Application of a bilayer tubular scaffold based on electrospun poly(l-lactide-co-caprolactone)/collagen fibers and yarns for tracheal tissue engineering†
Abstract
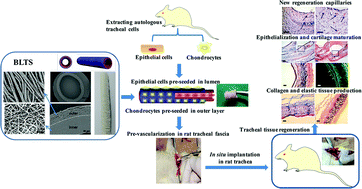
A bilayer tubular scaffold (BLTS) consisting of poly(L-lactide-co-caprolactone) (P(LLA–CL))/collagen submicron sized fibers and micron sized yarns, was prepared via electrospinning. Then, autologous tracheal epithelial cells and chondrocytes were separately seeded onto the two layers of the BLTS. After culturing for 7 days, the cell-seeded BLTS (CS-BLTS) was implanted and wrapped in rat tracheal fascia for pre-vascularization. The pre-vascularized BLTS (PV-BLTS) was subjected to an in situ trachea regeneration study using a rat trachea injury model, along with CS-BLTS and bare BLTS for comparison. The results presented the bilayer structure of the BLTS, and the two layers were arranged conterminously. The porosity of the outer layer (collagen/P(LLA–CL) yarns) was found to be significantly higher (P < 0.05) than that of the inner layer (collagen/P(LLA–CL) fibers). In vitro biological analysis demonstrated that the collagen/P(LLA–CL) showed good biocompatibility, which promoted tracheal epithelial cell initial adhesion and proliferation with a highly significant difference (P < 0.001) or significant difference (P < 0.05) compared to those of pure P(LLA–CL) materials respectively. Chondrocyte activity and proliferation were also enhanced on collagen/P(LLA–CL) yarns with a significant difference (P < 0.05) compared to those of pure P(LLA–CL). Chondrocyte penetration was promoted as well, due to the loose and porous structure of the electrospun collagen/P(LLA–CL) yarns. The in vivo evaluation results of immune response analysis and histological investigation demonstrated that the PV-BLTS performed better in new capillary regeneration, reducing immunogenicity and improving tracheal tissue regeneration compared to the CS-BLTS and bare BLTS, indicating its promising potential as a new tissue engineered alternative for trachea repair and regeneration.


 Please wait while we load your content...
Please wait while we load your content...