Inulin ameliorates schizophrenia via modulation of the gut microbiota and anti-inflammation in mice†
Abstract
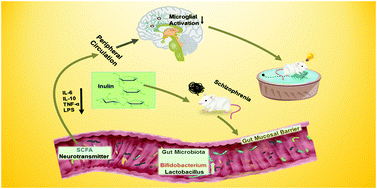
The microbiome–gut–brain (MGB) axis, which regulates neurological and cognitive functions, plays an essential role in schizophrenia (SCZ) progression. Dietary inulin could be a novel strategy for the treatment of SCZ due to its modulating effects on the gut microbiota. In this study, the effects of inulin on mice with SCZ were studied. As indicated by the behavioural tests, expression of neurotransmitters, inflammatory indicators, and brain morphology, inulin administration ameliorated aberrant behaviours (locomotor hypoactivity, anxiety disorders and depressive behaviours, and impaired learning and spatial recognition memory) and effectively reduced neuroinflammation and neuronal damage. In addition, inulin improved intestinal integrity and permeability, as indicated by the elevated expression of tight junction proteins (p < 0.05). The results of 16S rRNA sequencing and analysis showed that inulin increased the abundance of Lactobacillus and Bifidobacterium, which were negatively correlated with 5-hydroxytryptamine and inflammatory cytokines and positively correlated with brain-derived neurotrophic factor (BDNF). Inulin caused a reduction in Akkermansia that was positively correlated with inflammatory cytokines and negatively correlated with BDNF. These results suggested that dietary inulin modulated the gut microbiota and exerted anti-inflammatory effects in mice though the MGB axis, which further ameliorated SCZ. Therefore, the results of this study provide a potential explanation for inulin intervention in the treatment of SCZ.


 Please wait while we load your content...
Please wait while we load your content...