 8–12 ns. The laser fluence was about 0.1–10 J cm−2, and the results show that when the nanoclusters formed on the cell surface, cell viability decreased to 5% for a 532 nm laser and to 10% for a 1064 nm laser. The size of the bubbles produced at high energy levels was close to the size of the cells which caused the cell to rupture into different fragments.318 This research group also worked on a 420–575 nm short-pulse laser for 8 ns with 0.1–300 μJ pulse energy.319 When the MDA-MB-231 cell was treated with Ab-conjugated GNPs and exposed to pulsed laser, the percentage cell death reached 90% in comparison with the control group that was under 10%. The researchers found that enhancement of the bubble formation occurred when the GNPs aggregated into nanoclusters on the cell surfaces.
In a newly developed method, Hleb and coworkers were able to achieve the selective elimination of tumors using bubble generation with GNP clusters in the tumor tissue. C225 antibody-conjugated GNShs (171 nm), GNSps (20, 30, and 40 nm) and GNRs (13 × 45 nm) were synthesized, and of these GNRs were used to treat the cancer cell lines due to high yield of synthesis, followed by photothermal bubble generation with pulse laser (750 nm, 10 ns, 0–10 J) and induced cell destruction onto the cells and tumor. The bubble size reached 10–20 μm and had a life time of 1 μs. This result indicated that small nanoparticles provide a larger bubble than larger nanoparticles. Cell damage analysis revealed that cell death occurred by membrane destruction that induced after laser pulses and bubbles generation.320
The enhanced performance of GNPs by conjugation with cell-targeting antibody and application of short laser pulses was investigated.321 Peripheral blood lymphocytes were treated with Ab-conjugated GNPs and irradiated with 532 nm short-pulse laser with 20 ns duration at 0.5 J cm−2 which caused quick heating of the particles and vaporization of a thin layer of fluid surrounding each particle, making a microscopic version of an underwater explosion and cavitation bubble formation leading to cell damage. The results demonstrated more than 95% cell death in anti-CD8 immune-GNPs compared with only 5% of cells treated with 500 GNPs per cell.
Nedyakow and coworkers investigated the PTT effect of GNPs with two different particle sizes (40 and 100 nm) on a human cervical cancer cell line (HeLa) in vitro with pulse-laser irradiation at a wavelength of 532 nm and pulse duration of 15 ns. The repetition rate of the laser radiation was 1 Hz. Two, three, or 10 laser pulses with energy densities of F = 80 mJ cm−2 and F = 25 mJ cm−2 were used to irradiate the samples. The study was conducted in four groups: control; laser without irradiation; 40 nm GNPs + laser; and 100 nm GNPs + laser, with different pulse repetition and intensity. The results of this study showed that control laser treatment had no toxic effect on the cells. A stronger cytotoxic efficiency was observed for 100 nm particles compared with 40 nm particles. The results indicated that smaller particles cool down more rapidly than larger ones, leading to a stronger effect on the surrounding medium.322 In addition, we discuss several pulsed laser PTTs in this review.196,203,323
In a contrasting finding, Kessentini and colleagues concluded that GNCs could absorb light in a more efficient way than the other GNPs (GNRs, hollow GNSps, and GNShs) and could probably act in a more effective way in cancer PTT compared with the others.325
Maltzahn and coworker synthesized PEGylated GNRs (47 × 13 nm) and GNShs (core, 120 nm; shell, 15 nm) and exposed them to the 810 nm diode laser for 5 min with a power density of 2 W cm−2. The results showed that GNRs generated heat six-times more rapidly than GNShs. Consequently, incubation of GNRs with MDA-MB-435 human tumor cells in vitro caused extensive damage, while GNShs showed only a moderate toxicity in the same levels of NIR light.232
3.2. Plasmonic photothermal therapy in bacteria
Increases in the prevalence of antibiotic-resistant bacteria necessitate novel approaches for the treatment of infectious bacterial pathogens. Nanotechnology-driven approaches using GNPs PTT can be successfully implemented to control bacterial growth and destroy pathogenic bacteria. We have explored this approach as discussed below. A schematic illustration of the GNP PTT in bacteria is shown in Fig. 15.Staphylococcus aureus is one of the main pathogens threatening human health, and is responsible for a wide range of antibiotic-resistant infections. Zharov and coworkers developed a new method for the selective killing of Staphylococcus aureus by targeting monoclonal anti-protein-A-conjugated GNPs to the bacterial surface antigen. A 532 nm wavelength laser with 100 pulses for the duration of 12 ns each was used. Among different-sized GNPs (10, 20, and 40 nm), the largest showed the best non-linear PT responses. Although 40 nm GNPs illustrated a good PT response, their bacterial killing rate was not significantly different from the control group. Ab-conjugated GNPs decreased the bacterial survival rate from 70% to below 10% (ref. 323) (Fig. 16).
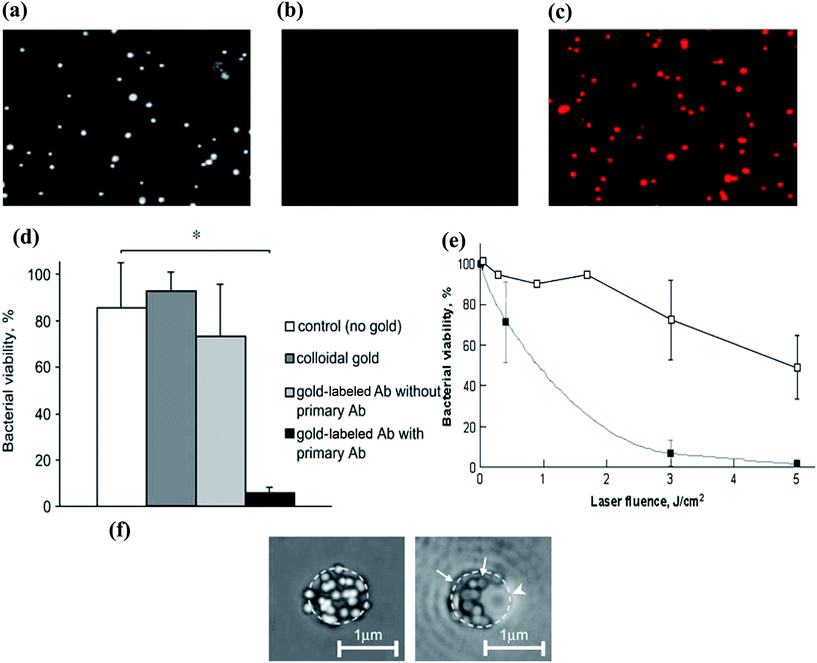 | ||
| Fig. 16 Antibody-conjugated gold nanoparticles binding with S. aureus. (a) Phase contrast; (b) fluorescent images of bacteria labeled with secondary antibodies and Alexa Fluor 594 without (primary antibody); (c) primary antibody labeled with Alexa Fluor 488; (d) bacterial viability evaluated after laser exposure (532 nm, 12 ns, 3 J cm−2); (e) bacterial viability to laser fluence diagram of S. aureus targeted via gold nanoparticles (0–5 J cm−2). Results are calculated using colony counting. The open squares show samples irradiated without gold nanoparticles and the solid squares have involved gold nanoparticles; (f) TEM images of S. aureus conjugated with gold nanoparticles with laser irradiation. The arrowhead shows a bubble around one nanoclusters. Laser fluence was of 3 J cm−2 at one. Reprinted with permission from ref. 323. Copyright 2006 Elsevier. | ||
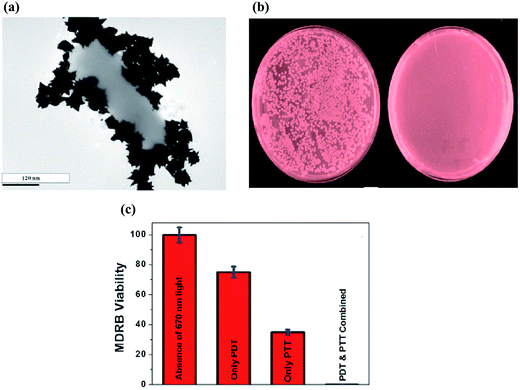 | ||
| Fig. 17 (a) TEM image demonstrating an antibody-conjugated multidrug-resistant-bacteria-attached with multifunctional nanoplatforms; (b) absence (left) presence (right) of a “multifunctional nanoplatform” combined therapy; (c) plot demonstrating the multidrug-resistant-bacteria viability after laser exposure (670 nm, 12 min) – each column shows the case of PDT, PTT, combined therapies, and absence of laser exposure. Reprinted with permission from ref. 342. Copyright 2011 American Chemical Society. | ||
To increase the antibacterial efficacy of vancomycin, it was conjugated to GNPs (Van/GNPs) and used against the antibiotic-resistant microbial strains under irradiation of NIR light (808 nm). Different bacteria-resistant strains received Van/GNPs + laser, GNPs + laser and laser alone, and it was found that the survival fraction of bacteria was significantly decreased after PTT treatment with Van/GNPs by >1000- and 20-times more than laser alone and GNP + laser, respectively, while the damage to human epidermoid carcinoma cells (HEp-2 cell line) was negligible, indicating the small side effect on human cells.326 The main limitation of this study was a lack of bacteria exposed to vancomycin alone as a positive control group. The successful observed results in Van/GNPs + laser-treated bacteria group may be attributed to the effect of vancomycin. The presence of vancomycin-resistant Enterococci among the investigated bacteria strains may diminish the effect of the lack of a positive control.
In an interesting study, Norman and colleagues developed anti-PA3 primary antibody-conjugated GNRs to selectively destroy the pathogenic antibiotic resistance Gram-negative bacterium, Pseudomonas aeruginosa. GNRs (68 nm × 18 nm) were synthesized with seed-mediated growth methods and antibody conjugation was designed with electrostatic interaction and covalent bonding. An electrostatic connection gained with the direct addition of antibody to as-prepared GNRs, while for covalent attachment two layers of polymers (PAA/PAH) (anionic poly(acrylic acid) [PAA] and cationic polyallylamine hydrochloride [PAH]) were further coated on GNRs using the layer-by-layer technique to cultivate amine terminal groups on modified GNRs in order to react with carboxylic acids of purified antibodies. The concentration of the antibody conjugated to GNRs and the efficacy of the bacteria target were the same in both methods, but greater stability was observed under physiological conditions when the antibody was attached to the GNRs with covalent bonding. Therefore, a covalently-attached antibody to GNRs was exposed to NIR light (785 nm; 50 mW; 10 min), resulting in a significant reduction in bacterial cell viability. The cell viability of the treated group (GNRs + cells + NIR) was below 20%, while the cell viability of the control groups (cells, cells + NIR, and cells + GNRs) was around 80%.327 The main limitation of this study was lack of bacteria exposed to cells + NIR + GNRs as a positive control group to allow the bacterial death of more than 80% to be assigned to effective targeting.
Recently, based on the National Antimicrobial Resistance Monitoring System, more than one-fifth of Salmonella strains were found to be resistant to at least five of the most extensively utilized antibiotics. Driven by this need, novel anti-Salmonella-antibody-conjugated oval-shaped GNPs were produced by seed-mediated growth in order to target antibiotic-resistant Salmonella. When antibody-conjugated GNPs were exposed to NIR irradiation (wavelength, 676 nm; light intensity, 40 mW; exposure time, 5–15 min), a Salmonella viability percentage of only 5% was reported, while 85% bacteria viability was observed for NIR radiation without GNPs. To show the active targeting of this therapeutic strategy, anti-Salmonella-antibody-conjugated GNRs were examined on E. coli bacteria and the results showed that most of the bacteria remained alive, even after 15 min of irradiation with 670 nm light. In contrast, 97% of Salmonella bacteria were killed after 15 min of irradiation. Interestingly, the effect of photothermal lysis became more dominant by the formation of microbial-clusters. For example, when the concentration of bacteria reached 104 cfu mL−1, the bacterial survival rate reached below 5% in comparison with 45% of bacterial viability at bacteria population of 500 mol L−1.328
Au/CuS core/shell NPs (25 nm) were designed by Addae and colleagues as a new type of transducer agent for PTT against B. anthracis (a life threatening bacterium) spores and cells. GNPs were synthesized using the seeded-growth method and then coated with CuS nanoshell. Cu+2 can enhance cell penetration of NPs through interaction with a negatively charged cell surface or ion/voltage-gated channels. The effect of Au/CuS NPs concentration (0.0083, 0.083, or 0.83 μM) and treatment time (0.5, 1, 3, 6, 12, or 24 h) on growth inhibition of B. anthracis spores and cells was investigated in order to obtain optimized bacteria death conditions. The results indicated cell membrane damage and a strong antimicrobial effect; even at a low concentration of NPs (0.83 μM) and short exposure time (0.5 h), the cell viability of the bacteria reached a 7-log reduction in bacteria population.168 It was found that Au/CuS NPs were extremely proficient in inactivating B. anthracis cells, but not efficient to the spores. The results were more informative if the GNPs and CuNPs were used as control groups.
Catheter-related infections (CRIs) are some of the most prevalent types of nosocomial infections.329–331 The surface modification of silicone (a widely used material for the fabrication of catheters) is one approach used to prevent pathogenic colonization on silicone catheters and, consequently, CRIs. Khantamat and colleagues applied GNShs for the NIR photothermal destruction of the drug-resistant Enterococcus faecalis (E. faecalis) pathogenic bacterium on the silicone surface. In order to cultivate GNShs on the silicone surface, first poly(amidoamine) dendrimer (PAMAM) was decorated on the silicone surface and then two different thiol-carboxylic acid dual functionalized components (16-mercaptohexadecanoic acid [16-MHDA] and D,L-α-lipoic acid) were connected to PAMAM and GNSHs via carboxylic acid and thiol functional groups, respectively. Both types of GNShs-decorated silicones along with a control sample (PAMAM-only coated silicone) were exposed to E. faecalis and then tested for a PTT effect. NIR illumination for 5 min showed that the surviving E. faecalis was substantially diminished when compared with the control sample. The results after 10 min of laser exposure were even more convincing, with almost 100% of bacteria having been killed. The PAMAM surface showed no tangible changes.332
Hu and colleges synthesized core–shell–shell Au–Ag–Au NRs and modified them with poly(sodium-p-styrenesulfonate) (PSS) to remove CTAB (a cytotoxic positively charged surfactant used in the synthesis procedure) and poly(allylamine hydrochloride) (PAH) to create a positive charge on the surface of NRs for better adherence to the E. coli. O157:H7 bacteria. The GNRs thus developed (60 × 18) were treated with E. coli and irradiated by NIR laser (785 nm/50 mW cm−2) for 0–60 min to investigate the PTT efficacy on bacterial killing. Au NRs and Au–Ag NRs were prepared and compared with core–shell–shell Au–Ag–Au NRs. After 20 min of irradiation, Au–Ag–Au NRs exhibited a surprisingly higher killing efficiency (two-times) than Au NRs, but the results were almost the same as Au–Ag NRs.333 Since Ag has an antibacterial performance and the bacteria killing rate of Au–Ag–Au and Au–Ag NRs were the same, the role of Ag seems to be important. Therefore, a control group consisting of Ag NPs would be necessary for a proper conclusion about the value of developing Au–Ag–Au NRs in PTT.
PEGylated reduced graphene oxide (PEG-rGO) has recently been introduced for efficient PTT, with high chemical and thermal stability. Turcheniuk and colleagues synthesized amine-terminated PEG-rGO and coupled it with carbocyclic-terminated PEG-GNRs (rGO-PEG-GNRs) for non-antibiotic-based treatments of Gram-negative uropathogenic E. coli UTI89. A standard proliferation assay revealed no toxic effect of rGO-PEG-GNRs on E. coli at concentrations up to 100 μg mL−1 without NIR radiation. The effect of laser irradiation (wavelength, 700 nm; laser power density of 8 W cm−2; exposure time, 10 min) showed temperature increases of up to 70, 50, and 30 °C for rGO-PEG-GNRs, GNRs, and rGO-PEG, respectively. This explains why the PTT effect on E. coli killing was more significant for rGO-PEG-GNRs than for rGO-PEG. Finally, rGO-PEG-GNRs were conjugated with heptyl α-D-mannoside (a bacterial surface presented glycan) for targeted killing of E. coli UTI89. The researchers demonstrated that rGO-PEG-GNRs are powerful photothermal agents for the effective killing (99% killing efficiency) of Gram-negative uropathogenic E. coli UTI89.334
It was hypothesized that the conjugation of GNRs and MNPs (GNR–MNPs) to fabricate recyclable antimicrobial agents may provide a fast, efficient, and reproducible route to the elimination of microbial and viral water contaminants. Ramasamy and coworkers synthesized GNR–MNPs and investigated their antibacterial activities against Gram-negative and Gram-positive strains of E. coli (KACC 10005) and E. faecalis (KACC 13807). NIR light with a wavelength of 671 nm, power densities of 10, 30, 60, 90 and 130 m W−2, and exposure time of 12 min was applied for photothermal studies. The bacteria killing rates were dramatically increased to 99% for E. coli and 95% for E. faecalis, while with simple laser exposed-bacteria (without NPs), no considerable effect on bacterial viability was observed.335 Further studies on bacteria PTT killing are summarized in Table 4.
| Particle type | Size | Laser radiation temperature | Significant remarks | Ref. |
|---|---|---|---|---|
| M3038 antibody-conjugated iron magnetic core–popcorn-shaped gold shell | 20 nm | 670 nm/1–2 W cm−2 10 min/48 °C | In vitro: multifunctional nanotechnology-driven approach was developed for targeted magnetic separation and enrichment, label-free SERS detection, and the selective photothermal destruction of MDR Salmonella DT104. The results indicated that MDR Salmonella bacteria percentage reached to 50% after 6 min laser exposure time while by increasing the laser exposure time to 9 min approximately up to 95% of bacteria died | 336 |
| Anti-protein A antibody conjugate GNRs | 15 × 50 nm | 825 nm/80 mW 6 min/45 °C | In vivo and in vitro GNRs conjugated with antibody treated group were significantly accumulated at infected muscle of mouse model and decreased the methicillin-resistant S. aureus (MRSA) bacteria level to 30% | 337 |
| Antibody-conjugated Au/Ag core–shell PEGylated GNRs | 10 × 40 nm | 480–850 nm 150 mW/10 min/44 °C | In vitro A new biomimetic coating strategy was designed for creating bimetallic Au/Ag nanorods (Au/Ag NRs) to kill bacteria through the combined effects of silver release and plasmonic heating. The results demonstrate antibody labeled GNRs + laser had higher cell damage in E. coli in comparison with S. epidermidis. This may be due to the rod-shape of E. coli compared with the spherical shape of S. epidermidis | 338 |
| GNRs-covered kanamycin-loaded hollow SiO2 nanocapsules | 100 nm | 785 nm/120 mW cm−2 20 min | In vitro: The results showed kanamycin, Au nanorods and hollow SiO2 nanocapsules cannot apply admissible fatality. But with a combination of them E. coli BL21 viability decreased to 50% | 339 |
| Highly fluorescent bovine serum albumin–gold nanoclusters conjugated human antistaphylococcal immunoglobulin and the Photosens photosynthesizer | 2 nm | 660 nm/300 mW cm−2 60 min | In vitro: They used Au nanoclusters for imaging and therapy. After incubation of bacteria with nanoclusters and laser treatment, CFU percent of S. aureus(MRSA) and E. coli was about 40, 25, 10% after 10, 15, 30 min laser irradiation, respectively | 340 |
| Gold nanoseeds bound to silica nanoeggs embedded with magnetic iron oxide NPs + vancomycin | 100 nm | 808 nm/250 mW cm−2/55 °C 3 min | In vitro: Survival fraction of all bacteria (A. baumannii, E. coli O157:H7, S. pyogenes, S. saprophyticus, E. faecalis, E. faecium) treated with Van-Fe3O4/Au without laser were about 50% toward the control group. But when the laser exposure was added to Van-Fe3O4/Au treated group, the survival fraction dropped to 0% | 341 |
| Iron/gold core–shell star-shaped nanoparticle conjugated with aptamer and MDRB Salmonella specific antibody | 70 nm | 670 nm/1–2 W cm−2 12 min | In vitro: Investigation of the effect of PTT and PDT of nanoparticles showing that PDT can reduce MDRB Salmonella viability to 75% and PTT to 40%. However, a combination provides an effective option, and dropped to 0% Salmonella viability (Fig. 17) | 342 |
| Staphylococcus aureus peptidoglycan specific antibody-conjugated GNPs | 40 nm | 532 nm/1 to 5 J cm−2 8 ns 100 pulse | In vitro: Comparison between functionalized GNP + laser and GNP + laser-treated groups show the first one can effectively apply cytotoxicity for S. aureus (MRSA and MSSA) with surviving population of 31% in the MSSA and 58% in the MRSA population | 343 |
| GNPs | 27 nm | 808 nm/2 W cm−2/10 min | In vitro: The evaluated bactericidal effect of nanoparticles on methicillin-resistant S. aureus (MRSA) live/dead cell with immuno-fluorescence microscopy. Photo-excitation of GNPs caused increased MRSA necrosis rates in comparison with MRSA groups received GNPs alone | 344 |
| Antibody-conjugated GNPs-SWCNTs nanohybrid | 20 nm | 670 nm/2 W cm−2 15 min | In vitro: Photothermal killing of bacteria treated with developed nanohybrid showed irreversible damage of more than 99% to Salmonella | 345 |
4. Conclusions and future perspectives
In summary, details of the PTT effect of GNPs on bacteria and cancer cells in the last 10 years have been discussed. It is considered that PTT might one day become an alternative treatment to replace traditional methods in the management of cancer and microbial infections. An overview of the literature shows the widespread research carried out on PTT all around the world. PTT has been conducted on quantum dots, GNPs, iron oxides, graphene oxides, and carbon nanotubes. GNPs attained an important place in studies conducted in the field of PTT due to its unique atomic, molecular, and plasmonic features. Factors that have been researched in studies of PTT include the size, morphology, and surface functionalization of GNPs; radiation intensity and wavelength of the emitted radiation; exposure duration; surface adsorption or cellular internalization; type of laser (continuous or pulsed); and direct or indirect radiation.As a result of the enormous evolution of photonic science and the unique features of GNPs in the optic and plasmonic field, it is predicted that photonics will play an exceptional role in future medicine and that GNPs will play a unique role in the field of diagnosis and therapy. Although the NIR investigated was in a range that is known to be harmless for tissues and cells of the body, further studies are needed to evaluate the extent of the energy to input to the cells. This is because, although the cellular genome will be unaffected, it is possible to affect the chemical bonds within the cell, as well as molecules inside the cell, cell-to-cell communication in the long-term and the causes of their collapse. Long-term safety is one of the most important concerns with respect to nanomaterials. Another challenge facing PTT is that the NIR-light beam used has little penetrating power on the tissues, meaning that PTT will not affect tumors in the deep tissue due to a lack of light penetration. Finally, we believe that development and investment in the field of PTT in the near future will be able to resolve many problems in terms of untreatable bacterial infections and cancerous diseases.
References
- T. Harper, Global funding of nanotechnologies & ITS Impact, Cientifica, july, 2011 Search PubMed.
- C.-M. J. Hu and L. Zhang, Curr. Drug Metab., 2009, 10, 836–841 CrossRef CAS PubMed.
- B. Al-Lazikani, U. Banerji and P. Workman, Nat. Biotechnol., 2012, 30, 679–692 CrossRef CAS PubMed.
- J. Song, H. Huang, Z. Xia, Y. Wei, N. Yao, L. Zhang, H. Yan, X. Jia and Z. Zhang, Integr. Cancer Ther., 2015, 3, 390–399 Search PubMed.
- A. Kapil, Indian J. Med. Res., 2005, 121, 83–91 Search PubMed.
- U. D. o. Health and H. Services, Centers for Disease Control and Prevention, Atlanta, GA, 2013, http://www.cdc.gov/drugresistance/threat-report-2013 Search PubMed.
- S. Rasouli, S. Davaran, F. Rasouli, M. Mahkam and R. Salehi, Des. Monomers Polym., 2014, 17, 227–237 CrossRef CAS.
- R. Salehi, H. Hamishehkar, M. Eskandani, M. Mahkam and S. Davaran, J. Drug Targeting, 2014, 22, 327–342 CrossRef CAS PubMed.
- S. Rasouli, S. Davaran, F. Rasouli, M. Mahkam and R. Salehi, Drug Delivery, 2014, 21, 155–163 CrossRef CAS PubMed.
- R. Salehi, E. Alizadeh, H. S. Kafil, A. M. Hassanzadeh and M. Mahkam, RSC Adv., 2015, 5, 105678–105691 RSC.
- R. Salehi, S. Rasouli and H. Hamishehkar, Int. J. Pharm., 2015, 487, 274–284 CrossRef CAS PubMed.
- R. Salehi, M. Irani, M. Eskandani, K. Nowruzi, S. Davaran and I. Haririan, Int. J. Polym. Mater. Polym. Biomater., 2014, 63, 609–619 CrossRef CAS.
- S. L. Hosseinipour, M. S. Khiabani, H. Hamishehkar and R. Salehi, J. Nanopart. Res., 2015, 17, 1–13 CrossRef CAS.
- L. C. Kennedy, L. R. Bickford, N. A. Lewinski, A. J. Coughlin, Y. Hu, E. S. Day, J. L. West and R. A. Drezek, Small, 2011, 7, 169–183 CrossRef CAS PubMed.
- P. K. Jain, X. Huang, I. H. El-Sayed and M. A. El-Sayed, Acc. Chem. Res., 2008, 41, 1578–1586 CrossRef CAS PubMed.
- D. P. O'Neal, L. R. Hirsch, N. J. Halas, J. D. Payne and J. L. West, Cancer Lett., 2004, 209, 171–176 CrossRef PubMed.
- R. Weissleder, Nat. Biotechnol., 2001, 19, 316–317 CrossRef CAS PubMed.
- A. M. Pekkanen, M. R. DeWitt and M. N. Rylander, J. Biomed. Nanotechnol., 2014, 10, 1677–1712 CrossRef CAS PubMed.
- H. Yuan, J. K. Register, H.-N. Wang, A. M. Fales, Y. Liu and T. Vo-Dinh, Anal. Bioanal. Chem., 2013, 405, 6165–6180 CrossRef CAS PubMed.
- H. Yuan, Y. Liu, A. M. Fales, Y. L. Li, J. Liu and T. Vo-Dinh, Anal. Chem., 2012, 85, 208–212 CrossRef PubMed.
- Y. Bayazitoglu, S. Kheradmand and T. K. Tullius, Int. J. Heat Mass Transfer, 2013, 67, 469–486 CrossRef CAS.
- H. Yuan, C. M. Wilson, J. Xia, S. L. Doyle, S. Li, A. M. Fales, Y. Liu, E. Ozaki, K. Mulfaul and G. Hanna, Nanoscale, 2014, 6, 4078–4082 RSC.
- D. Kumar, N. Saini, N. Jain, R. Sareen and V. Pandit, Expert Opin. Drug Delivery, 2013, 10, 397–409 CrossRef CAS PubMed.
- J. Xie, S. Lee and X. Chen, Adv. Drug Delivery Rev., 2010, 62, 1064–1079 CrossRef CAS PubMed.
- I. N. Biosciences, ClinicalTrials. gov., National Library of Medicine, Bethesda, MD, US, 2000 Search PubMed.
- S. C. Gad, K. L. Sharp, C. Montgomery, J. D. Payne and G. P. Goodrich, Int. J. Toxicol., 2012, 31, 584–594 CrossRef CAS PubMed.
- K. S. Merza, H. D. Al-Attabi, Z. M. Abbas and H. A. Yusr, Green Sustainable Chem., 2012, 2, 26 CrossRef CAS.
- M. B. Mohamed, Z. L. Wang and M. A. El-Sayed, J. Phys. Chem. A, 1999, 103, 10255–10259 CrossRef CAS.
- Z. Shervani and Y. Yamamoto, Mater. Lett., 2011, 65, 92–95 CrossRef CAS.
- P. Abdulkin, T. L. Precht, B. R. Knappett, H. E. Skelton, D. A. Jefferson and A. E. Wheatley, Part. Part. Syst. Charact., 2014, 31, 571–579 CrossRef CAS.
- J. K. Young, N. A. Lewinski, R. J. Langsner, L. C. Kennedy, A. Satyanarayan, V. Nammalvar, A. Y. Lin and R. A. Drezek, Nanoscale Res. Lett., 2011, 6, 1–11 CrossRef PubMed.
- J. Newman and G. Blanchard, Langmuir, 2006, 22, 5882–5887 CrossRef CAS PubMed.
- P. Nalawade, T. Mukherjee and S. Kapoor, Adv. Nanopart., 2013, 2, 78–86 CrossRef.
- C. J. Ward, R. Tronndorf, A. S. Eustes, M. L. Auad and E. W. Davis, J. Nanomater., 2014, 2014, 47 Search PubMed.
- S. Koeppl, N. Ghielmetti, W. Caseri and R. Spolenak, J. Nanopart. Res., 2013, 15, 1–11 CrossRef.
- L. Scarabelli, M. Grzelczak and L. M. Liz-Marzán, Chem. Mater., 2013, 25, 4232–4238 CrossRef CAS.
- R. Sardar, A. M. Funston, P. Mulvaney and R. W. Murray, Langmuir, 2009, 25, 13840–13851 CrossRef CAS PubMed.
- B. Lkhagvadulam, J. H. Kim, I. Yoon and Y. K. Shim, BioMed Res. Int., 2012, 2013, 720579 Search PubMed.
- Y. Cheng, A. C. Samia, J. D. Meyers, I. Panagopoulos, B. Fei and C. Burda, J. Am. Chem. Soc., 2008, 130, 10643–10647 CrossRef CAS PubMed.
- J. D. Meyers, Y. Cheng, A. M. Broome, R. S. Agnes, M. D. Schluchter, S. Margevicius, X. Wang, M. E. Kenney, C. Burda and J. P. Basilion, Part. Part. Syst. Charact., 2015, 32, 448–457 CrossRef CAS PubMed.
- V. P. Pattani and J. W. Tunnell, Lasers Surg. Med., 2012, 44, 675–684 CrossRef PubMed.
- S. Alex and A. Tiwari, J. Nanosci. Nanotechnol., 2015, 15, 1869–1894 CrossRef CAS PubMed.
- A. Khan, R. Rashid, G. Murtaza and A. Zahra, Trop. J. Pharm. Res., 2014, 13, 1169–1177 CrossRef CAS.
- L. Bac, J. Kim and J. Kim, Rev. Adv. Mater. Sci., 2011, 28, 117–121 CAS.
- C. Li, D. Li, G. Wan, J. Xu and W. Hou, Nanoscale Res. Lett., 2011, 6, 1–10 Search PubMed.
- N. N. Long, C. D. Kiem, S. C. Doanh, C. T. Nguyet, P. T. Hang, N. D. Thien and L. M. Quynh, J. Phys.: Conf. Ser., 2009, 187 CrossRef CAS.
- H. N. Verma, P. Singh and R. Chavan, Vet. World, 2014, 7, 72–77 CrossRef CAS.
- A. Tabrizi, F. Ayhan and H. Ayhan, Hacettepe Journal of Biology and Chemistry, 2009, 37, 217–226 Search PubMed.
- N. Hanžić, T. Jurkin, A. Maksimović and M. Gotić, Radiat. Phys. Chem., 2015, 106, 77–82 CrossRef.
- J. r. Polte, T. T. Ahner, F. Delissen, S. Sokolov, F. Emmerling, A. F. Thünemann and R. Kraehnert, J. Am. Chem. Soc., 2010, 132, 1296–1301 CrossRef CAS PubMed.
- I. Ojea-Jiménez and J. M. Campanera, J. Phys. Chem. C, 2012, 116, 23682–23691 Search PubMed.
- I. Ojea-Jiménez, F. M. Romero, N. G. Bastús and V. Puntes, J. Phys. Chem. C, 2010, 114, 1800–1804 Search PubMed.
- P. Sahoo and P. Singh, Vet. World, 2014, 7, 1010–1013 CrossRef.
- A. R. Prado, J. P. Oliveira, W. J. Keijok, B. A. Milaneze, B. V. Nogueira, M. C. Guimarães, M. J. Pontes and M. R. Ribeiro, BMC Proc., 2014, 8, 252 CrossRef.
- M. N. Martin, D. Li, A. Dass and S.-K. Eah, Nanoscale, 2012, 4, 4091–4094 RSC.
- M. Brust, M. Walker, D. Bethell, D. J. Schiffrin and R. Whyman, J. Chem. Soc., Chem. Commun., 1994, 801–802 RSC.
- C. Deraedt, L. Salmon, S. Gatard, R. Ciganda, R. Hernandez, J. Ruiz and D. Astruc, Chem. Commun., 2014, 50, 14194–14196 RSC.
- M. Chen, H. Kang, Y. Gong, J. Guo, H. Zhang and R. Liu, ACS Appl. Mater. Interfaces, 2015, 7, 21717–21726 CAS.
- A. K. Samal, T. S. Sreeprasad and T. Pradeep, J. Nanopart. Res., 2010, 12, 1777–1786 CrossRef CAS.
- N. R. Jana, L. Gearheart and C. J. Murphy, J. Phys. Chem. B, 2001, 105, 4065–4067 CrossRef CAS.
- A. Sánchez-Iglesias, J. Barroso, D. M. Solís, J. M. Taboada, F. Obelleiro, V. Pavlov, A. Chuvilin and M. Grzelczak, J. Mater. Chem. A, 2016, 4, 7045–7052 Search PubMed.
- Z. Kereselidze, V. H. Romero, X. G. Peralta and F. Santamaria, J. Visualized Exp., 2012, e3570 Search PubMed.
- S. K. Mandal, IOSR J. Appl. Chem., 2013, 3, 68–73 CrossRef.
- T. K. Sau, A. Pal, N. Jana, Z. Wang and T. Pal, J. Nanopart. Res., 2001, 3, 257–261 CrossRef CAS.
- Y. Zhou, C. Wang, Y. Zhu and Z. Chen, Chem. Mater., 1999, 11, 2310–2312 CrossRef CAS.
- A. Plech, V. Kotaidis, A. Siems and M. Sztucki, Phys. Chem. Chem. Phys., 2008, 10, 3888–3894 RSC.
- T. K. Sau and C. J. Murphy, Langmuir, 2004, 20, 6414–6420 CrossRef CAS PubMed.
- N. D. Burrows, W. Lin, J. G. Hinman, J. M. Dennison, A. M. Vartanian, N. S. Abadeer, E. M. Grzincic, L. M. Jacob, J. Li and C. J. Murphy, Langmuir, 2016, 32, 9905–9921 CrossRef CAS PubMed.
- A. Gole and C. J. Murphy, Chem. Mater., 2004, 16, 3633–3640 CrossRef CAS.
- K. R. Brown and M. J. Natan, Langmuir, 1998, 14, 726–728 CrossRef CAS.
- M.-C. Daniel and D. Astruc, Chem. Rev., 2004, 104, 293–346 CrossRef CAS PubMed.
- P. C. Chen, S. C. Mwakwari and A. K. Oyelere, Nanotechnol., Sci. Appl., 2008, 1, 45 CrossRef CAS.
- F. Scaletti, C. S. Kim, L. Messori and V. M. Rotello, MethodsX, 2014, 1, 118–123 CrossRef PubMed.
- J. Cao, T. Sun and K. T. Grattan, Sens. Actuators, B, 2014, 195, 332–351 CrossRef CAS.
- T. Thai, Y. Zheng, S. Ng, H. Ohshima, M. Altissimo and U. Bach, Nanoscale, 2014, 6, 6515–6520 RSC.
- Y. Li, J. Ma and Z. Ma, Electrochim. Acta, 2013, 108, 435–440 CrossRef CAS.
- H.-L. Wu, C.-H. Chen and M. H. Huang, Chem. Mater., 2008, 21, 110–114 CrossRef.
- Y. Zhang, F. Xu, Y. Sun, C. Guo, K. Cui, Y. Shi, Z. Wen and Z. Li, Chem.–Eur. J., 2010, 16, 9248–9256 CrossRef CAS PubMed.
- Z. Wei and H. Matsui, Nat. Commun., 2014, 5, 3870 CAS.
- D. Zhang, C. Zhang, Y. Lu, Y. LIU and Y. Hao, Progr. Chem., 2015, 27, 1057–1064 Search PubMed.
- C.-C. Huang, Z. Yang and H.-T. Chang, Langmuir, 2004, 20, 6089–6092 CrossRef CAS PubMed.
- Y. Gao, J. Gu, L. Li, W. Zhao and Y. Li, Langmuir, 2016, 32, 2251–2258 CrossRef CAS PubMed.
- H. Cui, W. Wang, C. F. Duan, Y. P. Dong and J. Z. Guo, Chem.–Eur. J., 2007, 13, 6975–6984 CrossRef CAS PubMed.
- W. Wang, T. Xiong and H. Cui, Langmuir, 2008, 24, 2826–2833 CrossRef CAS PubMed.
- D. Wei, W. Sun, W. Qian, Y. Ye and X. Ma, Carbohydr. Res., 2009, 344, 2375–2382 CrossRef CAS PubMed.
- D. R. Bhumkar, H. M. Joshi, M. Sastry and V. B. Pokharkar, Pharm. Res., 2007, 24, 1415–1426 CrossRef CAS PubMed.
- W. Wang and H. Cui, J. Phys. Chem. C, 2008, 112, 10759–10766 CAS.
- Z. Wang, J. Zhang, J. M. Ekman, P. J. Kenis and Y. Lu, Nano Lett., 2010, 10, 1886–1891 CrossRef CAS PubMed.
- L. Li and J. Weng, Nanotechnology, 2010, 21, 305603 CrossRef PubMed.
- L. Zhao, X. Ji, X. Sun, J. Li, W. Yang and X. Peng, J. Phys. Chem. C, 2009, 113, 16645–16651 CAS.
- W. Wang, X. Yang and H. Cui, J. Phys. Chem. C, 2008, 112, 16348–16353 CAS.
- N. Elizondo, A. Alcorta, E. Torres, F. Hernández, F. Paraguay, J. Arriaga, P. Segovia, R. Obregón, S. Belmares and V. Coello, Green Chemistry - Environmentally Benign Approaches, INTECH Open Access Publisher, 2012, pp. 139–156 Search PubMed.
- V. Makarov, A. Love, O. Sinitsyna, S. Makarova, I. Yaminsky, M. Taliansky and N. Kalinina, Acta Naturae, 2014, 6, 35–44 CAS.
- P. Elia, R. Zach, S. Hazan, S. Kolusheva, Z. e. Porat and Y. Zeiri, Int. J. Nanomed., 2014, 9, 4007 Search PubMed.
- Y. Li, T.-Y. Wu, S.-M. Chen, M. A. Ali and F. M. AlHemaid, Int. J. Electrochem. Sci., 2012, 7, 12742–12751 CAS.
- V. Vadlapudi and D. Kaladhar, Middle East J. Sci. Res., 2014, 19, 834–842 Search PubMed.
- M. Banoee, N. Mokhtari, A. A. Sepahi, P. J. Fesharaki, H. Monsef-Esfahani, Z. Ehsanfar, M. Khoshayand and A. Shahverdi, Iran. J. Mater. Sci. Eng., 2010, 7, 48–53 CAS.
- P. Alexandridis, Chem. Eng. Technol., 2011, 34, 15–28 CrossRef CAS.
- S. Mukherjee, S. Sau, D. Madhuri, V. S. Bollu, K. Madhusudana, B. Sreedhar, R. Banerjee and C. R. Patra, J. Biomed. Nanotechnol., 2016, 12, 165–181 CrossRef CAS PubMed.
- T. Suman, S. R. Rajasree, R. Ramkumar, C. Rajthilak and P. Perumal, Spectrochim. Acta, Part A, 2014, 118, 11–16 CrossRef CAS PubMed.
- R. Fierascu, R. Ion and I. Dumitriu, Rapid. Comm. Mass Spectrom., 2010, 4, 1297–1300 CAS.
- N. Basavegowda, A. Sobczak-Kupiec, R. I. Fenn and S. Dinakar, IET Micro & Nano Letters, 2013, 8, 400–404 CAS.
- C. G. Kumar, Y. Poornachandra and C. Chandrasekhar, Nanoscale, 2015, 7, 18738–18750 RSC.
- C. Malarkodi, S. Rajeshkumar, M. Vanaja, K. Paulkumar, G. Gnanajobitha and G. Annadurai, J. Nanostruct. Chem., 2013, 3, 1–7 Search PubMed.
- P. Manivasagan and J. Oh, Mar. Drugs, 2015, 13, 6818–6837 CrossRef CAS PubMed.
- L. Du, H. Jiang, X. Liu and E. Wang, Electrochem. Commun., 2007, 9, 1165–1170 CrossRef CAS.
- D. N. Correa-Llantén, S. A. Muñoz-Ibacache, M. E. Castro, P. A. Muñoz and J. M. Blamey, Microb. Cell Fact., 2013, 12, 1–6 CrossRef PubMed.
- U. Shedbalkar, R. Singh, S. Wadhwani, S. Gaidhani and B. Chopade, Adv. Colloid Interface Sci., 2014, 209, 40–48 CrossRef CAS PubMed.
- T. Beveridge and R. Murray, J. Bacteriol., 1976, 127, 1502–1518 CAS.
- C. Graf and A. van Blaaderen, Langmuir, 2002, 18, 524–534 CrossRef CAS.
- Z.-Y. Lin, J.-M. Wu, B.-Q. Fu, R. Xue, J.-Z. Zhou, Q.-X. Zheng, Y.-Y. Liu and J.-K. Fu, Acta Chim. Sin., 2004, 62, 1829–1834 CAS.
- C. Radloff, R. A. Vaia, J. Brunton, G. T. Bouwer and V. K. Ward, Nano Lett., 2005, 5, 1187–1191 CrossRef CAS PubMed.
- X. Huang, P. K. Jain, I. H. El-Sayed and M. A. El-Sayed, Nanomedicine, 2007, 2, 681–693 CrossRef CAS PubMed.
- C. L. Nehl, H. Liao and J. H. Hafner, Nano Lett., 2006, 6, 683–688 CrossRef CAS PubMed.
- S. Link and M. A. El-Sayed, Int. Rev. Phys. Chem., 2000, 19, 409–453 CrossRef CAS.
- T. El-Brolossy, T. Abdallah, M. B. Mohamed, S. Abdallah, K. Easawi, S. Negm and H. Talaat, Eur. Phys. J.: Spec. Top., 2008, 153, 361–364 CrossRef.
- X. Huang and M. A. El-Sayed, J. Adv. Res., 2010, 1, 13–28 CrossRef.
- W. Rechberger, A. Hohenau, A. Leitner, J. Krenn, B. Lamprecht and F. Aussenegg, Opt. Commun., 2003, 220, 137–141 CrossRef CAS.
- D. Ghosh and N. Chattopadhyay, Opt. Photonics J., 2013, 3, 18–26 CrossRef CAS.
- B. Dubertret, M. Calame and A. J. Libchaber, Nat. Biotechnol., 2001, 19, 365–370 CrossRef CAS PubMed.
- M. Swierczewska, S. Lee and X. Chen, Phys. Chem. Chem. Phys., 2011, 13, 9929–9941 RSC.
- C. H. Chen, Y.-J. Wu and J.-J. Chen, BioMed Res. Int., 2015, 2015 Search PubMed.
- L. Tong, Q. Wei, A. Wei and J. X. Cheng, Photochem. Photobiol., 2009, 85, 21–32 CrossRef CAS PubMed.
- M. Alsawafta, M. Wahbeh and V.-V. Truong, J. Nanomater., 2012, 2012, 33 Search PubMed.
- S. Mubeen, S. Zhang, N. Kim, S. Lee, S. Krämer, H. Xu and M. Moskovits, Nano Lett., 2012, 12, 2088–2094 CrossRef CAS PubMed.
- H. Chen, J. Lee, N. L. Kang, K. Koh and J. Lee, Microchim. Acta, 2011, 172, 489–494 CrossRef CAS.
- P. K. Jain, K. S. Lee, I. H. El-Sayed and M. A. El-Sayed, J. Phys. Chem. B, 2006, 110, 7238–7248 CrossRef CAS PubMed.
- I. H. El-Sayed, X. Huang and M. A. El-Sayed, Nano Lett., 2005, 5, 829–834 CrossRef CAS PubMed.
- J. Kim, Y. Piao and T. Hyeon, Chem. Soc. Rev., 2009, 38, 372–390 RSC.
- N. Kytai Truong, J. Bioeng. Biomed. Sci., 2012, 2, e112 Search PubMed.
- D. Jaque, L. M. Maestro, B. Del Rosal, P. Haro-Gonzalez, A. Benayas, J. Plaza, E. M. Rodríguez and J. G. Solé, Nanoscale, 2014, 6, 9494–9530 RSC.
- F. Zhang, J. Cao, X. Chen, K. Yang, L. Zhu, G. Fu, X. Huang and X. Chen, Evaluation, 2015, 5, 1445 Search PubMed.
- P. P. Joshi, Y.-S. Chen, S. Kim, J. Shah, K. Sokolov and S. Emelianov, Annual International Conference of the IEEE Engineering in Medicine and Biology Society, 2009, pp. 4106–4109 Search PubMed.
- W. I. Choi, A. Sahu, Y. H. Kim and G. Tae, Ann. Biomed. Eng., 2012, 40, 534–546 CrossRef PubMed.
- V. P. Zharov, J.-W. Kim, D. T. Curiel and M. Everts, Nanomedicine: Nanotechnology, Biology and Medicine, 2005, 1, 326–345 CrossRef CAS PubMed.
- F. Chen and W. Cai, Nanomedicine, 2015, 10, 1 CrossRef CAS PubMed.
- J. P. Leung, S. Wu, K. C. Chou and R. Signorell, Nanomaterials, 2013, 3, 86–106 CrossRef CAS.
- L. Cheng, C. Wang, L. Feng, K. Yang and Z. Liu, Chem. Rev., 2014, 114, 10869–10939 CrossRef CAS PubMed.
- J. Ren, S. Shen, D. Wang, Z. Xi, L. Guo, Z. Pang, Y. Qian, X. Sun and X. Jiang, Biomaterials, 2012, 33, 3324–3333 CrossRef CAS PubMed.
- N. Levi-Polyachenko, C. Young, C. MacNeill, A. Braden, L. Argenta and S. Reid, Int. J. Hyperthermia, 2014, 30, 490–501 CrossRef CAS PubMed.
- X. Song, Q. Chen and Z. Liu, Nano Res., 8, 340–354 CrossRef CAS.
- E. G. Graham, C. M. Macneill and N. H. Levi-Polyachenko, Nano LIFE, 2013, 3, 1330002 CrossRef.
- G. Z. Jia, W. K. Lou, F. Cheng, X. L. Wang, J. H. Yao, N. Dai, H. Q. Lin and K. Chang, Nano Res., 2014, 1–11 Search PubMed.
- L. Nair, Y. Nagaoka, T. Maekawa, D. Sakthikumar and R. Jayasree, Small, 2014, 10, 2771–2775 CrossRef CAS PubMed.
- N. Huang, H. Wang, J. Zhao, H. Lui, M. Korbelik and H. Zeng, Lasers Surg. Med., 2010, 42, 798–808 CrossRef PubMed.
- F. Zhou, D. Xing, Z. Ou, B. Wu, D. E. Resasco and W. R. Chen, J. Biomed. Opt., 2009, 14, 021009 CrossRef PubMed.
- R. Martínez-Zaguilán and J. Qiu, New J. Chem., 2015, 39, 5743–5749 RSC.
- V. Kotaidis and A. Plech, Appl. Phys. Lett., 2005, 87, 213102 CrossRef.
- J.-L. Li and M. Gu, IEEE J. Sel. Top. Quantum Electron., 2010, 16, 989–996 CrossRef.
- B. Cong, C. Kan, H. Wang, J. Liu, H. Xu and S. Ke, J. Mater. Sci. Chem. Eng., 2014, 2, 20 CAS.
- R. Mooney, E. Schena, A. Zhumkhawala, K. Aboody and J. Berlin, Conf Proc IEEE Eng Med Biol Soc, 2015, 2563 Search PubMed.
- X. Ding, C. H. Liow, M. Zhang, R. Huang, C. Li, H. Shen, M. Liu, Y. Zou, N. Gao and Z. Zhang, J. Am. Chem. Soc., 2014, 136, 15684–15693 CrossRef CAS PubMed.
- M.-F. Tsai, S.-H. G. Chang, F.-Y. Cheng, V. Shanmugam, Y.-S. Cheng, C.-H. Su and C.-S. Yeh, ACS Nano, 2013, 7, 5330–5342 CrossRef CAS PubMed.
- L. Li, Y. Liu, P. Hao, Z. Wang, L. Fu, Z. Ma and J. Zhou, Biomaterials, 2015, 41, 132–140 CrossRef CAS PubMed.
- M. W. Knight and N. J. Halas, New J. Phys., 2008, 10, 105006 CrossRef.
- J. Shah, S. R. Aglyamov, K. Sokolov, T. E. Milner and S. Y. Emelianov, Opt. Express, 2008, 16, 3776–3785 CrossRef CAS PubMed.
- D. Pissuwan, C. H. Cortie, S. M. Valenzuela and M. B. Cortie, Trends Biotechnol., 2010, 28, 207–213 CrossRef CAS PubMed.
- O. S. Muddineti, B. Ghosh and S. Biswas, Int. J. Pharm., 2015, 484, 252–267 CrossRef CAS PubMed.
- B. Van de Broek, N. Devoogdt, A. D'Hollander, H.-L. Gijs, K. Jans, L. Lagae, S. Muyldermans, G. Maes and G. Borghs, ACS Nano, 2011, 5, 4319–4328 CrossRef CAS PubMed.
- P. C. Ray, S. A. Khan, A. K. Singh, D. Senapati and Z. Fan, Chem. Soc. Rev., 2012, 41, 3193–3209 RSC.
- H. Wang, R. Yang, L. Yang and W. Tan, ACS Nano, 2009, 3, 2451–2460 CrossRef CAS PubMed.
- Y. Matsushita-Ishiodori and T. Ohtsuki, Acc. Chem. Res., 2012, 45, 1039–1047 CrossRef CAS PubMed.
- J. He, Y. Liu, T. Babu, Z. Wei and Z. Nie, J. Am. Chem. Soc., 2012, 134, 11342–11345 CrossRef CAS PubMed.
- H.-Z. Lai, W.-Y. Chen, C.-Y. Wu and Y.-C. Chen, ACS Appl. Mater. Interfaces, 2015, 7, 2046–2054 CAS.
- K. P. Miller, L. Wang, B. C. Benicewicz and A. W. Decho, Chem. Soc. Rev., 2015, 44, 7787–7807 RSC.
- M. Yin, Z. Li, E. Ju, Z. Wang, K. Dong, J. Ren and X. Qu, Chem. Commun., 2014, 50, 10488–10490 RSC.
- W.-L. Chiang, T.-T. Lin, R. Sureshbabu, W.-T. Chia, H.-C. Hsiao, H.-Y. Liu, C.-M. Yang and H.-W. Sung, J. Controlled Release, 2015, 199, 53–62 CrossRef CAS PubMed.
- E. Addae, X. Dong, E. McCoy, C. Yang, W. Chen and L. Yang, J. Biol. Eng., 2014, 8, 1–11 CrossRef PubMed.
- M. K. Popp, I. Oubou, C. Shepherd, Z. Nager, C. Anderson and L. Pagliaro, J. Nanomater., 2014, 2014 Search PubMed.
- T. Curry, R. Kopelman, M. Shilo and R. Popovtzer, Contrast Media Mol. Imaging, 2014, 9, 53–61 CrossRef CAS PubMed.
- Y. Jin, Adv. Mater., 2012, 24, 5153–5165 CrossRef CAS PubMed.
- F. Lu, T. L. Doane, J.-J. Zhu and C. Burda, Inorg. Chim. Acta, 2012, 393, 142–153 CrossRef CAS.
- A. M. Alkilany, L. B. Thompson, S. P. Boulos, P. N. Sisco and C. J. Murphy, Adv. Drug Delivery Rev., 2012, 64, 190–199 CrossRef CAS PubMed.
- C.-B. Kim, D. K. Yi, P. S. S. Kim, W. Lee and M. J. Kim, J. Nanosci. Nanotechnol., 2009, 9, 2841–2845 CrossRef CAS PubMed.
- M. L. Cohen, Science, 1992, 257, 1050–1055 CAS.
- A. Newaj-Fyzul, A. Mutani, A. Ramsubhag and A. Adesiyun, Zoonoses Public Health, 2008, 55, 206–213 CrossRef CAS PubMed.
- A. Bartoloni, L. Pallecchi, M. Benedetti, C. Fernandez, Y. Vallejos, E. Guzman, A. L. Villagran, A. Mantella, C. Lucchetti and F. Bartalesi, Emerging Infect. Dis., 2006, 12, 907–913 CrossRef PubMed.
- J. Tanwar, S. Das, Z. Fatima and S. Hameed, Interdiscip. Perspect. Infect. Dis., 2014, 2014 Search PubMed.
- U. Gopinathan, S. Sharma, P. Garg and G. N. Rao, Indian J. Ophthalmol., 2009, 57, 273 Search PubMed.
- S. Mansouri and S. Abbasi, Iran. J. Med. Sci., 2015, 35, 101–108 Search PubMed.
- W. Jia, G. Li and W. Wang, Int. J. Environ. Res. Public Health, 2014, 11, 3424–3442 CrossRef PubMed.
- S. S. Andrade, R. N. Jones, A. C. Gales and H. S. Sader, J. Antimicrob. Chemother., 2003, 52, 140–141 CrossRef CAS PubMed.
- A. P. Magiorakos, A. Srinivasan, R. Carey, Y. Carmeli, M. Falagas, C. Giske, S. Harbarth, J. Hindler, G. Kahlmeter and B. Olsson-Liljequist, Clin. Microbiol. Infect., 2012, 18, 268–281 CrossRef CAS PubMed.
- S. Nseir, C. Di Pompeo, B. Cavestri, E. Jozefowicz, M. Nyunga, S. Soubrier, M. Roussel-Delvallez, F. Saulnier, D. Mathieu and A. Durocher, Crit. Care Med., 2006, 34, 2959–2966 CrossRef CAS PubMed.
- E. Fröhlich, Int. J. Nanomed., 2012, 7, 5577 CrossRef PubMed.
- F. Lu, S. H. Wu, Y. Hung and C. Y. Mou, Small, 2009, 5, 1408–1413 CrossRef CAS PubMed.
- A. M. Alkilany and C. J. Murphy, J. Nanopart. Res., 2010, 12, 2313–2333 CrossRef CAS PubMed.
- P. Wang, X. Wang, L. Wang, X. Hou, W. Liu and C. Chen, Sci. Technol. Adv. Mater., 2015, 16, 034610 CrossRef.
- K. Niikura, T. Matsunaga, T. Suzuki, S. Kobayashi, H. Yamaguchi, Y. Orba, A. Kawaguchi, H. Hasegawa, K. Kajino and T. Ninomiya, ACS Nano, 2013, 7, 3926–3938 CrossRef CAS PubMed.
- L. Shang, K. Nienhaus and G. U. Nienhaus, J. Nanobiotechnol., 2014, 12, b67 CrossRef PubMed.
- P. Nativo, I. A. Prior and M. Brust, ACS Nano, 2008, 2, 1639–1644 CrossRef CAS PubMed.
- M. Neshatian, S. Chung, D. Yohan, C. Yang and D. B. Chithrani, Colloid and Interface Science Communications, 2014, 1, 57–61 CrossRef CAS.
- J. D. Trono, K. Mizuno, N. Yusa, T. Matsukawa, K. Yokoyama and M. Uesaka, J. Radiat. Res., 2011, 52, 103–109 CrossRef PubMed.
- P. Jurney, R. Agarwal, K. Roy, S. Sreenivasan and L. Shi, J. Nanotechnol. Eng. Med., 2015, 6, 011007 CrossRef.
- R. K. Kannadorai and Q. Liu, Med. Phys., 2013, 40, 103301 CrossRef PubMed.
- I. L. Maksimova, G. G. Akchurin, B. N. Khlebtsov, G. S. Terentyuk, G. G. Akchurin, I. A. Ermolaev, A. A. Skaptsov, E. P. Soboleva, N. G. Khlebtsov and V. V. Tuchin, Med. Laser Appl., 2007, 22, 199–206 CrossRef.
- E. Moros, Physics of thermal therapy: fundamentals and clinical applications, CRC Press, 2012 Search PubMed.
- M. Etrati Khosroshahi, L. Ghazanfari and Z. Hasan-Nejad, Iranian Journal of Medical Physics, 2013, 9, 253–263 Search PubMed.
- Y. Hong, E. Lee, J. Choi, S. J. Oh, S. Haam, Y.-M. Huh, D. S. Yoon, J.-S. Suh and J. Yang, J. Nanomater., 2012, 2012, 2 Search PubMed.
- A. Sarker, Monitoring temperature distribution during laser-tissue interaction for cancer treatment using magnetic resonance thermometry, University of Central Oklahoma, 2009 Search PubMed.
- J. R. Navarro, D. Manchon, F. Lerouge, N. P. Blanchard, S. Marotte, Y. Leverrier, J. Marvel, F. Chaput, G. Micouin and A.-M. Gabudean, Nanotechnology, 2012, 23, 465602 CrossRef PubMed.
- X. Huang, I. H. El-Sayed, W. Qian and M. A. El-Sayed, J. Am. Chem. Soc., 2006, 128, 2115–2120 CrossRef CAS PubMed.
- L. Gao, J. Fei, J. Zhao, H. Li, Y. Cui and J. Li, ACS Nano, 2012, 6, 8030–8040 CrossRef CAS PubMed.
- J. Chen, M. Yang, Q. Zhang, E. C. Cho, C. M. Cobley, C. Kim, C. Glaus, L. V. Wang, M. J. Welch and Y. Xia, Adv. Funct. Mater., 2010, 20, 3684–3694 CrossRef CAS.
- H. Liu, D. Chen, F. Tang, G. Du, L. Li, X. Meng, W. Liang, Y. Zhang, X. Teng and Y. Li, Nanotechnology, 2008, 19, 455101 CrossRef PubMed.
- Y. Ma, X. Liang, S. Tong, G. Bao, Q. Ren and Z. Dai, Adv. Funct. Mater., 2013, 23, 815–822 CrossRef CAS.
- H. Liu, T. Liu, X. Wu, L. Li, L. Tan, D. Chen and F. Tang, Adv. Mater., 2012, 24, 755–761 CrossRef CAS PubMed.
- L. R. Hirsch, A. M. Gobin, A. R. Lowery, F. Tam, R. A. Drezek, N. J. Halas and J. L. West, Ann. Biomed. Eng., 2006, 34, 15–22 CrossRef PubMed.
- V. P. Pattani, J. Shah, A. Atalis, A. Sharma and J. W. Tunnell, J. Nanopart. Res., 2015, 17, 1–11 CrossRef CAS.
- T. Okuno, S. Kato, Y. Hatakeyama, J. Okajima, S. Maruyama, M. Sakamoto, S. Mori and T. Kodama, J. Controlled Release, 2013, 172, 879–884 CrossRef CAS PubMed.
- M. A. Mackey, M. R. Ali, L. A. Austin, R. D. Near and M. A. El-Sayed, J. Phys. Chem. B, 2014, 118, 1319–1326 CrossRef CAS PubMed.
- E. B. Dickerson, E. C. Dreaden, X. Huang, I. H. El-Sayed, H. Chu, S. Pushpanketh, J. F. McDonald and M. A. El-Sayed, Cancer Lett., 2008, 269, 57–66 CrossRef CAS PubMed.
- H.-W. Yang, H.-L. Liu, M.-L. Li, I.-W. Hsi, C.-T. Fan, C.-Y. Huang, Y.-J. Lu, M.-Y. Hua, H.-Y. Chou and J.-W. Liaw, Biomaterials, 2013, 34, 5651–5660 CrossRef CAS PubMed.
- N. Martin and M. Modi, Clin. Pharmacokinet., 2001, 40, 539–551 CrossRef PubMed.
- P. Bailon and C.-Y. Won, Expert Opin. Drug Delivery, 2009, 6, 1–16 CrossRef CAS PubMed.
- G. F. Paciotti, L. Myer, D. Weinreich, D. Goia, N. Pavel, R. E. McLaughlin and L. Tamarkin, Drug Delivery, 2004, 11, 169–183 CrossRef CAS PubMed.
- G. Kong, R. D. Braun and M. W. Dewhirst, Cancer Res., 2000, 60, 4440–4445 CAS.
- G. Kong, R. D. Braun and M. W. Dewhirst, Cancer Res., 2001, 61, 3027–3032 CAS.
- A. J. Gormley, K. Greish, A. Ray, R. Robinson, J. A. Gustafson and H. Ghandehari, Int. J. Pharm., 2011, 415, 315–318 CrossRef CAS PubMed.
- A. J. Gormley, N. Larson, S. Sadekar, R. Robinson, A. Ray and H. Ghandehari, Nano Today, 2012, 7, 158–167 CrossRef CAS PubMed.
- W. I. Choi, J.-Y. Kim, C. Kang, C. C. Byeon, Y. H. Kim and G. Tae, ACS Nano, 2011, 5, 1995–2003 CrossRef CAS PubMed.
- Y.-C. Chuang, C.-J. Lin, S.-F. Lo, J.-L. Wang, S.-C. Tzou, S.-S. Yuan and Y.-M. Wang, Biomaterials, 2014, 35, 4678–4687 CrossRef CAS PubMed.
- S. Shen, H. Tang, X. Zhang, J. Ren, Z. Pang, D. Wang, H. Gao, Y. Qian, X. Jiang and W. Yang, Biomaterials, 2013, 34, 3150–3158 CrossRef CAS PubMed.
- Y. Tao, E. Ju, Z. Liu, K. Dong, J. Ren and X. Qu, Biomaterials, 2014, 35, 6646–6656 CrossRef CAS PubMed.
- W.-S. Kuo, Y.-T. Chang, K.-C. Cho, K.-C. Chiu, C.-H. Lien, C.-S. Yeh and S.-J. Chen, Biomaterials, 2012, 33, 3270–3278 CrossRef CAS PubMed.
- R. Chen, X. Wang, X. Yao, X. Zheng, J. Wang and X. Jiang, Biomaterials, 2013, 34, 8314–8322 CrossRef CAS PubMed.
- E. Fischer and F. Varga, Acta Physiol. Acad. Sci. Hung., 1978, 54, 89–94 Search PubMed.
- B. Wang, J.-H. Wang, Q. Liu, H. Huang, M. Chen, K. Li, C. Li, X.-F. Yu and P. K. Chu, Biomaterials, 2014, 35, 1954–1966 CrossRef CAS PubMed.
- A. R. Kim, S. W. Shin, S. W. Cho, J. Y. Lee, D. I. Kim and S. H. Um, Adv. Healthcare Mater., 2013, 2, 1252–1258 CrossRef CAS PubMed.
- K. W. Hu, C. C. Huang, J. R. Hwu, W. C. Su, D. B. Shieh and C. S. Yeh, Chem.–Eur. J., 2008, 14, 2956–2964 CrossRef CAS PubMed.
- M. Ma, H. Chen, Y. Chen, X. Wang, F. Chen, X. Cui and J. Shi, Biomaterials, 2012, 33, 989–998 CrossRef CAS PubMed.
- G. von Maltzahn, J.-H. Park, A. Agrawal, N. K. Bandaru, S. K. Das, M. J. Sailor and S. N. Bhatia, Cancer Res., 2009, 69, 3892–3900 CrossRef CAS PubMed.
- J. H. Park, G. von Maltzahn, L. L. Ong, A. Centrone, T. A. Hatton, E. Ruoslahti, S. N. Bhatia and M. J. Sailor, Adv. Mater., 2010, 22, 880–885 CrossRef CAS PubMed.
- P. Huang, L. Bao, C. Zhang, J. Lin, T. Luo, D. Yang, M. He, Z. Li, G. Gao and B. Gao, Biomaterials, 2011, 32, 9796–9809 CrossRef CAS PubMed.
- C. Wang, J. Chen, T. Talavage and J. Irudayaraj, Angew. Chem., 2009, 121, 2797–2801 CrossRef.
- Y. Zhong, C. Wang, L. Cheng, F. Meng, Z. Zhong and Z. Liu, Biomacromolecules, 2013, 14, 2411–2419 CrossRef CAS PubMed.
- L. Tong, Y. Zhao, T. B. Huff, M. N. Hansen, A. Wei and J. X. Cheng, Adv. Mater., 2007, 19, 3136–3141 CrossRef CAS PubMed.
- T. B. Huff, L. Tong, Y. Zhao, M. N. Hansen, J.-X. Cheng and A. Wei, Nanomedicine, 2007, 2, 125–132 CrossRef CAS PubMed.
- Z. Zhang, L. Wang, J. Wang, X. Jiang, X. Li, Z. Hu, Y. Ji, X. Wu and C. Chen, Adv. Mater., 2012, 24, 1418–1423 CrossRef CAS PubMed.
- Y. T. Chang, P. Y. Liao, H. S. Sheu, Y. J. Tseng, F. Y. Cheng and C. S. Yeh, Adv. Mater., 2012, 24, 3309–3314 CrossRef CAS PubMed.
- X. Yang, Z. Liu, Z. Li, F. Pu, J. Ren and X. Qu, Chem.–Eur. J., 2013, 19, 10388–10394 CrossRef CAS PubMed.
- Z. Li, P. Huang, X. Zhang, J. Lin, S. Yang, B. Liu, F. Gao, P. Xi, Q. Ren and D. Cui, Mol. Pharmaceutics, 2009, 7, 94–104 CrossRef PubMed.
- Y.-F. Huang, K. Sefah, S. Bamrungsap, H.-T. Chang and W. Tan, Langmuir, 2008, 24, 11860–11865 CrossRef CAS PubMed.
- V. Raji, J. Kumar, C. Rejiya, M. Vibin, V. N. Shenoi and A. Abraham, Exp. Cell Res., 2011, 317, 2052–2058 CrossRef CAS PubMed.
- Y. Shen, H. Tang, Y. Zhan, E. A. Van Kirk and W. J. Murdoch, Nanomedicine: Nanotechnology, Biology and Medicine, 2009, 5, 192–201 CrossRef CAS PubMed.
- J. F. Hainfeld, L. Lin, D. N. Slatkin, F. A. Dilmanian, T. M. Vadas and H. M. Smilowitz, Nanomedicine: Nanotechnology, Biology and Medicine, 2014, 10, 1609–1617 CrossRef CAS PubMed.
- I. H. El-Sayed, X. Huang and M. A. El-Sayed, Cancer Lett., 2006, 239, 129–135 CrossRef CAS PubMed.
- Y. Jin, J. Wang, H. Ke, S. Wang and Z. Dai, Biomaterials, 2013, 34, 4794–4802 CrossRef CAS PubMed.
- V. Cebrián, F. Martín-Saavedra, L. Gómez, M. Arruebo, J. Santamaria and N. Vilaboa, Nanomedicine: Nanotechnology, Biology and Medicine, 2013, 9, 646–656 CrossRef PubMed.
- E. S. Day, P. A. Thompson, L. Zhang, N. A. Lewinski, N. Ahmed, R. A. Drezek, S. M. Blaney and J. L. West, J. Neuro-Oncol., 2011, 104, 55–63 CrossRef CAS PubMed.
- N. Manuchehrabadi, R. Toughiri, C. Bieberich, H. Cai, A. Attaluri, R. Edziah, E. Lalanne, A. M. Johnson, R. Ma and L. Zhu, Int. J. Biomed. Eng. Technol., 2013, 12, 157–176 CrossRef.
- I. L. Maksimova, G. G. Akchurin, G. S. Terentyuk, B. N. Khlebtsov, G. Akchurin, I. A. e. Ermolaev, A. Skaptsov, E. Revzina, V. V. Tuchin and N. G. e. Khlebtsov, Quantum Electron., 2008, 38, 536–542 CrossRef CAS.
- C. Wu, C. Yu and M. Chu, Int. J. Nanomed., 2011, 6, 807 CAS.
- H. Ke, J. Wang, Z. Dai, Y. Jin, E. Qu, Z. Xing, C. Guo, X. Yue and J. Liu, Angew. Chem., 2011, 123, 3073–3077 CrossRef.
- C. Loo, A. Lowery, N. Halas, J. West and R. Drezek, Nano Lett., 2005, 5, 709–711 CrossRef CAS PubMed.
- H. Xie, P. Diagaradjane, A. A. Deorukhkar, B. Goins, A. Bao, W. T. Phillips, Z. Wang, J. Schwartz and S. Krishnan, Int. J. Nanomed., 2011, 6, 259 CrossRef CAS PubMed.
- M. P. Melancon, A. M. Elliott, A. Shetty, Q. Huang, R. J. Stafford and C. Li, J. Controlled Release, 2011, 156, 265–272 CrossRef CAS PubMed.
- W. Lu, C. Xiong, G. Zhang, Q. Huang, R. Zhang, J. Z. Zhang and C. Li, Clin. Cancer Res., 2009, 15, 876–886 CrossRef CAS PubMed.
- R. Fekrazad, N. Hakimiha, E. Farokhi, M. J. Rasaee, M. S. Ardestani, K. A. Kalhori and F. Sheikholeslami, Int. J. Nanomed., 2011, 6, 2749 CAS.
- W. Lu, M. P. Melancon, C. Xiong, Q. Huang, A. Elliott, S. Song, R. Zhang, L. G. Flores, J. G. Gelovani and L. V. Wang, Cancer Res., 2011, 71, 6116–6121 CrossRef CAS PubMed.
- L. Cheng, K. Yang, Y. Li, X. Zeng, M. Shao, S.-T. Lee and Z. Liu, Biomaterials, 2012, 33, 2215–2222 CrossRef CAS PubMed.
- W. Dong, Y. Li, D. Niu, Z. Ma, J. Gu, Y. Chen, W. Zhao, X. Liu, C. Liu and J. Shi, Adv. Mater., 2011, 23, 5392–5397 CrossRef CAS PubMed.
- W.-S. Kuo, C.-M. Wu, Z.-S. Yang, S.-Y. Chen, C.-Y. Chen, C.-C. Huang, W.-M. Li, C.-K. Sun and C.-S. Yeh, Chem. Commun., 2008, 4430–4432 RSC.
- T. T. Nhung, Y. Bu and S.-W. Lee, J. Cryst. Growth, 2013, 373, 132–137 CrossRef CAS.
- K. Winkler, A. Kaminska, T. Wojciechowski, R. Holyst and M. Fialkowski, Plasmonics, 2011, 6, 697–704 CrossRef CAS PubMed.
- P. Forrer, F. Schlottig, H. Siegenthaler and M. Textor, J. Appl. Electrochem., 2000, 30, 533–541 CrossRef CAS.
- K. W. Hu, C. C. Huang, J. R. Hwu, W. C. Su, D. B. Shieh and C. S. Yeh, Chem.–Eur. J., 2008, 14, 2956–2964 CrossRef CAS PubMed.
- C. Burda, X. Chen, R. Narayanan and M. A. El-Sayed, Chem. Rev., 2005, 105, 1025–1102 CrossRef CAS PubMed.
- J. Xie, Q. Zhang, J. Y. Lee and D. I. Wang, ACS Nano, 2008, 2, 2473–2480 CrossRef CAS PubMed.
- Y. Jiang, X.-J. Wu, Q. Li, J. Li and D. Xu, Nanotechnology, 2011, 22, 385601 CrossRef PubMed.
- J. Han, J. Li, W. Jia, L. Yao, X. Li, L. Jiang and Y. Tian, Int. J. Nanomed., 2014, 9, 517 CrossRef PubMed.
- P. Huang, O. Pandoli, X. Wang, Z. Wang, Z. Li, C. Zhang, F. Chen, J. Lin, D. Cui and X. Chen, Nano Res., 2012, 5, 630–639 CrossRef CAS.
- S. Wang, P. Huang, L. Nie, R. Xing, D. Liu, Z. Wang, J. Lin, S. Chen, G. Niu and G. Lu, Adv. Mater., 2013, 25, 3055–3061 CrossRef CAS PubMed.
- S. E. Skrabalak, J. Chen, Y. Sun, X. Lu, L. Au, C. M. Cobley and Y. Xia, Acc. Chem. Res., 2008, 41, 1587–1595 CrossRef CAS PubMed.
- L. Wang, J. Shi, H. Zhang, H. Li, Y. Gao, Z. Wang, H. Wang, L. Li, C. Zhang and C. Chen, Biomaterials, 2013, 34, 262–274 CrossRef CAS PubMed.
- L. Wang, J. Shi, X. Jia, R. Liu, H. Wang, Z. Wang, L. Li, J. Zhang, C. Zhang and Z. Zhang, Pharm. Res., 2013, 30, 2757–2771 CrossRef CAS PubMed.
- S. A. Khan, R. Kanchanapally, Z. Fan, L. Beqa, A. K. Singh, D. Senapati and P. C. Ray, Chem. Commun., 2012, 48, 6711–6713 RSC.
- J.-G. Piao, L. Wang, F. Gao, Y.-Z. You, Y. Xiong and L. Yang, ACS Nano, 2014, 8, 10414–10425 CrossRef CAS PubMed.
- F. Hao, C. L. Nehl, J. H. Hafner and P. Nordlander, Nano Lett., 2007, 7, 729–732 CrossRef CAS PubMed.
- S. Liang, C. Li, C. Zhang, Y. Chen, L. Xu, C. Bao and X. Wang, Theranostics, 2015, 5, 970 CrossRef CAS PubMed.
- C. Kim, H.-M. Song, X. Cai, J. Yao, A. Wei and L. V. Wang, J. Mater. Chem., 2011, 21, 2841–2844 RSC.
- R. Vankayala, Y. K. Huang, P. Kalluru, C. S. Chiang and K. C. Hwang, Small, 2014, 10, 1612–1622 CrossRef CAS PubMed.
- M. Olivo, S. S. Lucky, R. Bhuvaneswari and N. Dendukuri, European Conferences on Biomedical Optics, 2011, 80870T Search PubMed.
- L. Wang, D. Meng, Y. Hao, Y. Zhao, D. Li, B. Zhang, Y. Zhang and Z. Zhang, J. Biomater. Appl., 2015, 30, 547–557 CrossRef CAS PubMed.
- Y. Liu, Z. Chang, H. Yuan, A. M. Fales and T. Vo-Dinh, Nanoscale, 2013, 5, 12126–12131 RSC.
- Y. Liu, J. R. Ashton, E. J. Moding, H. Yuan, J. K. Register, A. M. Fales, J. Choi, M. J. Whitley, X. Zhao and Y. Qi, Theranostics, 2015, 5, 946–960 CrossRef CAS PubMed.
- J. O. You, P. Guo and D. T. Auguste, Angew. Chem., Int. Ed., 2013, 52, 4141–4146 CrossRef CAS PubMed.
- L. Au, D. Zheng, F. Zhou, Z.-Y. Li, X. Li and Y. Xia, ACS Nano, 2008, 2, 1645–1652 CrossRef CAS PubMed.
- X. Liu, Y. Chen, H. Li, N. Huang, Q. Jin, K. Ren and J. Ji, ACS Nano, 2013, 7, 6244–6257 CrossRef CAS PubMed.
- L. Cheng, K. Yang, Y. Li, J. Chen, C. Wang, M. Shao, S. T. Lee and Z. Liu, Angew. Chem., 2011, 123, 7523–7528 CrossRef.
- J. Chen, C. Glaus, R. Laforest, Q. Zhang, M. Yang, M. Gidding, M. J. Welch and Y. Xia, Small, 2010, 6, 811–817 CrossRef CAS PubMed.
- W. Lu, A. K. Singh, S. A. Khan, D. Senapati, H. Yu and P. C. Ray, J. Am. Chem. Soc., 2010, 132, 18103–18114 CrossRef CAS PubMed.
- J. Chen, D. Wang, J. Xi, L. Au, A. Siekkinen, A. Warsen, Z.-Y. Li, H. Zhang, Y. Xia and X. Li, Nano Lett., 2007, 7, 1318–1322 CrossRef CAS PubMed.
- J.-L. Li, L. Wang, X.-Y. Liu, Z.-P. Zhang, H.-C. Guo, W.-M. Liu and S.-H. Tang, Cancer Lett., 2009, 274, 319–326 CrossRef CAS PubMed.
- H. Yuan, C. G. Khoury, C. M. Wilson, G. A. Grant, A. J. Bennett and T. Vo-Dinh, Nanomedicine, 2012, 8, 1355–1363 CAS.
- C. P. Liu, F. S. Lin, C. T. Chien, S. Y. Tseng, C. W. Luo, C. H. Chen, J. K. Chen, F. G. Tseng, Y. Hwu and L. W. Lo, Macromol. Biosci., 2013, 13, 1314–1320 CrossRef CAS PubMed.
- J. Lee, J. Yang, H. Ko, S. Oh, J. Kang, J. Son, K. Lee, S.-W. Lee, H.-G. Yoon and J.-S. Suh, Adv. Funct. Mater., 2008, 18, 258–264 CrossRef CAS.
- S. J. Leung and M. Romanowski, ACS Nano, 2012, 6, 9383–9391 CrossRef CAS PubMed.
- J. Nam, N. Won, H. Jin, H. Chung and S. Kim, J. Am. Chem. Soc., 2009, 131, 13639–13645 CrossRef CAS PubMed.
- J. Lin, S. Wang, P. Huang, Z. Wang, S. Chen, G. Niu, W. Li, J. He, D. Cui and G. Lu, ACS Nano, 2013, 7, 5320–5329 CrossRef CAS PubMed.
- J. Nam, W.-G. La, S. Hwang, Y. S. Ha, N. Park, N. Won, S. Jung, S. H. Bhang, Y.-J. Ma and Y.-M. Cho, ACS Nano, 2013, 7, 3388–3402 CrossRef CAS PubMed.
- Y.-L. Luo, Y.-S. Shiao and Y.-F. Huang, ACS Nano, 2011, 5, 7796–7804 CrossRef CAS PubMed.
- J. He, X. Huang, Y.-C. Li, Y. Liu, T. Babu, M. A. Aronova, S. Wang, Z. Lu, X. Chen and Z. Nie, J. Am. Chem. Soc., 2013, 135, 7974–7984 CrossRef CAS PubMed.
- J. Yang, D. Shen, L. Zhou, W. Li, X. Li, C. Yao, R. Wang, A. M. El-Toni, F. Zhang and D. Zhao, Chem. Mater., 2013, 25, 3030–3037 CrossRef CAS.
- H. Yuan, A. M. Fales and T. Vo-Dinh, J. Am. Chem. Soc., 2012, 134, 11358–11361 CrossRef CAS PubMed.
- V. Pustovalov, A. Smetannikov and V. Zharov, Laser Phys. Lett., 2008, 5, 775 CrossRef CAS.
- H. Takahashi, T. Niidome, A. Nariai, Y. Niidome and S. Yamada, Chem. Lett., 2006, 35, 500–501 CrossRef CAS.
- H. Takahashi, T. Niidome, A. Nariai, Y. Niidome and S. Yamada, Nanotechnology, 2006, 17, 4431 CrossRef CAS.
- A. Sibille, C. D'alincourt, T. Ponchon, F. Berger and R. Lambert, J. Phys. IV, 1994, 4, C4-C211–C4-C214 Search PubMed.
- A. Sibille, T. Ponchon, F. Berger and R. Lambert, Laser. Med. Sci., 1995, 10, 47–53 CrossRef.
- J. L. Compton, A. N. Hellman and V. Venugopalan, Biophys. J., 2013, 105, 2221–2231 CrossRef CAS PubMed.
- X. Huang, B. Kang, W. Qian, M. A. Mackey, P. C. Chen, A. K. Oyelere, I. H. El-Sayed and M. A. El-Sayed, J. Biomed. Opt., 2010, 15, 058002–058007 CrossRef PubMed.
- M. Ganguly and K. Mitra, Analyzing Thermal and Mechanical Effects of Pulsed Laser Irradiation on Tissues, in ICHMT Digital Library Online, Begel House Inc., 2015 Search PubMed.
- J.-L. Li and M. Gu, Biomaterials, 2010, 31, 9492–9498 CrossRef CAS PubMed.
- V. V. Klimenko, N. A. Knyazev, F. V. Moiseenko, A. A. Rusanov, A. A. Bogdanov and M. V. Dubina, Photodiagn. Photodyn. Ther., 2016, 13, 101–107 CrossRef CAS PubMed.
- V. P. Zharov, E. Galitovskaya and M. Viegas, Proc. SPIE, 2004, 5319, 291–300 CrossRef CAS.
- M. G. B. Ashiq, M. A. Saeed, B. A. Tahir, N. Ibrahim and M. Nadeem, Chin. J. Cancer Res., 2013, 25, 756 Search PubMed.
- V. P. Zharov, E. N. Galitovskaya, C. Johnson and T. Kelly, Lasers Surg. Med., 2005, 37, 219–226 CrossRef PubMed.
- V. Zharov, R. Letfullin and E. Galitovskaya, J. Phys. D: Appl. Phys., 2005, 38, 2571 CrossRef CAS.
- E. Y. Hleb, J. H. Hafner, J. N. Myers, E. Y. Hanna, B. C. Rostro, S. A. Zhdanok and D. O. Lapotko, Nanomedicine, 2008, 3, 647–667 CrossRef CAS PubMed.
- C. M. Pitsillides, E. K. Joe, X. Wei, R. R. Anderson and C. P. Lin, Biophys. J., 2003, 84, 4023–4032 CrossRef CAS PubMed.
- N. Nedyalkov, S. Imamova, P. Atanasov, R. Toshkova, E. Gardeva, L. Yossifova, M. Alexandrov and M. Obara, Appl. Surf. Sci., 2011, 257, 5456–5459 CrossRef CAS.
- V. P. Zharov, K. E. Mercer, E. N. Galitovskaya and M. S. Smeltzer, Biophys. J., 2006, 90, 619–627 CrossRef CAS PubMed.
- Y. Wang, K. C. Black, H. Luehmann, W. Li, Y. Zhang, X. Cai, D. Wan, S.-Y. Liu, M. Li and P. Kim, ACS Nano, 2013, 7, 2068–2077 CrossRef CAS PubMed.
- S. Kessentini and D. Barchiesi, Progress In Electromagnetics Research Symposium Proceedings, 2013 Search PubMed.
- W.-C. Huang, P.-J. Tsai and Y.-C. Chen, Nanomedicine, 2007, 2, 777–787 CrossRef CAS PubMed.
- R. S. Norman, J. W. Stone, A. Gole, C. J. Murphy and T. L. Sabo-Attwood, Nano Lett., 2008, 8, 302–306 CrossRef CAS PubMed.
- S. Wang, A. K. Singh, D. Senapati, A. Neely, H. Yu and P. C. Ray, Chem.–Eur. J., 2010, 16, 5600–5606 CrossRef CAS PubMed.
- L. A. Mermel, B. M. Farr, R. J. Sherertz, I. I. Raad, N. O'Grady, J. S. Harris and D. E. Craven, Infect. Contr. Hosp. Epidemiol., 2001, 22, 222–242 CAS.
- S. Fletcher, Cont. Educ. Anaesth. Crit. Care Pain, 2005, 5, 49–51 CrossRef.
- K. Mozaffari, H. Bakhshandeh, H. Khalaj and H. Soudi, Res Cardiovasc Med, 2013, 2, 99 CrossRef PubMed.
- O. Khantamat, C.-H. Li, F. Yu, A. C. Jamison, W.-C. Shih, C. Cai and T. R. Lee, ACS Appl. Mater. Interfaces, 2015, 7, 3981–3993 CAS.
- B. Hu, N. Wang, L. Han, M.-L. Chen and J.-H. Wang, Acta Biomater., 2015, 11, 511–519 CrossRef CAS PubMed.
- K. Turcheniuk, C.-H. Hage, J. Spadavecchia, A. Y. Serrano, I. Larroulet, A. Pesquera, A. Zurutuza, M. G. Pisfil, L. Héliot and J. Boukaert, J. Mater. Chem. B, 2015, 3, 375–386 RSC.
- M. Ramasamy, S. S. Lee, D. K. Yi and K. Kim, J. Mater. Chem. B, 2014, 2, 981–988 RSC.
- Z. Fan, D. Senapati, S. A. Khan, A. K. Singh, A. Hamme, B. Yust, D. Sardar and P. C. Ray, Chem.–Eur. J., 2013, 19, 2839–2847 CrossRef CAS PubMed.
- R. Shokri, M. Salouti and R. S. Zanjani, J. Microbiol., 2015, 53, 116–121 CrossRef CAS PubMed.
- K. C. Black, T. S. Sileika, J. Yi, R. Zhang, J. G. Rivera and P. B. Messersmith, Small, 2014, 10, 169–178 CrossRef CAS PubMed.
- B. Hu, L.-P. Zhang, X.-W. Chen and J.-H. Wang, Nanoscale, 2013, 5, 246–252 RSC.
- B. Khlebtsov, E. Tuchina, V. Tuchin and N. Khlebtsov, RSC Adv., 2015, 5, 61639–61649 RSC.
- W. C. Huang, P. J. Tsai and Y. C. Chen, Small, 2009, 5, 51–56 CrossRef CAS PubMed.
- X. Dai, Z. Fan, Y. Lu and P. C. Ray, ACS Appl. Mater. Interfaces, 2013, 5, 11348–11354 CAS.
- N. J. Millenbaugh, J. B. Baskin, M. N. DeSilva, W. R. Elliott and R. D. Glickman, Int. J. Nanomed., 2015, 10, 1953 CrossRef CAS PubMed.
- L. Mocan, I. Ilie, C. Matea, F. Tabaran, E. Kalman, C. Iancu and T. Mocan, IInt. J. Nanomed., 2014, 9, 1453 CrossRef PubMed.
- Y. Lin and A. T. Hamme II, Analyst, 2014, 139, 3702–3705 RSC.
| This journal is © The Royal Society of Chemistry 2016 |